Table of Contents |
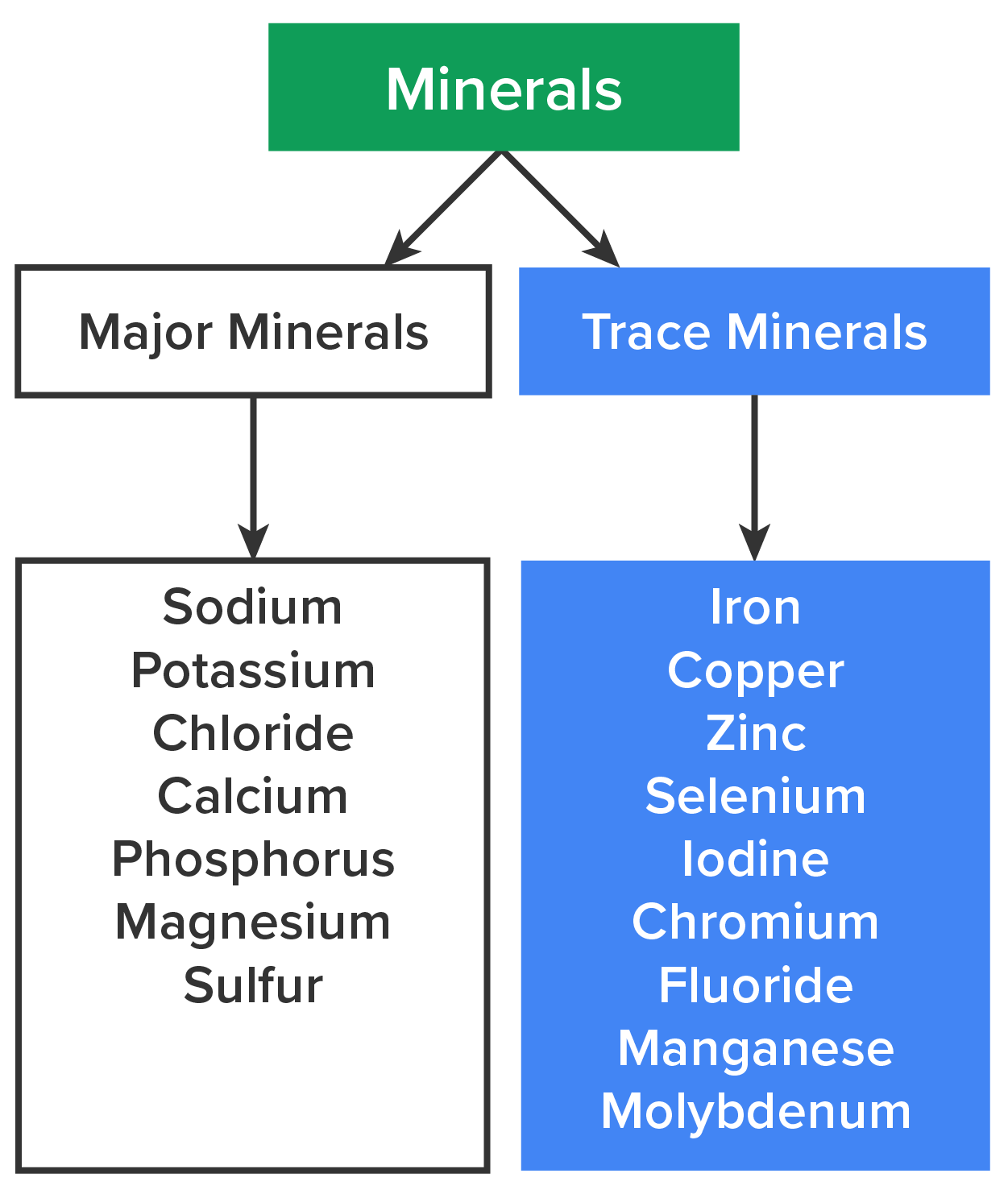
Trace minerals are classified as minerals required in the diet daily in smaller amounts, specifically 100 milligrams or less. These include copper, zinc, selenium, iodine, chromium, fluoride, manganese, molybdenum, and others. Although trace minerals are needed in smaller amounts, it is important to remember that a deficiency in a trace mineral can be just as detrimental to your health as a major mineral deficiency.
| Micronutrient | Sources | Recommended Intakes for Adults | Major Functions |
|---|---|---|---|
| Iron | Red meat, egg yolks, dark leafy vegetables, dried fruit, iron-fortified foods | 8-18 mg/day | Assists in energy production, DNA synthesis required for red blood cell function |
| Copper | Nuts, seeds, whole grains, seafood | 900 mcg/day | Assists in energy production, iron metabolism |
| Zinc | Oysters, wheat germ, pumpkin seeds, squash, beans, sesame seeds, tahini, beef, lamb | 8-11 mg/day | Assists in energy production, protein, RNA, and DNA synthesis; required for hemoglobin synthesis |
| Selenium | Meat, seafood, eggs, nuts | 55 mcg/day | Essential for thyroid hormone activity |
| Iodine | Iodized salt, seaweed, dairy products | 150 mcg/day | Making thyroid hormone, metabolism, growth and development |
| Chromium | Grape juice, ham, brewer's yeast | 25-35 mcg/day | Assists insulin in carbohydrate, lipid and protein metabolism |
| Fluoride | Fluoridated water, foods prepared in fluoridated water, seafood | 3-4 mg/day | Component of mineralized bone, provides structure and microarchitecture, stimulates new bone growth |
| Manganese | Legumes, nuts, leafy green vegetables | 1.8-2.3 mg/day | Glucose synthesis, amino-acid catabolism |
| Molybdenum | Milk, grains, legumes | 45 mcg/day | Cofactor for a number of enzymes |
| Micronutrient | Deficiency Diseases and Symptoms | Groups at Risk for Deficiency | Toxicity | UL |
|---|---|---|---|---|
| Iron | Anemia: fatigue, paleness, faster heart rate | Infants and preschool children, adolescents, women, pregnant women, athletes, vegetarians | Liver damage, increased risk of diabetes and cancer | 45 mg/day |
| Copper | Anemia: fatigue, paleness, faster heart rate | Those who consume excessive zinc supplements | Vomiting, abdominal pain, diarrhea, liver damage | 10 mg/day |
| Zinc | Delayed growth in children, hair loss, diarrhea, skin sores, loss of appetite, weight loss | Vegetarians, older adults | Depressed immune function | 40 mg/day |
| Selenium | Fatigue, muscle pain, weakness, Keshan disease | Populations where the soil is low in selenium | Nausea, diarrhea, vomiting, fatigue | 400 mcg/day |
| Iodine | weight gain, itchy skin, low heart-rate | Populations where the soil is low in iodine, and iodized salt is not used | Enlarged thyroid | 1110 mcg/day |
| Chromium | Abnormal glucose metabolism | Malnourished children | None | ND |
| Fluoride | Increased risk of dental caries | Populations with non-fluoridated water | Fluorosis mottled teeth, kidney damage | 10 mg/day |
| Manganese | Impaired growth, skeletal abnormalities, abnormal glucose metabolism | None | Nerve damage | 11 mg/day |
| Molybdenum | Unknown | None | Arthritis, joint inflammation | 2 mg/day |
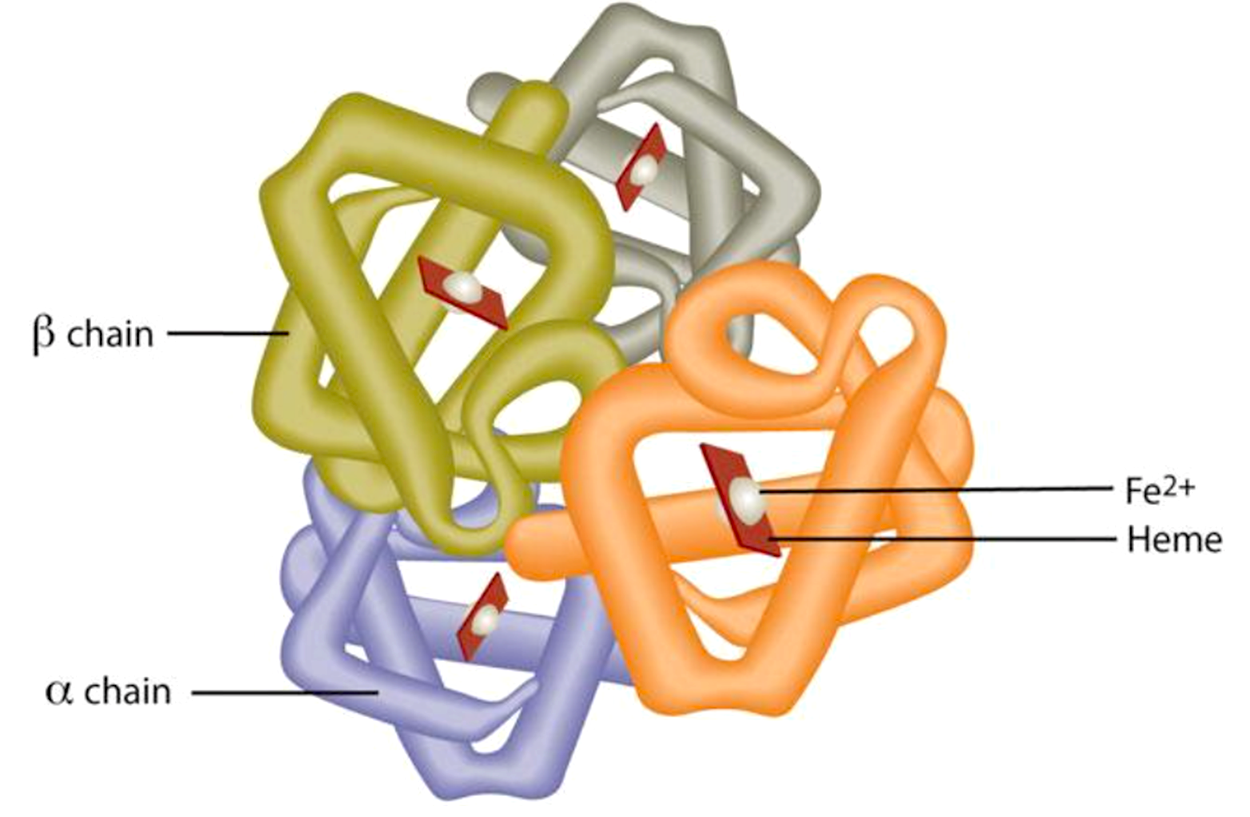
Red blood cells contain the oxygen-carrier protein hemoglobin. It is composed of four globular peptides, each containing a heme complex. In the center of each heme lies iron. Iron is needed for the production of other iron-containing proteins such as myoglobin. Myoglobin is a protein found in the muscle tissues that enhances the amount of available oxygen for muscle contraction. Iron is also a key component of hundreds of metabolic enzymes. Many of the proteins in the electron-transport chain contain iron–sulfur clusters involved in the transfer of high-energy electrons and ultimately ATP synthesis.
Iron is also involved in numerous metabolic reactions that take place mainly in the liver and detoxify harmful substances. Moreover, iron is required for DNA synthesis. The great majority of iron used in the body is recycled from the continuous breakdown of red blood cells.
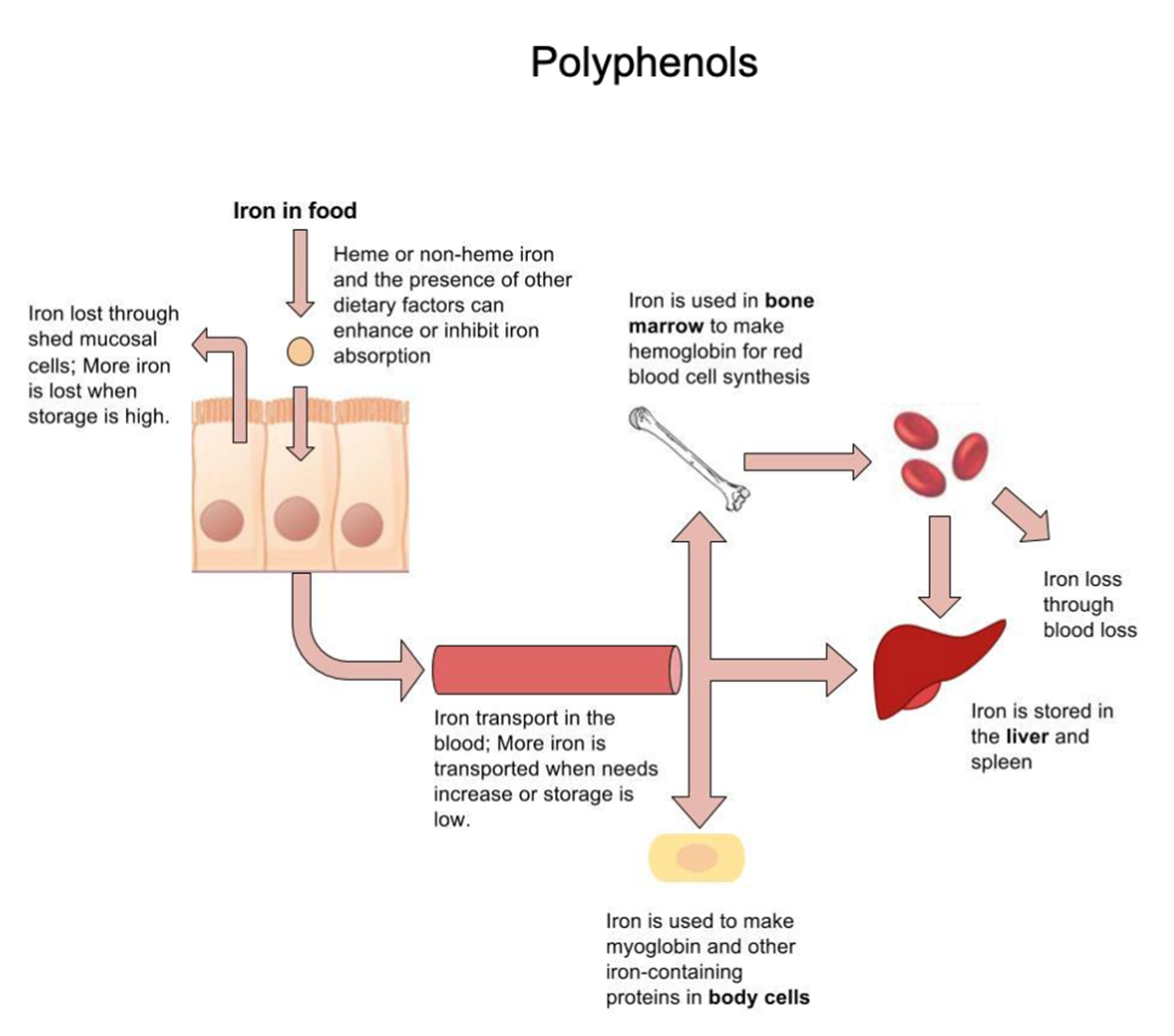
The bioavailability of iron is highly dependent on dietary sources. In animal-based foods, about 60 percent of iron is bound to hemoglobin, and heme iron is more bioavailable than nonheme iron. The other 40 percent of iron in animal-based foods is nonheme, which is the only iron source in plant-based foods. Some plants contain chemicals (such as phytate, oxalates, tannins, and polyphenols) that inhibit iron absorption. However, eating fruits and vegetables rich in vitamin C at the same time as iron-containing foods markedly increases iron absorption. Vegans are at higher risk for iron deficiency, but careful meal planning can prevent its development. Iron deficiency is the most common of all micronutrient deficiencies.
| Enhancers and Inhibitors of Iron Absorption | |
|---|---|
| Enhancer | Inhibitor |
| Meat | Phosphate |
| Fish | Calcium |
| Poultry | Tea |
| Seafood | Coffee |
| Stomach acid | Colas |
| Soy protein | |
| High doses of minerals (antacids) | |
| Bran/fiber | |
| Phytates | |
| Oxalates | |
| Polyphenols | |
The body excretes little iron, and therefore, the potential for accumulation in tissues and organs is considerable. Iron accumulation in certain tissues and organs can cause a host of health problems in children and adults, including extreme fatigue, arthritis, joint pain, and severe liver and heart toxicity. In children, death has occurred from ingesting as little as 200 mg of iron, and therefore, it is critical to keep iron supplements out of children’s reach.
The Institute of Medicine has set tolerable upper intake levels of iron. Mostly a hereditary disease, hemochromatosis is the result of a genetic mutation that leads to abnormal iron metabolism and an accumulation of iron in certain tissues, such as the liver, pancreas, and heart. The signs and symptoms of hemochromatosis are similar to those of iron overload in tissues caused by high dietary intake of iron or other non-genetic metabolic abnormalities, but are often increased in severity.
The following charts indicate the dietary reference intakes and sources of iron.
| Dietary Reference Intakes for Iron | ||
|---|---|---|
| Age Group | RDA (mg/day) | UL (mg/day) |
| Infant (0–6 months) | 0.27* | 40 |
| Infants (6–12 months) | 11* | 40 |
| Children (1–3 years) | 7 | 40 |
| Children (4–8 years) | 10 | 40 |
| Children (9–13 years) | 8 | 40 |
| Adolescents (14–18 years) | 11 (males), 15 (females) | 45 |
| Adults (19–50 years) | 8 (males), 18 (females) | 45 |
| Adults (> 50 years) | 8 | 45 |
| * denotes Adequate Intake | ||
| Iron Content of Various Foods | |||
|---|---|---|---|
| Food | Serving | Iron (mg) | Percent Daily Value |
| Breakfast cereals, fortified | 1 serving | 18 | 100 |
| Oysters | 3 oz. | 8 | 44 |
| Dark chocolate | 3 oz. | 7 | 39 |
| Beef liver | 3 oz. | 5 | 28 |
| Lentils | ½ c. | 3 | 17 |
| Spinach, boiled | ½ c. | 3 | 17 |
| Tofu, firm | ½ c. | 3 | 17 |
| Kidney beans | ½ c. | 2 | 11 |
| Sardines | 3 oz. | 2 | 11 |
Iron-deficiency anemia is a condition that develops from having insufficient iron levels in the body, resulting in fewer and smaller red blood cells containing lower amounts of hemoglobin. Regardless of the cause (be it from low dietary intake of iron or via excessive blood loss), iron-deficiency anemia has the following signs and symptoms, which are linked to the essential functions of iron in energy metabolism and blood health:
The Centers for Disease Control and Prevention reports that iron deficiency is the most common nutritional deficiency worldwide. The WHO estimates that 80 percent of people are iron deficient, and 30 percent of the world population has iron-deficiency anemia. The main causes of iron deficiency worldwide are parasitic worm infections in the gut, causing excessive blood loss, and malaria, a parasitic disease causing the destruction of red blood cells. In the developed world, iron deficiency is more the result of dietary insufficiency and/or excessive blood loss occurring during menstruation or childbirth.
IN CONTEXT
At-risk populations, including infants, children, adolescents, and women, are the populations most at risk worldwide for iron-deficiency anemia by all causes. Infants, children, and even teens require more iron because iron is essential for growth. In these populations, iron deficiency (and eventually iron-deficiency anemia) can also cause the following signs and symptoms: poor growth, failure to thrive, and poor performance in school, as well as mental, motor, and behavioral disorders. Women who experience heavy menstrual bleeding or who are pregnant require more iron in the diet. One more high-risk group is the elderly. Both elderly men and women have a high incidence of anemia, and the most common causes are dietary iron deficiency and chronic disease, such as ulcers, inflammatory diseases, and cancer. Additionally, those who have recently suffered from traumatic blood loss—frequently donate blood, or take excessive antacids for heartburn—need more iron in the diet.
In young children, iron-deficiency anemia can cause significant motor, mental, and behavioral abnormalities that are long-lasting.
Copper, like iron, assists in electron transfer in the electron-transport chain. Furthermore, copper is a cofactor of enzymes essential for iron absorption and transport. The other important function of copper is as an antioxidant. Symptoms of mild to moderate copper deficiency are rare. More severe copper deficiency can cause anemia from the lack of iron mobilization in the body for red blood cell synthesis. Other signs and symptoms include delayed growth in children and neurological problems because copper is a cofactor for an enzyme that synthesizes myelin, which surrounds many nerves.
Zinc is a cofactor for more than 200 enzymes in the human body and plays a direct role in RNA, DNA, and protein synthesis. Zinc is also a cofactor for enzymes involved in energy metabolism. As a result of its prominent roles in anabolic and energy metabolism, a zinc deficiency in infants and children blunts growth. The reliance of growth on adequate dietary zinc was discovered in the early 1960s in the Middle East, where adolescent nutritional dwarfism was linked to diets containing high amounts of phytate.
The following charts indicate the dietary reference intakes and dietary sources for zinc.
| Dietary Reference Intakes for Zinc | ||
|---|---|---|
| Age Group | RDA (mg/day) | UL (mg/day) |
| Infant (0–6 months) | 2* | 4 |
| Infants (6–12 months) | 3 | 5 |
| Children (1–3 years) | 3 | 7 |
| Children (4–8 years) | 5 | 12 |
| Children (9–13 years) | 8 | 23 |
| Adolescents (14–18 years) | 11 (males), 9 (females) | 34 |
| Adults (19 + years) | 11 (males), 8 (females) | 40 |
| * denotes Adequate Intake | ||
| Zinc Content of Various Foods | |||
|---|---|---|---|
| Food | Serving | Zinc (mg) | Percent Daily Value |
| Oysters | 3 oz. | 74 | 493 |
| Beef, chuck roast | 3 oz. | 7 | 47 |
| Crab | 3 oz. | 6.5 | 43 |
| Lobster | 3 oz. | 3.4 | 23 |
| Pork loin | 3 oz. | 2.9 | 19 |
| Baked beans | ½ c. | 2.9 | 19 |
| Yogurt, low fat | 8 oz. | 1.7 | 11 |
| Oatmeal, instant | 1 packet | 1.1 | 7 |
| Almonds | 1 oz. | 0.9 | 6 |
Iodine is essential for the synthesis of thyroid hormone, which regulates basal metabolism, growth, and development. Low iodine levels, and the resulting hypothyroidism, have many signs and symptoms, including fatigue, sensitivity to cold, constipation, weight gain, depression, dry, itchy skin, and paleness.

The following charts indicate the dietary reference intakes and dietary sources for iodine.
| Dietary Reference Intakes for Iodine | ||
|---|---|---|
| Age Group | RDA Males and Females mcg/day | UL |
| Infants (0–6 months) | 110* | |
| Infants (7–12 months) | 130* | |
| Children (1–3 years) | 90 | 200 |
| Children (4–8 years) | 120 | 300 |
| Children (9–13 years) | 150 | 600 |
| Adolescents (14–18 years) | 150 | 900 |
| Adults (> 19 years) | 150 | 1,100 |
| * denotes Adequate Intake | ||
The mineral content of foods is greatly affected by the soil from which it grew, and thus geographic location is the primary determinant of the mineral content of foods. For instance, iodine comes mostly from seawater, so the greater the distance from the sea, the lesser the iodine content in the soil.
| Iodine Content of Various Foods | |||
|---|---|---|---|
| Food | Serving | Iodine (mcg) | Percent Daily Value |
| Seaweed | 1 g. | 16 to 2,984 | 11 to 1,989 |
| Cod fish | 3 oz. | 99 | 66 |
| Yogurt, low fat | 8 oz. | 75 | 50 |
| Iodized salt | 1.5 g. | 71 | 47 |
| Milk, reduced fat | 8 oz. | 56 | 37 |
| Ice cream, chocolate | ½ c. | 30 | 20 |
| Egg | 1 large | 24 | 16 |
| Tuna, canned | 3 oz. | 17 | 11 |
| Prunes, dried | 5 prunes | 13 | 9 |
| Banana | 1 medium | 3 | 2 |
Source: This Tutorial has been adapted from "Human Resources Management" by Lumen Learning. Access for free at courses.lumenlearning.com/wm-humanresourcesmgmt/. License: CC BY: Attribution.
REFERENCES
Fact Sheet for Health Professionals: Zinc. National Institute of Health, Office of Dietary Supplements. ods.od.nih.gov/factsheets/Zinc-HealthProfessional/. Updated February 11, 2016. Accessed November 10, 2017.
Health Professional Fact Sheet: Iodine. National Institute of Health, Office of Dietary Supplements. ods.od.nih.gov/factsheets/Iodine-HealthProfessional/. Updated June 24, 2011. Accessed November 10, 2017.