Table of Contents |
The way that addiction is viewed has changed significantly in many ways over the past decades. At the turn of the 20th century, people with addictions were viewed as having moral shortcomings and weak willpower and were often separated from society rather than receiving treatment (Herron & Brennan, 2020). Starting in the 1970s, brain imaging studies demonstrated that addictions change the brain, helping dispel the stigma that addiction is a matter of morals and willpower. However, stigma and misconceptions about addictions persist today, with people mistakenly thinking that people can stop addictive behaviors simply by choosing to do so. In reality, addiction is a complex disease of the brain, and quitting an addiction usually takes more than good intentions or willpower. Addictions change the brain in ways that make quitting hard, even for those who are ready and willing to quit.
According to the National Institute on Drug Abuse, addiction is defined as a chronic disease characterized by seeking and use that is compulsive, or difficult to control, despite harmful consequences. More specifically, addictions are characterized by three cycles (Herron & Brennan, 2020):
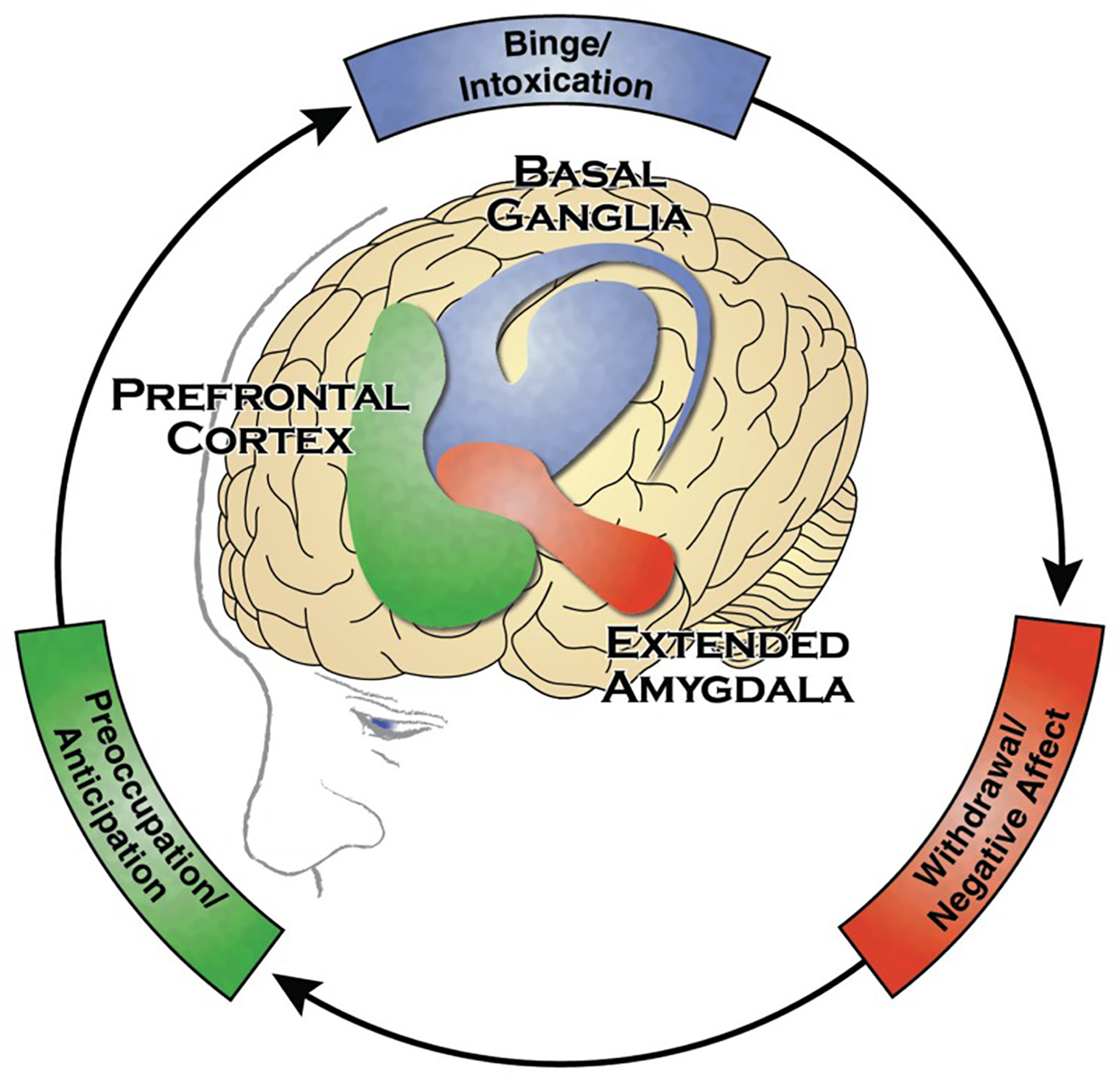
IN CONTEXT
In the lesson titled “Mental Health”, you learned about the value of person-first language in avoiding stigma. This is important in the context of addiction, as stigma can reinforce negative stereotypes and prevent people from seeking treatment (National Institute on Drug Abuse, 2021). Some examples of person-first language in addiction contexts include the following:
- “Person with a substance use disorder” rather than an “addict” or a “drug user”
- “Drug use” or “drug misuse” rather than “drug abuse”
- “Person with an alcohol use disorder” rather than an “alcoholic”
- “Person with a gambling disorder” rather than a “problem gambler”
- “Person in recovery” rather than “a former addict”
The human brain is an extraordinarily complex and fine-tuned communications network made up of billions of cells that govern our thoughts, emotions, perceptions, and drives. Our brains reward certain behaviors such as eating or procreating—registering these as pleasurable activities that we want to repeat. Addiction taps into these vital mechanisms geared for our survival. Although not a life necessity, to a person with an addiction, the addiction becomes life itself, driving compulsive use—even in the face of dire life consequences.
Most drugs or behavioral addictions affect the brain’s “reward circuit” by flooding it with the chemical messenger dopamine. This reward system controls the body’s ability to feel pleasure and motivates a person to repeat behaviors needed to thrive, such as eating and spending time with loved ones. This overstimulation of the reward circuit causes the intensely pleasurable “high” that can lead people to take a drug again and again. Some drugs can cause up to 10 times the amount of dopamine as natural rewards, like eating. As a person continues to use drugs, the brain adjusts to the excess dopamine by making less of it and/or reducing the ability of cells in the reward circuit to respond to it. The person might take more of the drug, trying to achieve the same dopamine high. It can also cause less pleasure from non-drug behaviors, like food or social activities. This reaction sets in motion a reinforcing pattern that “teaches” people to repeat the rewarding behavior of abusing drugs.
Long-term drug use also disrupts the brain circuits involved in memory and control over behavior. Memories of the drug experience can trigger craving as can exposure to people, places, or things associated with former drug use. An area of the brain called the frontal cortical region is responsible for actions such as planning and decision-making, and drug use can affect this region (Herron & Brennan, 2020). The frontal cortical region is also one of the last brain areas to mature, making teenagers particularly vulnerable to the effects of drugs on the brain. The regions of the brain that exert control over desires and emotions are affected when a person has an addiction, compromising their behavior.
When does drug use become drug addiction? It rarely happens with the first use of a drug. Drug use and drug addiction can be thought of as points along a continuum. Any use of a mind-altering drug or the inappropriate use of medication (either prescription or over-the-counter drugs) is potentially problematic use, but the point at which this becomes drug addiction is less clear. Different people may reach the point of addiction at different stages, and research is ongoing as to the nature of addiction.
No single factor can predict whether a person will become addicted to drugs. The risk for addiction is influenced by a combination of factors that include individual biology, social environment, and age or stage of development. The more risk factors an individual has, the greater the chance that taking drugs can lead to addiction. Consider the following risk factors:
In addition to drugs, behaviors can also promote the qualities of addiction. Research suggests that behaviors that produce the same types of short-term reward effects in the brain can make a person want to continue engaging with the behaviors, even when negative consequences result (Grant et al., 2010). However, the main difference with behavioral addiction is that the person is driven by the feelings associated with the behavior rather than using a substance (Alavi et al., 2012).
Some common types of behavioral addictions are gambling, internet-related addictions such as video gaming or internet use, exercise addiction, shopping addiction, and sex addiction. Doing a behavior regularly because it makes you feel good or is a habit is not an addiction. However, a behavior becomes an addiction when it goes beyond being a habit and becomes an obligation or compulsion, leading to problems functioning in everyday life, such as at work or in social situations (Alavi et al., 2012).
EXAMPLE
Exercise is a positive behavior with many physical and mental health benefits, as you’ve learned. Many people make exercise a daily part of their routine because of these benefits, and some people training for specific goals, like running a marathon, will devote significant amounts of time to exercise, likely sacrificing other activities. However, behaviors begin crossing the line into addiction when the behavior becomes the most important activity in a person’s life, dominating their thoughts, feelings, and behavior, and leading to conflicts with others (Griffiths, 1996). Like drug addiction, the aspects of tolerance and withdrawal can also occur with behavioral addictions.You’ve learned about the DSM-V as the authoritative resource for diagnosing mental health disorders and sleep disorders, and the DSM-V is also used for diagnoses related to addiction. The DSM-V first recognized gambling disorder as a behavioral addiction but does not officially recognize all the behaviors listed above as behavioral addictions. However, it’s important to consider that even if a behavior doesn’t fit all the criteria for addiction, it can still cause negative effects from being done compulsively. Research on technology use, like the internet and cell phones, explains that technology uses impulses, such as wanting to check email or browse social media (Eyal, 2014). These impulses can then turn into compulsions where we end up spending significant amounts of time on the behavior, detracting from other activities that are worthwhile to us.
Source: THIS TUTORIAL HAS BEEN ADAPTED FROM (1) “WELLNESS” BY EXTENDED LEARNING INSTITUTE (ELI) AT NOVA. ACCESS FOR FREE AT oer commons. LICENSING: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.
Disclaimer: The use of any CDC and United States government materials, including any links to the materials on the CDC or government websites, does not imply endorsement by the CDC or the United States government of us, our company, product, facility, service, or enterprise.
REFERENCES
Eyal, N. (2014). Hooked: How to build habit-forming products. Penguin. ISBN: 9781591847786.
Grant, J. E., Potenza, M. N., Weinstein, A., & Gorelick, D. A. (2010). Introduction to behavioral addictions. The American Journal of Drug and Alcohol Abuse, 36(5), 233–241. doi.org/10.3109/00952990.2010.491884
Griffiths, M. (1996). Nicotine, tobacco and addiction. Nature, 384(6604), 18-18. doi.org/10.1038/384018a0
Herron, A.J. & Brennan, T.K. (2020). The ASAM Principles of Addiction Medicine, Third Edition. Wolters Kluwer. ISBN: 9781975107956
National Institute on Drug Abuse. (2021). Words matter: preferred language for talking about addiction. National Institutes of Health. nida.nih.gov/research-topics/addiction-science/words-matter-preferred-language-talking-about-addiction