Table of Contents |
Urine formation happens in three stages.
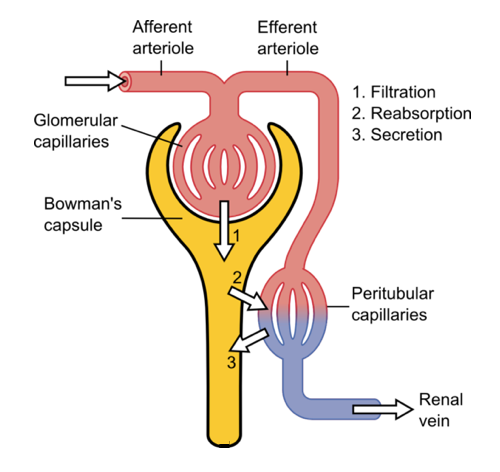
Filtration is the first step in urine production, and this process of urine formation ensures that only necessary products are excreted from the body.
Filtration only occurs within a specific part of the nephron, the Bowman's capsule. During filtration, blood enters the capillaries within the Bowman's capsule, called the glomerulus or glomeruli, through the afferent arteriole, which is narrow compared to other blood vessels within the body. Because of this, blood is delivered towards the nephron through the afferent at high pressure due to the more narrow diameter these arterioles have. This high pressure will force water and solutes from the blood in these afferent arterioles, into the Bowman's capsule of the nephron.
The solutes that are forced out of the blood include glucose, sodium, urea, vitamins, amino acids, et cetera. Water and solutes that are pushed out of the blood would then flow into the proximal tubule, where the next stage of urine formation occurs: Reabsorption.
Reabsorption is the second step in urine formation and is sometimes referred to as tubular reabsorption. In this step of urine formation, water and solutes that have been filtered from blood in the first step, filtration, move throughout the rest of the nephron. Water and other solutes sometimes are very valuable, and our body needs to retain them. These water and solutes need to be reabsorbed back into blood so the body can retain them.
Reabsorption primarily takes place across the walls of the proximal tubules. The walls of the proximal tubule are very thin, about one cell thick. Solutes and water will leak out or be pumped out of nephron tubules and will then be reabsorbed into peritubular capillaries.
Peritubular capillaries interweave within the nephron, and from there, they will return solutes to the bloodstream. Any remaining solutes that weren't reabsorbed from the nephron tubules into the bloodstream will become a part of urine.
Tubular secretion starts at the proximal tubule, and then it'll occur at the other tubular parts of the nephron as it moves through. Substances such as hydrogen, potassium, and urea at this point will move from the peritubular capillaries into nephron tubules, joining with forming urine.
In reabsorption, water and extra solutes that haven't been reabsorbed back into the blood will become a part of urine. Hydrogen, potassium, and urea from the peritubular capillaries will join with them, forming urine. Urine will then move toward the collecting duct, which will then move the formed urine into the ureters, and then the urinary bladder.
Secretion helps to maintain the body's acid-base balance and makes sure that substances don't build up in the blood. It starts at the proximal tubule and will work its way down through the loop of Henle and distal tubule.
To better understand, take a look at the diagram below:
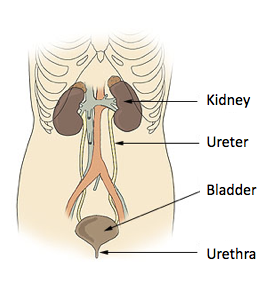
The kidney is where the nephrons are located. The nephrons produce urine and carry it to the collecting ducts. Collecting ducts move urine to the renal pelvis of the kidney, which funnels it into the ureter. Ureters will then funnel that urine down to the urinary bladder where it will be stored until it's excreted through the urethra. The urethra connects the urinary bladder to the outside, as urine is excreted. When urine is expelled from the urinary bladder through the urethra to the outside, we call it urination, which is a reflex response.
As the bladder fills with urine that it's storing, the tension across the muscles of the urinary bladder will increase, causing the internal sphincter to relax. The bladder will then contract, or shorten, forcing urine out through the urethra.
 Investigate the urinary system in three dimensions using augmented reality (AR)!
Investigate the urinary system in three dimensions using augmented reality (AR)!