Table of Contents |
Screening involves testing asymptomatic individuals. This approach is used to try to detect cancers early, before there are noticeable symptoms. Early detection can potentially allow cancers to be treated early, but good screening tests have only been developed for some cancers.
EXAMPLE
. As you learned previously, the CA125 test can be used to screen for ovarian cancer in individuals at high risk, but it can be affected by too many factors to be useful for screening people in general (Mayo Clinic staff, 2025).Successful screening programs should allow precancerous tissue or early cancers to be detected while they can be effectively treated (e.g., Aguiar-Ibáñez et al., 2025) without exposing large numbers of people to unnecessary procedures and treatments (overdiagnosis). Overdiagnosis occurs when patients undergo treatments that do not benefit them.
EXAMPLE
It would be overdiagnosis if someone underwent invasive treatments such as mastectomy for a cancer that would never have progressed (e.g., Houston et al., 2019).A screening test is intended to catch people at higher risk so that they can undergo further testing.
EXAMPLE
Someone who undergoes a screening mammogram may be called back for additional imaging, and sometimes a biopsy may be needed.However, a 2020 study found an average recall rate of 10.7 percent (meaning that 10.7 percent of women who underwent testing were asked to return), with only 4 out of 1,000 mammograms resulting in a cancer diagnosis. The authors suggested that a recall rate of 7–9 percent would be better, but this clearly shows that many healthy women are asked to return for more testing (Rauscher et al. 2021).
It’s important to be familiar with the terms false positive and false negative and to understand how this differs from the screening results described above. A false positive test appears positive when the true result should be negative.
EXAMPLE
Someone might test positive for influenza but not actually have it.A false negative test is the opposite: someone tests negative when they actually have the condition.
EXAMPLE
Someone might test negative for influenza when they actually do have the flu (Merriam Webster, n.d.a and n.d.b.).Being called back after a screening test is not the same as having a false positive result, even though people may sometimes mistakenly say that. A screening test identifies people who need further assessment for some reason, perhaps because something suggests that they are at higher risk (such as having an abnormality on a mammogram). For this to be a false positive, someone would actually have to receive a cancer diagnosis without actually having cancer.
Some additional important terms are sensitivity and specificity. Sensitivity is defined as how well a test detects a condition if the condition is present. A highly sensitive test is very good at detecting the condition. A test with the highest possible sensitivity would detect every case of a disease. In contrast, specificity describes how well a test distinguishes those who have the disease from those who don’t. A test with very high specificity has a very low false positive rate; a positive result means that someone is very likely to have the condition. In a test with low specificity, the false positive rate is higher (InformedHealth.org, 2025).

You have already encountered some examples of screening tests. Some common examples are summarized below.
A Pap smear is used for cervical cancer screening. As you have learned, cervical cancer is often caused by the human papillomavirus (HPV), which can also cause cancers of other tissues. To perform a Pap smear, a physician obtains cervical cells, typically while performing a pelvic exam. An HPV test can be performed simultaneously (WebMD, 2024).
The image below shows a normal Pap smear on the left and a Pap smear showing a mildly abnormal lesion on the right. Note the differences in the appearances of the cells.
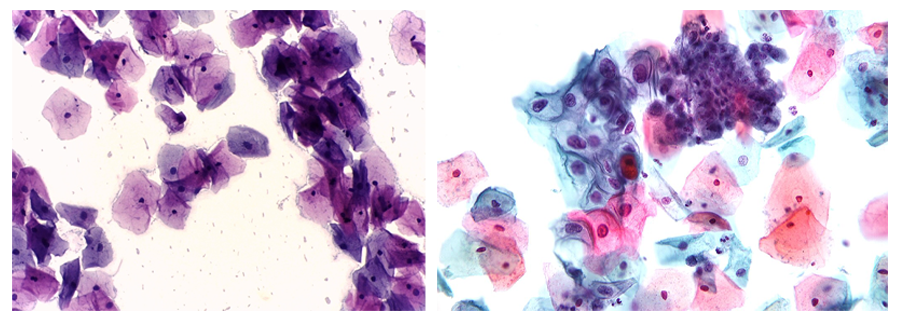
Another common test is a mammogram, which is used for breast cancer screening. A mammogram uses X-rays to produce images of the breasts. 3D mammograms (which use tomosynthesis) produce images as slices that can be assembled to produce a 3D representation of the breast (Cleveland Clinic, 2024).
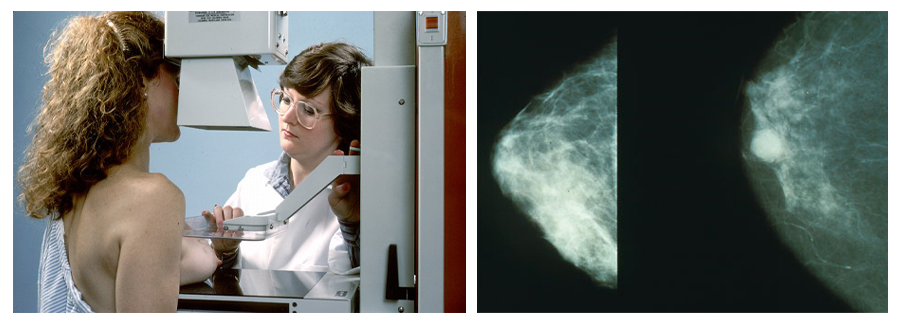
Several types of tests are used to screen for colorectal cancer, and you have learned about some of these before. These tests include stool tests that detect blood in stool samples, blood-based tests that detect a biomarker associated with colorectal cancer (not typically used as a first-line test), and visualization tests like a colonoscopy, among others. Options for visualization include colonoscopy, which has the advantage of allowing abnormal growths to be removed; sigmoidoscopy (which views only the rectum and sigmoid colon); and virtual colonoscopy (which uses a CT scan; NCI, 2024a).
A low-dose CT scan (LDCT) is available to screen for lung cancer. Although X-rays and sputum cytology can also be used, there is evidence that LDCT improves survival in people with a history of smoking; therefore, LDCT is the recommended screening test. One recommendation (from the U.S. Preventive Services Task Force) is that people who meet specific criteria for age (50-80) and heavy smoking history should be screened every year (CDC, 2024 and NCI, 2024b).
Prostate specific antigen (PSA) testing can be used to screen for prostate cancer, but its use has been controversial. The National Cancer Institute currently summarizes the available data by suggesting that it is not known whether the use of the PSA test reduces the risk of dying, even though it can detect cancer. In other words, it may result in overdiagnosis, meaning that men undergo invasive treatments for a cancer that may not have harmed them (NCI, 2024c). However, a 2025 study suggests that changing recommendations regarding PSA testing may have resulted in more cases of distant-stage disease (meaning that it has spread). The authors acknowledge the problem of overdiagnosis and suggest the need for targeted screening (Kratzer et al., 2025).
The figure below shows a polyp on the wall of a colon.
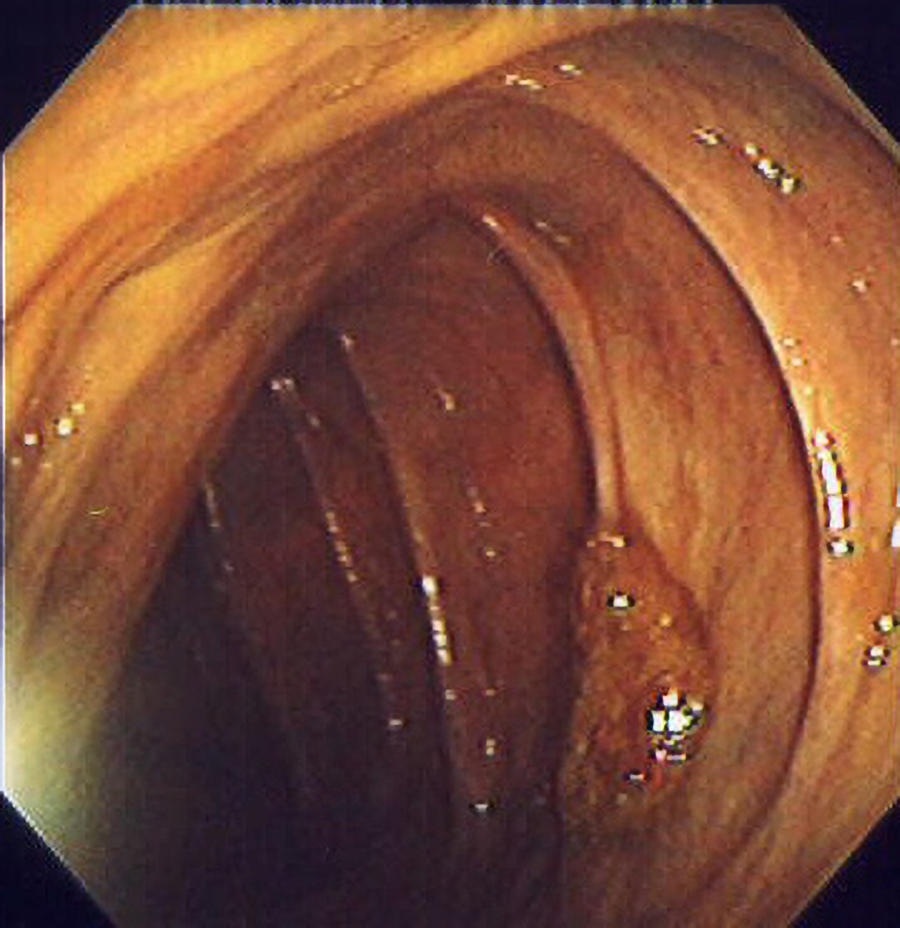
In some cases, genetic testing can be used to help make decisions about screening. Patients at higher risk may choose to have more screening than a patient at lower risk. Genetic testing is available for certain cancers, such as breast cancer and colorectal cancer (M.D. Anderson, 2021; NCI, 2024d).
EXAMPLE
It is possible for patients to get genetic testing for the BRCA1 or BRCA2 genes, which increases the risk of certain cancers (including breast cancer).Someone who knows that they are at high risk may choose to begin screening mammograms and other testing (such as ultrasounds or MRIs) earlier than typical screening recommendations. Some patients choose to have mastectomies (Alexander, 2021; NCI, 2024d).
To diagnose cancer, doctors use a variety of tests that you are already familiar with. These include imaging tests, biopsies, laboratory and molecular tests, and endoscopies.
Types of imaging commonly used in cancer diagnosis, assessment, and monitoring can include X-rays, CT scans (such as virtual colonoscopies and LDCT for lung cancer screening), tomography (to produce a 3D image, as discussed above for breast cancer screening), MRI to evaluate soft tissue in particular, ultrasounds, nuclear scans (to examine where injected radioactive substances travel in the body), specialized nuclear scans that target bone tissue (bone scans), and PET scans (to evaluate metabolic processes, which is useful in detecting metabolically active cancer cells (NCI, 2023a).
The figure below shows an image produced by LDCT. The bright spot enclosed in a circle is a calcified lung nodule. While these are often benign, they can sometimes be more serious (Khan et al., 2010).
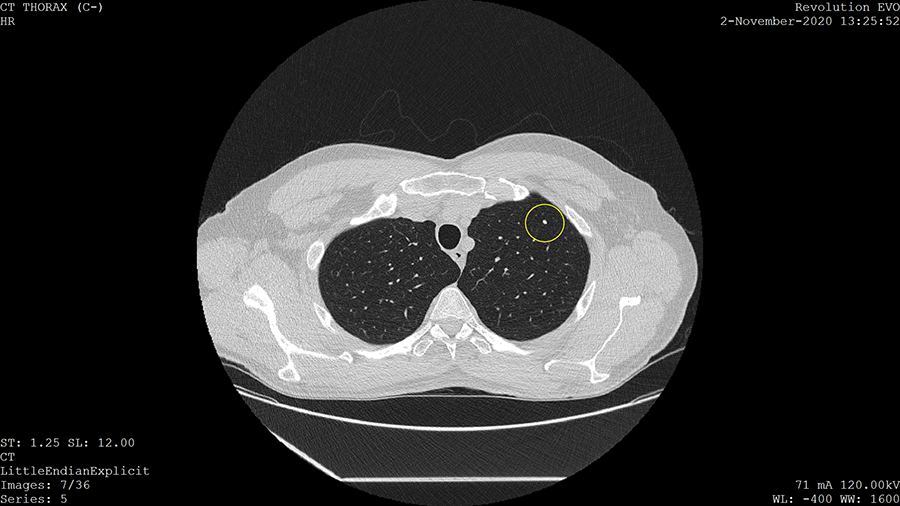
You have also already encountered examples of biopsies. Core needle biopsies and fine needle aspiration can be used, as can excisional biopsies, incisional biopsies, and punch biopsies.
You previously learned about the importance of evaluating the margins to help understand whether the cancer has been fully removed. In some cases, frozen sections are taken for rapid analysis as an operation is ongoing. These frozen sections can be evaluated quickly because they do not require the careful preparation typically used to prepare slides for analysis. Although permanent sections are considered the very best choice for diagnostic accuracy, they take much longer to prepare, and frozen sections provide information that can be needed to adjust the surgery (for example, to determine whether more tissue needs to be removed to obtain clear margins; Eichenger et al, 2022).
The figure below shows a sample obtained using fine needle aspiration. The left-hand side shows an adenocarcinoma, compared with normal tissue on the right.
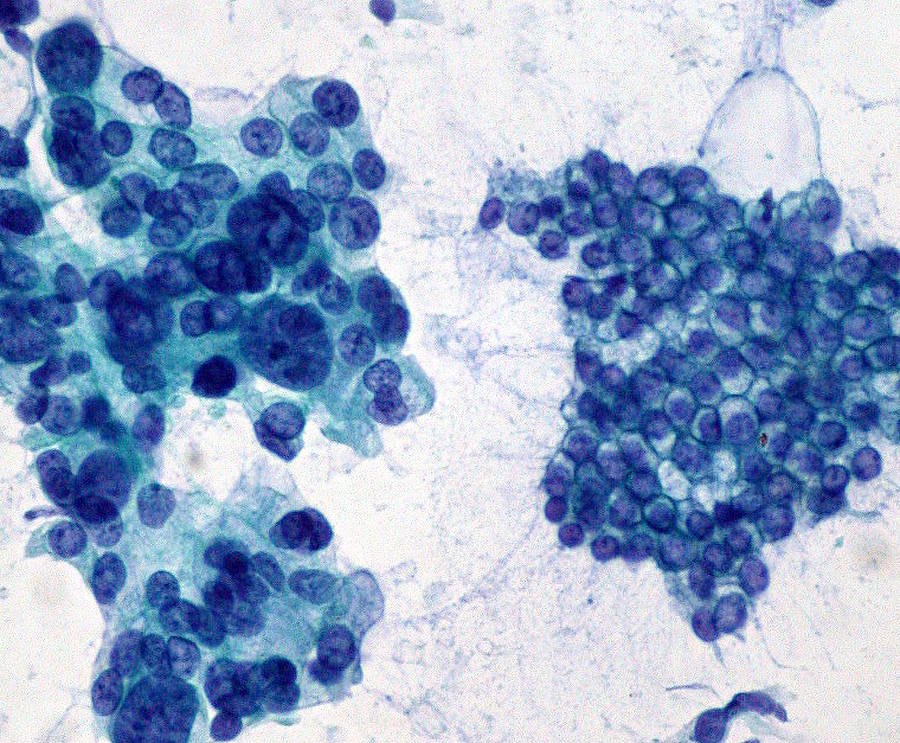
Laboratory testing can be used to detect biomarkers associated with cancer. Examples include prostate specific antigen (PSA), CA-125, and CEA. These are used for PSA tests (prostate cancer), CA-125 tests (ovarian cancer), and CEA tests (several cancers), respectively. Remember that just because these biomarkers are associated with cancer does not mean that they are helpful for general screening. Instead, each test is used in specific ways.
EXAMPLE
CA-125 is not recommended for widespread screening, but can be useful in diagnosis and monitoring for specific patients, such as those with symptoms, at high risk, or being monitored for a recurrence (Cleveland Clinic, 2022).As discussed previously, the PSA test is sometimes used for screening and diagnosis as well as monitoring, although its use for screening is controversial. CEA is also used for monitoring and to detect cancer recurrence, not for initial screening (Cleveland Clinic, 2025a).
Alpha-fetoprotein (AFP) is another biomarker that can be used in the diagnosis and monitoring of several types of cancers, including liver cancer and ovarian cancer. AFP can also be helpful in diagnosing germ cell cancers, which are cancers of the gamete (egg and sperm) producing tissues (NCI, 2023b).
As mentioned above, genetic testing can be used to aid in making decisions about screening. It can also be used to help guide treatment planning. Genetic testing can detect genes that are mutated in cancer cells, such as oncogenes (Cleveland Clinic, 2021).
There are genes that control cell division. When these mutate, cells may divide inappropriately, leading to cancer. One type of these genes is an oncogene. Oncogenes encode substances that promote inappropriate cell division. (Cleveland Clinic, 2025b).
Other genes can also be detected, and medications are available that target specific genetic mutations. So detecting these mutations can help in knowing which medications are likely to be effective.
EXAMPLE
Some breast cancers have a mutation in the HER2 gene, and these HER2 positive patients can be treated with specific medications that are often effective against cancers with this mutation (Cleveland Clinic, 2021).In some cases, endoscopies can be used to identify abnormal tissue for further examination. Examples include colonoscopy (to view the colon), bronchoscopy (to view the bronchi), cystoscopy (to view the interior of the bladder), and laparoscopy (to view the interior of the abdomen).
Source: THIS TUTORIAL WAS AUTHORED BY SOPHIA LEARNING. PLEASE SEE OUR TERMS OF USE.
REFERENCES
CA 125 Test. (2025, March 7). Mayo Clinic. CA 125 test - Mayo Clinic
Aguiar-Ibáñez, R., Mbous, Y., Sharma, S., Chakali, R., & Chawla, E. (2025). Barriers to cancer screening uptake and approaches to overcome them: a systematic literature review. Frontiers in Oncology, 15, 1575820. doi.org/10.3389/fonc.2025.1575820
Housten, A. J., Lowenstein, L. M., Hoffman, A., Jacobs, L. E., Zirari, Z., Hoover, D. S., Stacey, D., Pratt, G., Bevers, T. B., & Volk, R. J. (2019). A Review of the Presentation of Overdiagnosis in Cancer Screening Patient Decision Aids. MDM Policy & Practice, 4(2), 2381468319881447. doi.org/10.1177/2381468319881447
Rauscher, G. H., Murphy, A. M., Qiu, Q., Dolecek, T. A., Tossas, K., Liu, Y., & Alsheik, N. H. (2021). The "Sweet Spot" Revisited: Optimal Recall Rates for Cancer Detection With 2D and 3D Digital Screening Mammography in the Metro Chicago Breast Cancer Registry. AJR. American Journal of Roentgenology, 216(4), 894–902. doi.org/10.2214/AJR.19.22429
Merriam-Webster. (n.d.). False negative. In Merriam-Webster.com dictionary. Retrieved September 3, 2025, from www.merriam-webster.com/dictionary/false%20negative
Merriam-Webster. (n.d.). False positive. In Merriam-Webster.com dictionary. Retrieved September 3, 2025, from www.merriam-webster.com/dictionary/false%20positive
Institute for Quality and Efficiency in Health Care (IQWiG). (2025, January 22). In brief: Sensitivity and specificity. InformedHealth.org. www.ncbi.nlm.nih.gov/books/NBK611900/
Pap Smear. (2024, July 20). Mayo Clinic staff. Pap smear - Mayo Clinic
Mammogram. (2024, October 17). Cleveland Clinic. Mammogram: What It Is, Purpose, Procedure, Results & Types
Screening Tests to Detect Colorectal Cancer and Polyps. (2024a, October 29). National Institutes of Health (NIH) National Cancer Institute (NCI). Screening Tests to Detect Colorectal Cancer and Polyps - NCI
Screening for Lung Cancer. (2024, October 15). Centers for Disease Control and Prevention (CDC). Screening for Lung Cancer | Lung Cancer | CDC
Lung Cancer Screening (PDQ) - Patient Version. (2024b, May 24). National Institutes of Health (NIH) National Cancer Institute (NCI). Lung Cancer Screening - NCI
Kratzer, T. B., Mazzitelli, N., Star, J., Dahut, W. L., Jemal, A., & Siegel, R. L. (2025). Prostate cancer statistics, 2025. CA: A Cancer Journal for Clinicians, 10.3322/caac.70028. Advance online publication. doi.org/10.3322/caac.70028
Cheong, J., Faye, A., & Shaukat, A. (2023). Colorectal cancer screening and surveillance in the geriatric population. Current Gastroenterology Reports, 25(7), 141–145. doi.org/10.1007/s11894-023-00875-8
Alexander, H. (2021, March 6). How to get genetic testing for cancer. M.D. Anderson Cancer Center. How to get genetic testing for cancer | MD Anderson Cancer Center
The Genetics of Cancer. (2024d, August 8). National Institutes of Health (NIH) National Cancer Institute (NCI). The Genetics of Cancer - NCI
Tests and Procedures Used to Diagnose Cancer. (2023a, January 13). National Institutes of Health (NIH) National Cancer Institute (NCI). Tests and Procedures Used to Diagnose Cancer - NCI
Khan, A. N., Al-Jahdali, H. H., Allen, C. M., Irion, K. L., Al Ghanem, S., & Koteyar, S. S. (2010). The calcified lung nodule: What does it mean?. Annals of Thoracic Medicine, 5(2), 67–79. doi.org/10.4103/1817-1737.62469
Eichinger, S. E., Heymann, H. B., Mbagwu, M., Knezevic, A., & Bryar, P. J. (2022). Correlation between frozen section and permanent histopathologic diagnoses in adult orbital lesions. Ocular Oncology and Pathology, 8(2), 141–147. doi.org/10.1159/000521075
Tumor Marker Tests in Common Use. (2023b, December 7). National Institutes of Health (NIH) National Cancer Institute (NCI). Tumor Marker Tests in Common Use - NCI
CA-125 Blood Test. (2022, July 12). Cleveland Clinic. CA-125 Blood Test: Results, Normal Range & What To Expect
CEA Test (Carcinoembryonic Antigen). (2025a, June 5). Cleveland Clinic. CEA Test (Carcinoembryonic Antigen): What It Is & Results
How Genetic Testing Can Make Your Cancer Treatment More Effective. (2021, April 6). Cleveland Clinic. Genetic Testing and Cancer Treatment
Oncogene. (2025b, February 20). Cleveland Clinic. Oncogene: What They Are & What They Do