Table of Contents |
As you have learned, the CNS consists of the brain and spinal cord. The brain is the control center of our nervous system and is divided into complex divisions. It is commonly divided into three main regions: the forebrain, the midbrain, and the hindbrain.
Take a look at the image below as you learn about the three main regions of the brain.
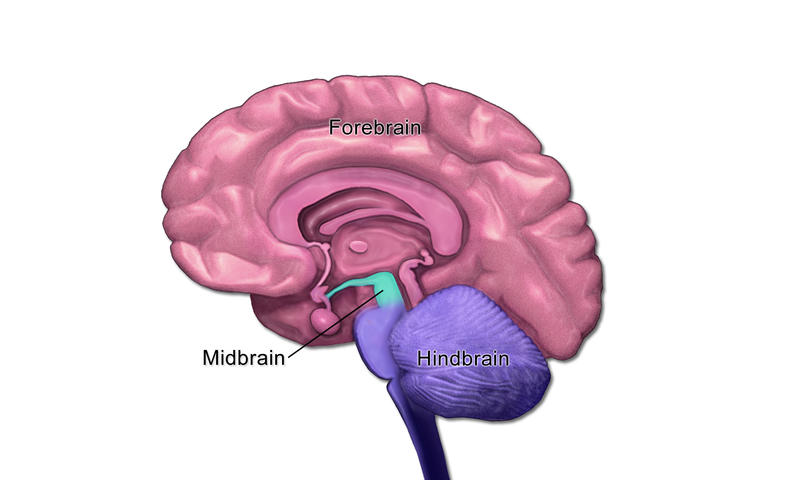
The forebrain is the most highly developed part of your brain. It includes the two hemispheres of the cerebrum, the thalamus, the hypothalamus, and the epithalamus.
The midbrain, which is the little part labeled in green, is the smallest region of our brain. The function of the midbrain is to relate information from the body's sensory organs to the forebrain, where that information can then be processed.
The hindbrain, in pink, is located just above the spinal cord and includes the parts of the brain such as the medulla oblongata, the cerebellum, and the pons.
However, scientific literature often varies in how these divisions are presented, depending on the depth of the material. See the brain division chart below that describes some of the more complex divisions of the brain. You will encounter several of these divisions in future lessons.
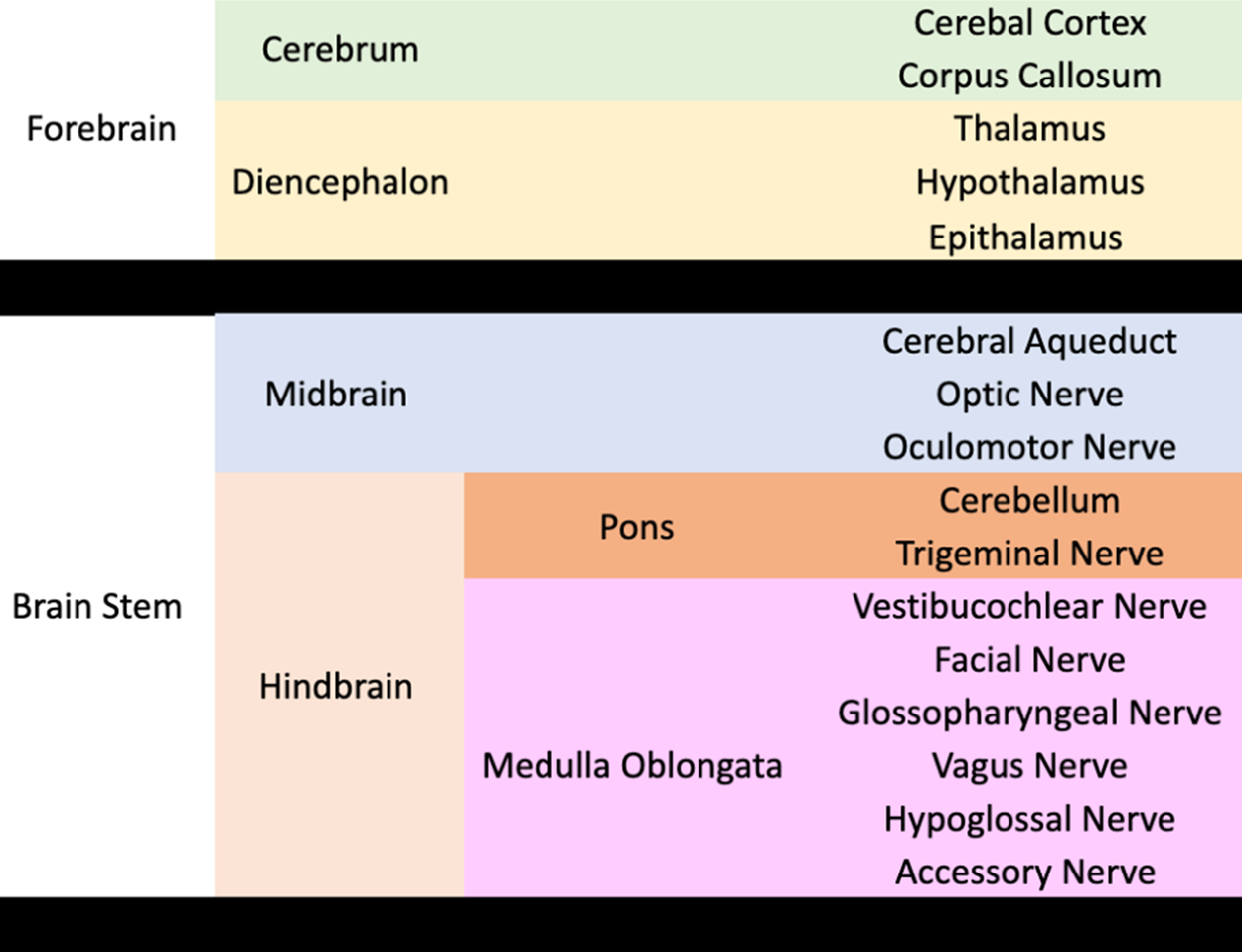
The cerebellum is often referred to as a separate structure from the pons. However, one of the main roles of the pons is to serve as the connection point between the forebrain and peripheral nervous system and the cerebellum. The cerebellum receives copies of incoming and outgoing messages through the pons and makes changes to commands based on new incoming data. You will learn more about each of these parts of the brain in future lessons.
The brain and spinal cord of the CNS are covered with three layers of protective coverings called meninges (from the Greek word for membrane). Meninges are just membranes of connective tissue located between the skull and the brain. The purpose of these three layers is to cover the CNS's neurons and blood vessels. They protect the brain as well as the neurons and blood vessels associated with the brain.
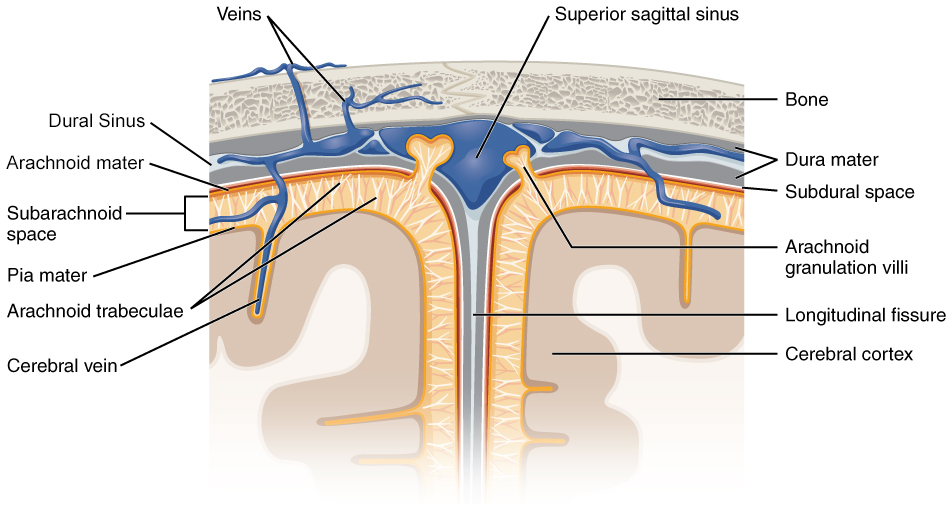
The outermost layer is the dura mater (Latin for “hard mother”). As the Latin suggests, the primary function of this thick layer is to protect the brain and spinal cord. The space between the dura mater and the skull is called the epidural space.
The dura mater is a thick, fibrous, outer layer and a strong protective sheath over the entire brain and spinal cord. It is anchored to the inner surface of the cranium and vertebral cavity. It encloses the entire CNS and the major blood vessels that enter the cranium and vertebral cavity.
The middle layer is the web-like arachnoid mater. The subdural space exists between the dura mater and the arachnoid mater.
The membrane of the arachnoid mater is composed of a thin, fibrous tissue that forms a loose sac around the CNS. Beneath the arachnoid is a thin, filamentous mesh called the arachnoid trabeculae, which looks like a spider web and gives this layer its name (arachnid, arthropod such as spider).
The space that the trabeculae extend through is called the subarachnoid space. This space is filled with cerebrospinal fluid (CSF) that is circulating around the CNS and acts to cushion the brain.
Around the brain, the arachnoid membrane forms arachnoid granulations, which are periodic extensions into the superficial dural sinus (space within the dura mater), where the CSF is filtered back into the blood for drainage from the nervous system.
The last layer is the pia mater (Latin for “soft mother”), which is a thin, fibrous membrane that follows the convolutions of gyri and sulci in the cerebral cortex and fits into other grooves and indentations. The pia mater directly contacts and covers the brain and spinal cord like plastic wrap.
IN CONTEXT
Disorders of the Meninges
Meningitis is an inflammation of the meninges, the three layers of fibrous membrane that surround the CNS. Meningitis can be caused by bacterial or viral infection. The particular pathogens are not special to meningitis; it is just an inflammation of that specific set of tissues from what might be a broader infection. Bacterial meningitis can be caused by Streptococcus, Staphylococcus, or the tuberculosis pathogen, among many others. Viral meningitis is usually the result of common enteroviruses (such as those that cause intestinal disorders) but may be the result of the herpes virus or West Nile virus. Bacterial meningitis tends to be more severe.
The symptoms associated with meningitis can be fever, chills, nausea, vomiting, light sensitivity, soreness of the neck, or severe headache. More important are the neurological symptoms, such as changes in mental state (confusion, memory deficits, and other dementia-type symptoms). A serious risk of meningitis can be damage to peripheral structures because of the nerves that pass through the meninges. Hearing loss is a common result of meningitis.
The primary test for meningitis is a lumbar puncture. A needle inserted into the lumbar region of the spinal column through the dura mater and arachnoid membrane into the subarachnoid space can be used to withdraw the fluid for chemical testing. Fatality occurs in 5% to 40% of children and 20% to 50% of adults with bacterial meningitis. Bacterial meningitis can be treated with antibiotics, but viral meningitis cannot be treated with antibiotics because viruses do not respond to that type of drug. Fortunately, the viral forms are milder.
The blood-brain barrier controls what blood-borne substances are allowed to enter the CSF.
The reason the blood-brain barrier is protective and can control what substances can enter the CSF is that the capillary walls of the barrier are much less permeable to substances than other capillaries found in your body. It helps to control the spread of viruses, toxins, and bacteria from having contact with the brain. You don't want those materials entering your CSF because your brain is such an important part of your nervous system and your entire body that you need to make sure that whatever is entering it is controlled. This means that if you do have an infection in your CNS, it's much harder to get medicine (such as antibiotics) past the blood-brain barrier to the site of infection.
However, the blood-brain barrier doesn't protect your hypothalamus, and the reason for that is because your hypothalamus needs to be exposed to your bloodstream so it can monitor the chemical makeup and the temperature of your blood to help maintain homeostasis.
A lack of oxygen in the CNS can be devastating and may cause issues such as stroke, brain damage, seizures, lack of consciousness, and even death. To counteract even short-term losses, the blood vessels supplying blood to the brain have been designed with multiple pathways to the brain as well as regulatory reflexes that ensure blood supply is not interrupted.
In the CNS, there are multiple pathways for blood to get to the brain. You may have heard of the carotid or vertebral arteries. If one gets blocked, blood can travel by the others to continue supplying the brain with nutrients. Furthermore, these pathways fuse and diverge multiple times so that a blockage or narrowing in one does not affect the perfusion of the CNS.
Additionally, when you stand up, blood tends to rush downwards, away from the brain, due to gravity. A reflex, called the orthostatic reflex, exists to maintain blood pressure so that the brain continues to receive blood.
IN CONTEXT
Disorders of the Central Nervous System
The supply of blood to the brain is crucial to its ability to perform many functions. Without a steady supply of oxygen, and to a lesser extent glucose, the nervous tissue in the brain cannot keep up its extensive electrical activity. These nutrients get into the brain through the blood, and if blood flow is interrupted, neurological function is compromised.
The common name for a disruption of blood supply to the brain is a stroke. It is caused by a blockage of an artery in the brain. The blockage is from some type of embolus: a blood clot, a fat embolus, or an air bubble. When the blood cannot travel through the artery, the surrounding tissue that is deprived starves and dies.
Strokes will often result in the loss of very specific functions. A stroke in the lateral medulla, for example, can cause a loss in the ability to swallow. Sometimes, seemingly unrelated functions will be lost because they are dependent on structures in the same region. Along with the swallowing in the previous example, a stroke in that region could affect sensory functions from the face or extremities because important white matter pathways also pass through the lateral medulla. Loss of blood flow to specific regions of the cortex can lead to the loss of specific higher functions, from the ability to recognize faces to the ability to move a particular region of the body. Severe or limited memory loss can be the result of a temporal lobe stroke.
Related to strokes are transient ischemic attacks (TIAs), which can also be called “mini-strokes.” These are events in which a physical blockage may be temporary, cutting off the blood supply and oxygen to a region, but not to the extent that it causes cell death in that region. While the neurons in that area are recovering from the event, neurological function may be lost. Function can return if the area is able to recover from the event.
Recovery from a stroke (or TIA) is strongly dependent on the speed of treatment. Often, the person who is present and notices something is wrong must then make a decision. The mnemonic FAST helps people remember what to look for when someone is dealing with sudden losses of neurological function. If someone complains of feeling “funny,” check these things quickly: Look at the person’s face. Do they have problems moving Face muscles and making regular facial expressions? Ask the person to raise their Arms above the head. Can the person lift one arm but not the other? Has the person’s Speech changed? Are they slurring words or having trouble saying things? If any of these things have happened, then it is Time to call for help.
Sometimes, treatment with blood-thinning drugs can alleviate the problem, and recovery is possible. If the tissue is damaged, the amazing thing about the nervous system is that it is adaptable. With physical, occupational, and speech therapy, victims of strokes can recover, or more accurately relearn, functions.
SOURCE: THIS TUTORIAL HAS BEEN ADAPTED FROM (1) OPENSTAX “BIOLOGY 2E”. ACCESS FOR FREE AT OPENSTAX.ORG/BOOKS/BIOLOGY-2E/PAGES/1-INTRODUCTION (2) OPENSTAX “ANATOMY AND PHYSIOLOGY 2E”. ACCESS FOR FREE AT OPENSTAX.ORG/BOOKS/ANATOMY-AND-PHYSIOLOGY-2E/PAGES/1-INTRODUCTION. LICENSING (1 & 2): CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.