Table of Contents |
Musculoskeletal injuries are common, and proper use of diagnostic imaging and testing is important to evaluate bones, joints, and soft tissues. Common types of imaging include X-rays, MRIs, bone density testing, and some others. Some types of testing use contrast to make particular structures more clearly visible.
X-rays use a form of radiation that travels through the body and strikes an X-ray detector (such as radiographic film or a digital X-ray detector) on the other side of the patient, forming an image that represents the “shadows” of objects inside the body. Bones readily absorb X-rays and, therefore, produce high contrast on the X-ray detector. As a result, bony structures appear whiter than other tissues against the black background of a radiograph. X-rays are used to detect bone fractures, tumors, and dental problems.
The figure below shows a normal hip X-ray.
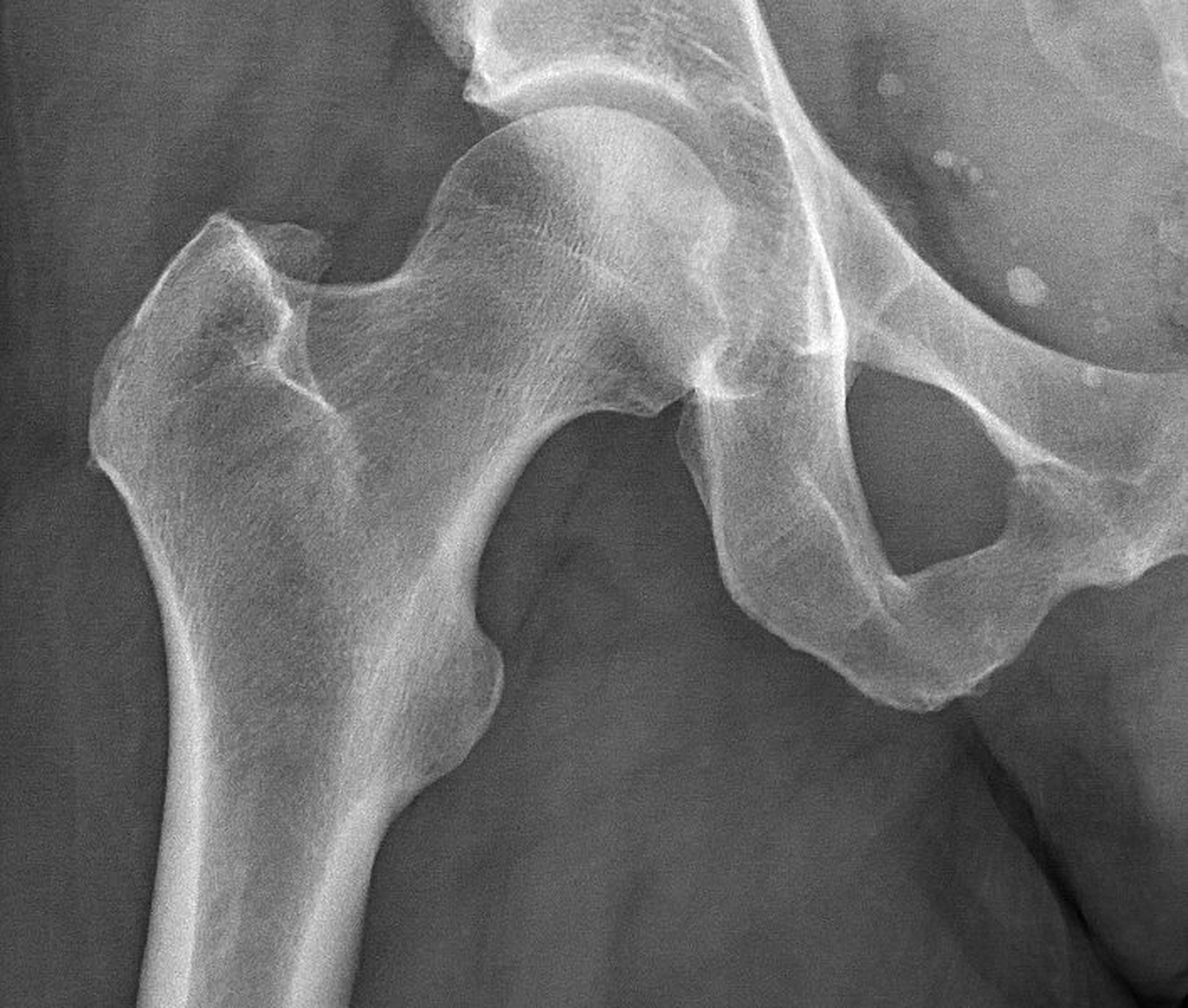
X-rays should be used wisely because they produce ionizing radiation, a form of radiation that has the potential to harm living tissue. This risk increases with the number of X-ray exposures over the lifetime of an individual. Although the risk of developing cancer from radiation exposure is generally small, it is safest to avoid unnecessary exposure and to take extra precautions when working with patients who may be pregnant. Children are more sensitive to ionizing radiation and have a long life expectancy, so machine settings can be adjusted according to the patient’s age. Radiation exposure is measured in millisieverts (mSv), and exposure of people who regularly work in radiography is monitored. Sometimes lead shielding is used to reduce the risk.
X-rays are most effective in identifying fractures, dislocations, arthritis, and bone tumors.
Some important combining forms are shown in the table below.
| Term | Definition | Example | Definition of Example |
|---|---|---|---|
| Radi/o | X-ray, radiation | Radiography | Imaging using radiation |
| Tom/o | Slice, section | Computed tomography (CT) scan | A type of imaging scan that includes information from multiple X-rays (slices) |
| Densit/o | Density | Bone densitometry | Testing to determine bone density |
Additional terminology related to X-rays includes:
- Radiolucent – Structures that appear dark on X-ray (e.g., air, soft tissue).
- Radiopaque – Structures that appear white on X-ray (e.g., bone, metal implants)
Several types of X-ray studies can be used in musculoskeletal diagnosis. These include:
- Standard X-ray (plain radiography) – Basic imaging for fractures, arthritis, bone tumors.
- Stress X-ray – Taken while joint is stressed or bearing weight.
- Fluoroscopy – Real-time X-ray imaging used in guided injections or fracture repairs.
In some cases, a contrast medium such as iodine is used. The contrast medium is taken up by certain body structures, increasing their visibility.
Magnetic resonance imaging (MRI) uses magnetic fields and radio waves to create detailed images of soft tissues, bones, and joints. It is best for evaluating ligament injuries, cartilage damage, spinal cord abnormalities, and tumors. Because metal implants (such as pacemakers) can be hazardous in an MRI, patients must be warned and checked for incompatible implants. Additionally, some patients find MRI scans very claustrophobic. Open MRI machines, which are less confining, can help.
Some common MRI terminology includes:
- T1-weighted image – Shows fat as bright, useful for bone marrow evaluation
- T2-weighted image – Shows fluid as bright, useful for detecting swelling or inflammation
- Gadolinium contrast – A type of contrast that enhances blood vessels and soft tissues in MRI scans
Some common types of MRI studies used for musculoskeletal diagnosis include:
- MRI arthrogram – Uses contrast injection to evaluate joint structures.
- Functional MRI (fMRI) – Measures blood flow changes in tissues, useful in muscle injuries.
- MR myelography – Evaluates spinal cord and nerve roots without radiation.
The image below shows MRI imaging of the lower back. This patient has an intervertebral disk that has herniated, meaning it has moved out of place and is now pressing on the spine. The red arrow is pointing to the affected area, and you can see a gray patch where the disk is protruding.
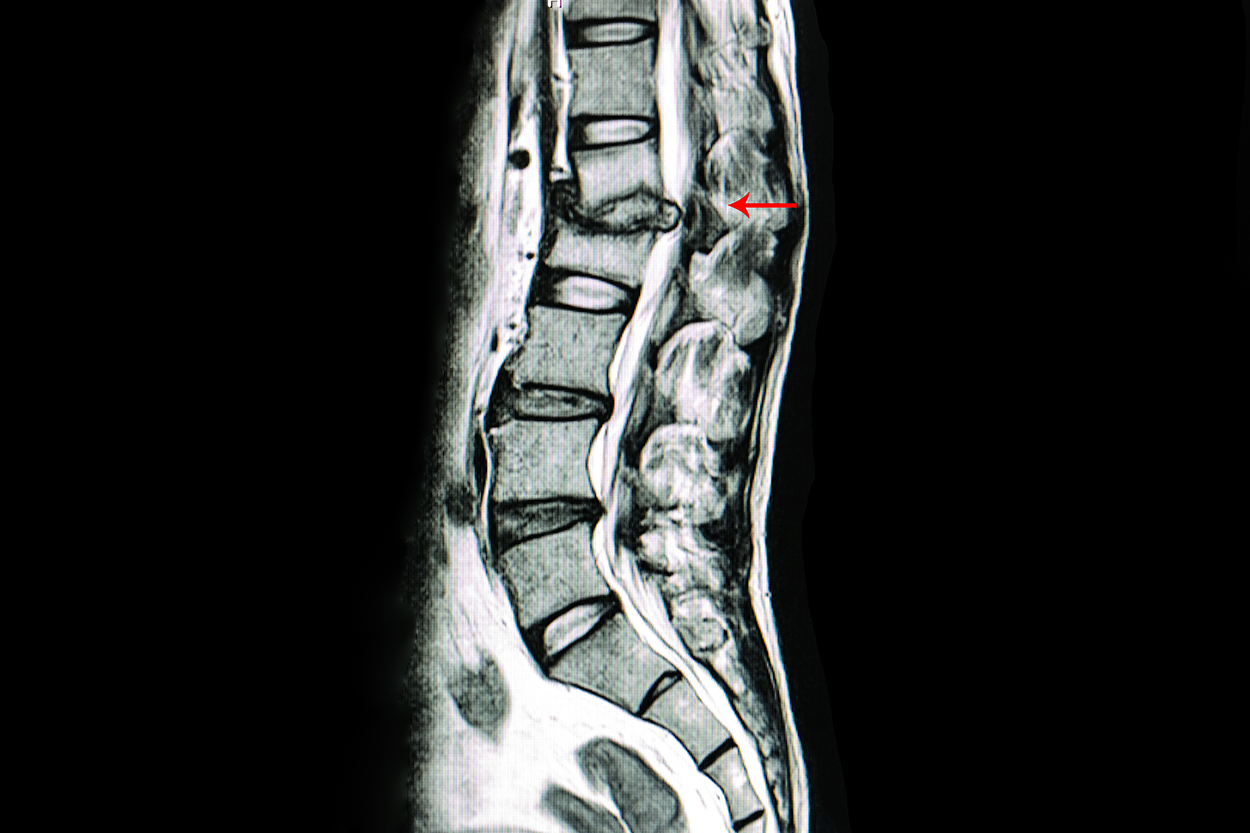
A bone mineral density (BMD) test is a test that measures calcium and other minerals in bone. This type of testing is also called bone densitometry. Bones can become less dense as people age or if certain medical conditions occur. When too much bone is lost, osteopenia or osteoporosis can develop, causing bones to become weak and brittle and increasing the risk of fractures.
The most common bone mineral density test is a central dual energy X-ray absorptiometry or also called a DEXA scan. DEXA scans use radiation to measure how much calcium and other minerals are in a specific area of the bone. Because the weakest bones that break most often due to osteoporosis are the hip and spine, DEXA scans typically measure bone mineral density in these bones. DEXA scans are best at detecting osteopenia, osteoporosis, and trabecular bone loss (weakening of spongy bone due to osteoporosis).
Postmenopausal women and men over age 50 receive bone mineral density test results as a T-score or Z-score. A T-score is the difference between their bone mineral density and 0, which represents the bone mineral density of a healthy young adult. The lower the T-score, the higher the risk of bone fracture. A Z-score compares the patient’s bone density to age-matched peers.
The figure below shows a patient undergoing a DEXA scan.
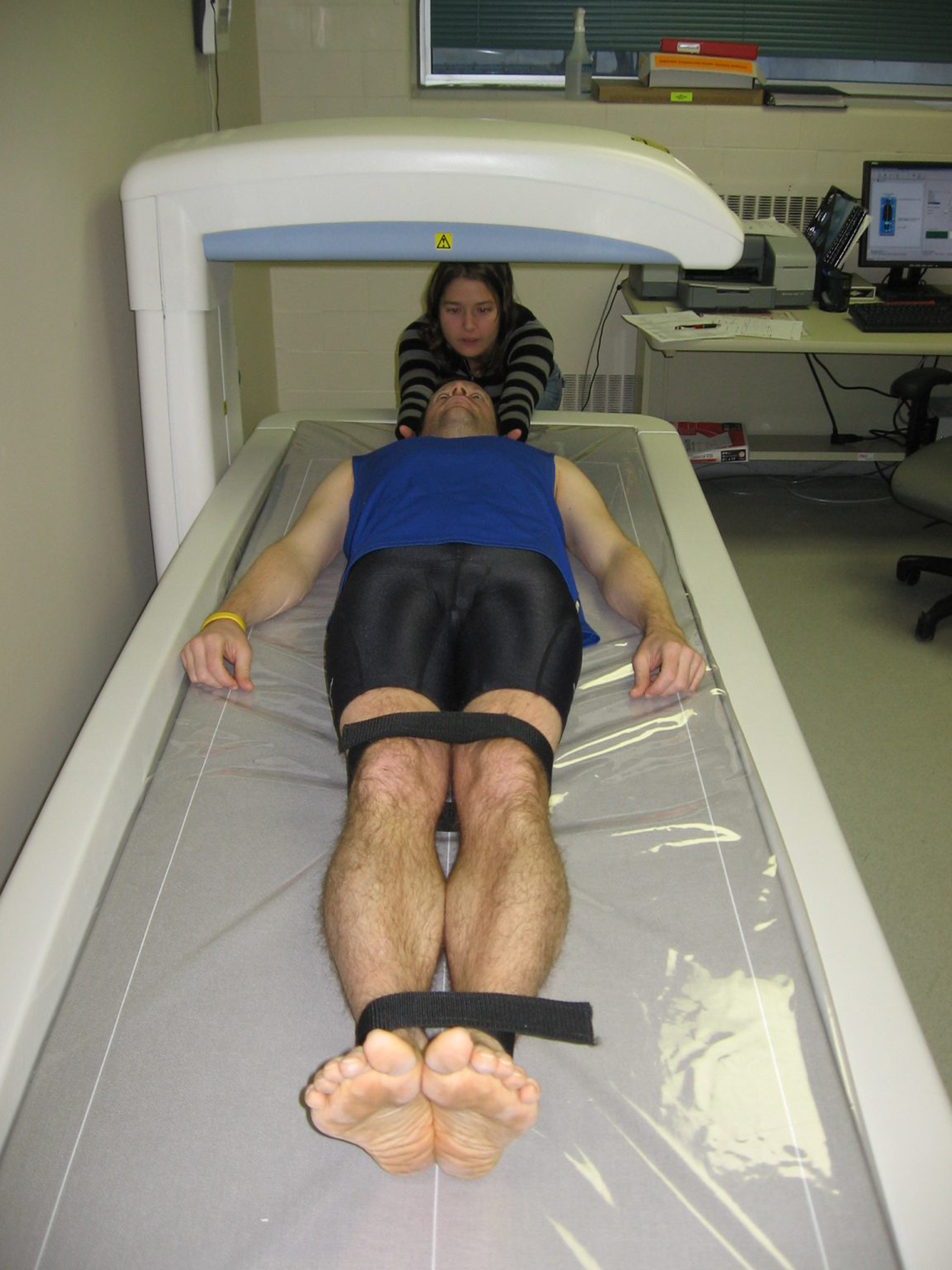
Alternative testing includes quantitative computed tomography (QCT), which provides 3D imaging of bone mineral density, and peripheral DEXA (pDEXA), which is used for the wrist, heel, or finger bones instead of the spine and hip.
The figure below shows an image produced from a DEXA scan. The left-hand image shows bone density in the hip, and the right-hand image shows bone density in the vertebral column of L1 through L4.
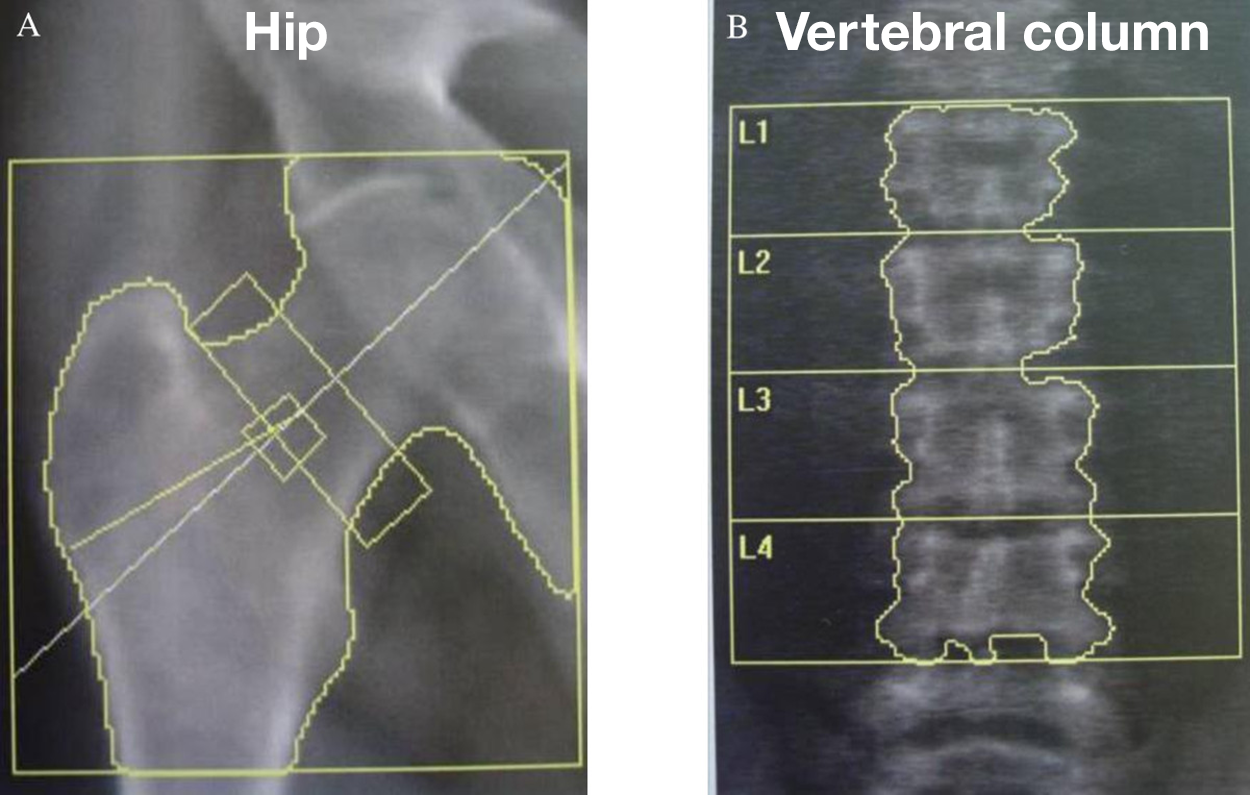
Other testing can also be used to diagnose and detect musculoskeletal conditions. CT (computed tomography) scans use X-rays and computer processing to create detailed cross-sectional images. This is best for examining complex fractures, bone tumors, and spinal injuries. In CT scans, axial slice means a horizontal section of the body, and 3D reconstruction refers to a three-dimensional view produced by the scan.
Another common type of testing is ultrasound (sonography). Ultrasound uses sound waves to evaluate tendons, muscles, and joints. It is best for examining tendon tears (e.g., rotator cuff, Achilles tendon) and joint inflammation. Doppler ultrasound is a technique that examines blood flow, which can be helpful in assessing whether there is sufficient blood flow to an injured limb. The terms hyperechoic (brighter) and hypoechoic (darker) describe brightness levels in ultrasound images.
Nuclear medicine scans can also be used for bone evaluation. A bone scan (radionuclide imaging) detects bone infections, fractures, and cancer metastasis. A PET (positron emission tomography) scan identifies tumors and metabolic activity.
There are many conditions that can affect bone, some due to disease, some due to injuries, and some that are congenital.
Fractures are very common. Types of fractures include:
- Closed fracture (simple fracture) – Bone breaks but does not pierce skin.
- Open fracture (compound fracture) – Bone breaks through the skin.
- Transverse fracture – Bone breaks straight across.
- Oblique fracture – Bone breaks at an angle.
- Spiral fracture – Bone twists apart.
- Comminuted fracture – Bone shatters into multiple pieces.
- Greenstick fracture – Partial fracture common in children.
- Pathologic fracture – Caused by disease (e.g., osteoporosis, cancer).
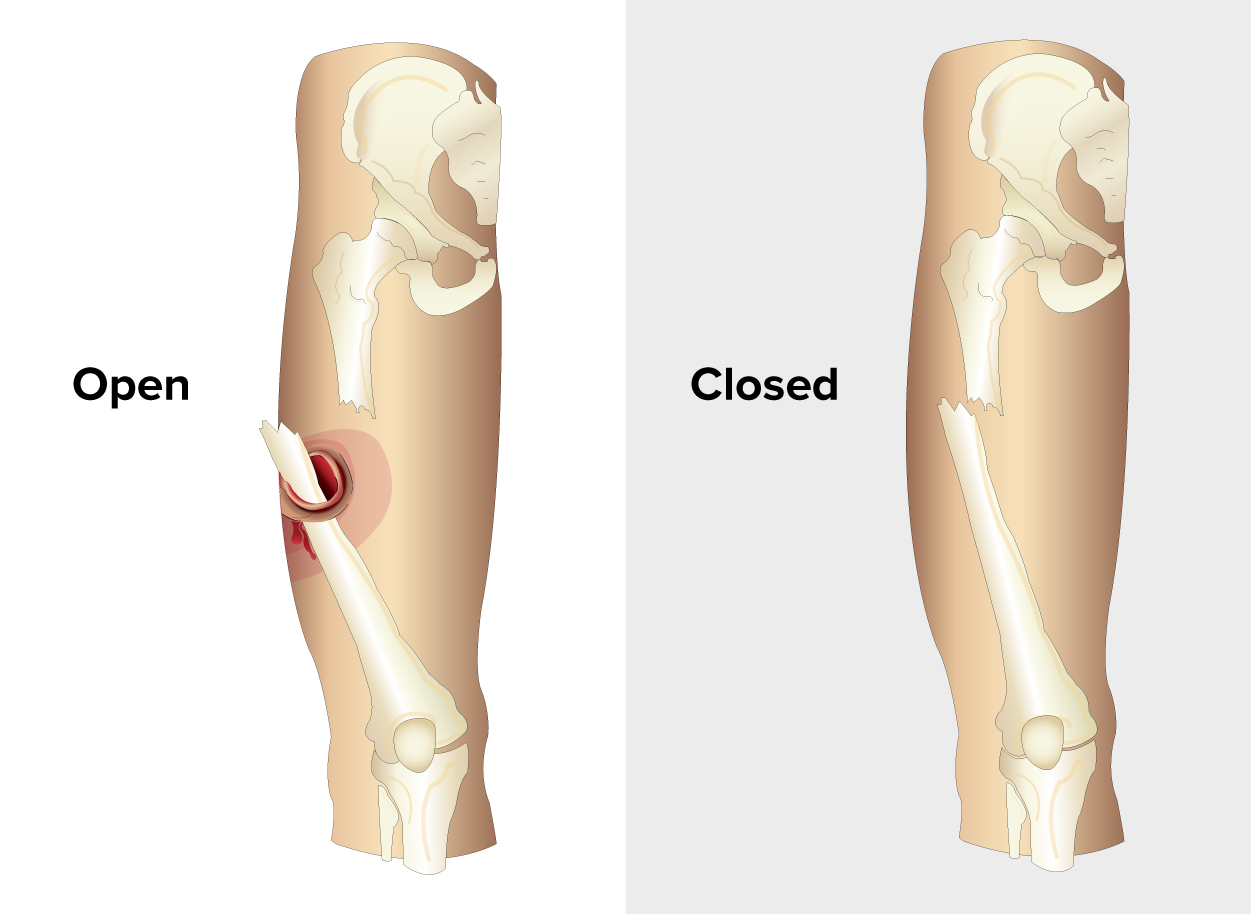
The figure below shows the difference between open and closed fractures. Note how the open fracture breaks the skin.
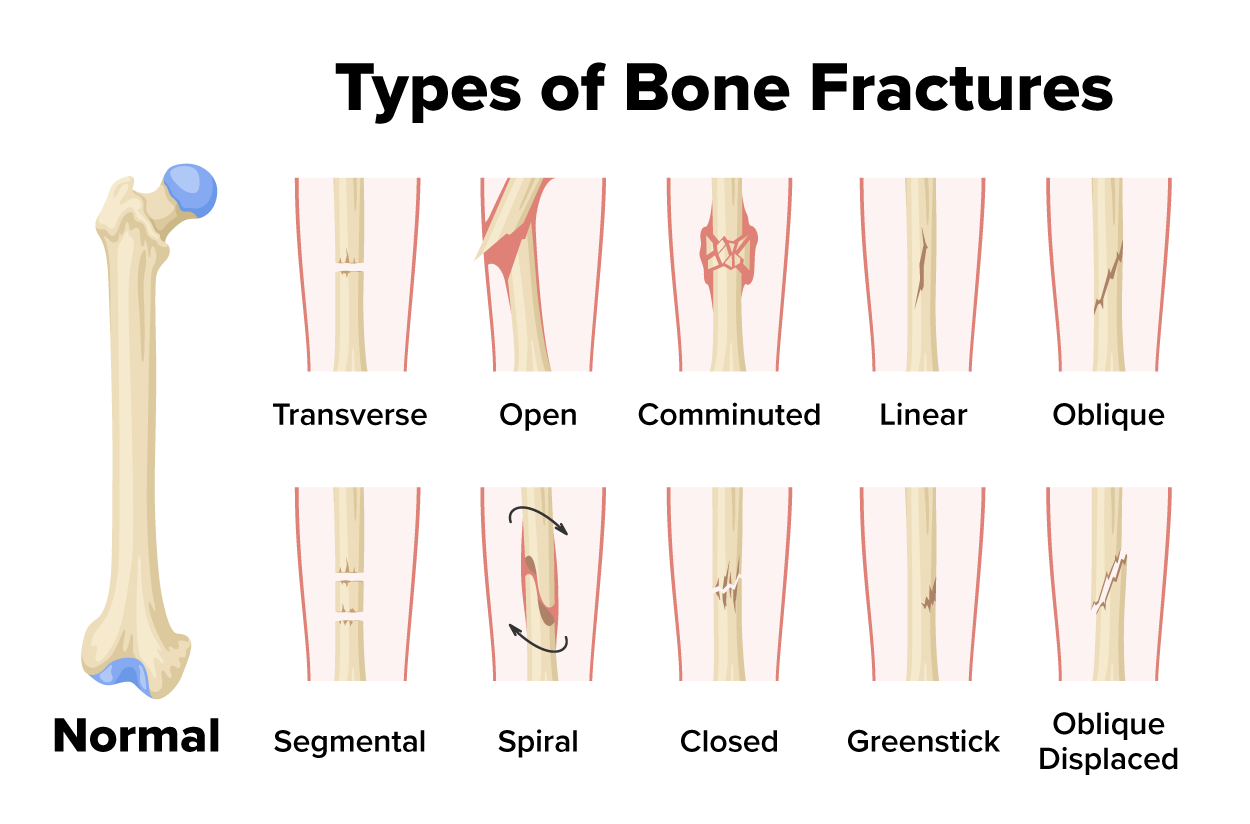
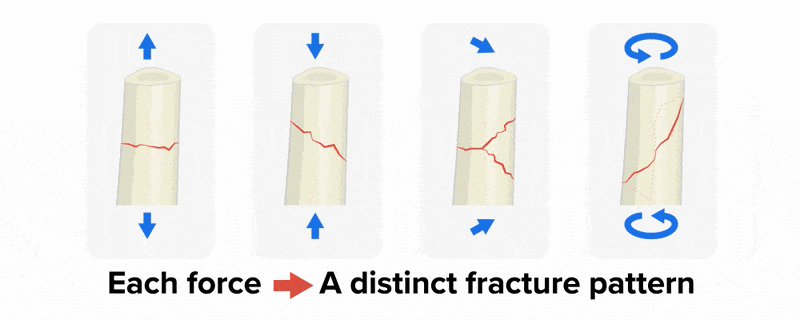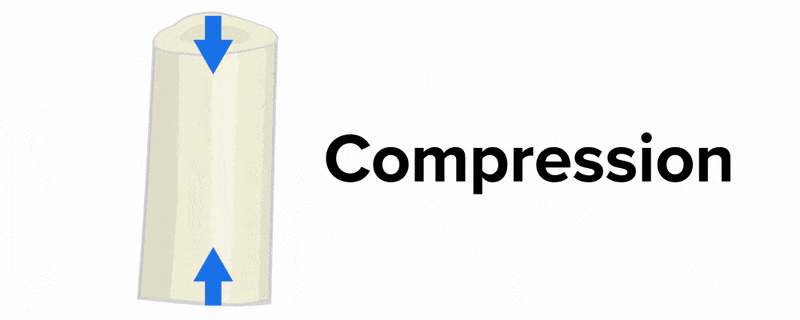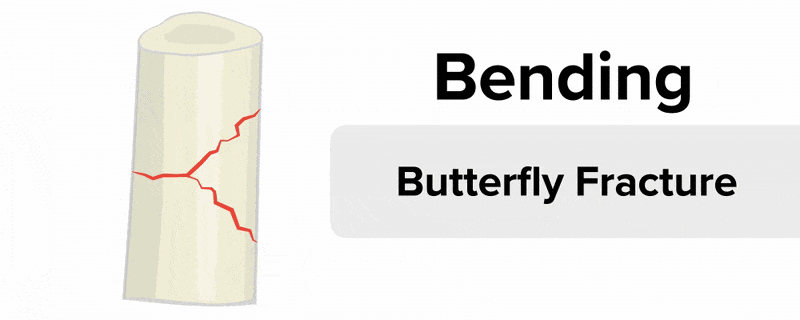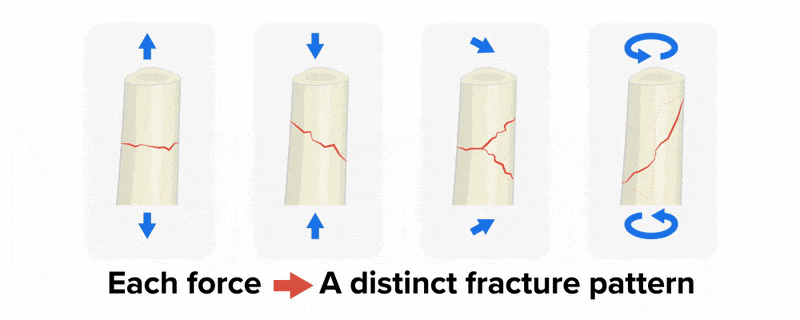
The image below shows more detail about different types of closed fractures. Note that the transverse, linear, and oblique fractures are types of closed fractures that differ in the angle of the break.
You have learned about osteopenia and osteoporosis. Some additional bone conditions are listed in the table below.
| Term | Bone referenced |
|---|---|
| Osteomalacia | Soft bones, typically due to Vitamin D deficiency |
| Paget’s disease | Chronic disorder of disorganized bone remodeling leading to deformities |
| Osteomyelitis | Inflammation of the bone and bone marrow |
| Fibrosarcoma | A type of malignant fibrous connective tissue cancer; it can develop in bones or connective tissues around bones (Cleveland Clinic, 2024). |
| Osteosarcoma | A type of malignant bone cancer that develops from osteoblasts in bones, especially long bones (Johns Hopkins Medicine, n.d.). |
| Ewing's sarcoma | A malignant bone cancer that is most common in children and young adults (Mayo Clinic, 2024). |
In addition to the imaging approaches already discussed, biopsy can also be used for diagnosis and treatment planning. Bone biopsies are used to detect infection, cancer, metabolic conditions, and other diseases.
Common bone surgeries and procedures include:
- Open reduction and internal fixation (ORIF) – Surgical repair of fractures with plates and screws (in contrast, a closed reduction moves bone parts into place without surgery)
- Joint replacement (arthroplasty) – Total hip or knee replacement
- Laminectomy – Removal of part of the vertebra to relieve pressure on spinal nerves
- Bone grafting – Transplanting bone tissue to repair or rebuild damaged bones
Source: THIS TUTORIAL HAS BEEN ADAPTED FROM “OPEN RN | MEDICAL TERMINOLOGY – 2e” BY ERNSTMEYER & CHRISTMAN AT OPEN RESOURCES FOR NURSING (Open RN). ACCESS FOR FREE AT https://wtcs.pressbooks.pub/medterm/ LICENSING: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.
REFERENCES
Cleveland Clinic. (n.d.). Fibrosarcoma. In Cleveland Clinic. Retrieved April 13, 2025, from Fibrosarcoma: Symptoms, Causes & Treatment
Johns Hopkins Medicine. (n.d.). Osteosarcoma. In Johns Hopkins Medicine. Retrieved April 13, 2025, from Osteosarcoma | Johns Hopkins Medicine
Mayo Clinic. (2024, December 5). Ewing Sarcoma. Mayo Clinic. Ewing sarcoma - Symptoms and causes - Mayo Clinic
Choong, W. S., Gallacher, S., & Ahmed, S. F. (2015). Assessing osteoporosis in the young adult. European endocrinology, 11(1), 43–44. Assessing Osteoporosis in the Young Adult - PMC
Gibson, D., Filan, Z., Westmoreland, P., & Mehler, P. S. (2024). Loss of bone density in patients with anorexia nervosa food that alone will not cure. Nutrients, 16(21), 3593. doi.org/10.3390/nu16213593
Gitajn, IL and EK Rodriguez. (2011). Biomechanics of musculoskeletal injury. In V. Klita (Ed.), Biomechanics in Applications, InTech. doi: 10.5772/20672
Kardong, K. (2018). Vertebrates: Comparative Anatomy, Function, and Evolution. 8th Edition. McGraw Hill.