Table of Contents |
This overview of health services in modern times may overlook many nuances and historical events that influenced the evolution of U.S. health care, as many of these events are outside the scope of this course. Health services in the United States transitioned from premodern times to modern times during the time of germ theory and the beginning of the professionalization of doctors. As the role of women in administering health care to the family changed over time, between 1750 and 2000, the U.S. health care system evolved into a complex, scientific, technological, and bureaucratic system. It included medical science, technology, and the authority of medical professionals. Advances in treating diseases, the acceptance of germ theory, and the rise of medical institutions contributed to modern health care.
Medical specialization did not exist in premodern times. The few doctors who existed handled a wide range of health issues but usually only in the most serious and life-threatening cases. Their practice was based on tradition, folklore, and limited scientific knowledge, so their methods and understanding differed greatly from modern medicine.
IN CONTEXT
General Practitioners
Treating infections, cuts, and wounds was a common task in premodern times. General practitioners used basic wound care techniques, poultices (a soft, moist mass of material made of plant material), and herbal remedies. They managed fevers associated with various diseases, by relying on cooling measures like cool water on a damp cloth and herbal medicines. Herbal infusions and steam inhalations were used to address respiratory issues and pain relief for headaches, and joint pain and other discomforts were treated by administering herbal painkillers. Before the advent of antibiotics in the early 20th century, medical professionals used various methods to treat infections, cuts, and wounds. Topical iodine was commonly used to disinfect wounds, and bromine was applied topically or injected into wounds to combat infections. Wounds were often washed using wine, and surgeons applied topical remedies like myrrh, frankincense, and honey to prevent dressings from adhering to the wound.
In the mid-1800s, specializations began to emerge. Eye hospitals and specialized wards for eye disease existed in American cities. This specialty is referred to as ophthalmology. The 20th century saw professionalization and new careers opening up for women as nurses. In the early 1900s, nursing underwent a significant evolution, shaping the profession into what it is today. The Nightingale-era schools, led by Florence Nightingale, laid the groundwork for evolution in nursing education. These schools eventually gave way to hospital-controlled programs, emphasizing clinical experience over book learning (Penn Nursing, n.d.).
With modern medical specialization, some specialized doctors focus on specific areas of health like cardiology (heart health), nephrology (kidney health), and oncologists (cancer). Each specialty has unique responsibilities and areas of focus. Specialists are crucial to health care. After completing medical school, physicians or surgeons usually further their education in a specialty by completing a multiple-year residency. Residencies typically last several years and provide hands-on training, clinical experience, and exposure to specialized cases. Skills are refined as these doctors learn specialized techniques and gain expertise in their field.

In premodern times, limited tools were used to provide health services. For example, leeches were used in bloodletting because people believed that an excess of blood caused various illnesses. Applying leeches helped “rebalance” the body by removing blood. This was used to treat headaches, seizures, and other ailments. It was also used to treat cancer and mental health conditions.
Modern times have seen a significant evolution of the tools used in providing health services. For example, in premodern times, opium was used for anesthesia during surgery. Then, inhalable gases were introduced in the mid-1800s. Today, anesthesia and anesthetics are used during surgery to minimize pain, and antiseptics are used to prevent infections during procedures.
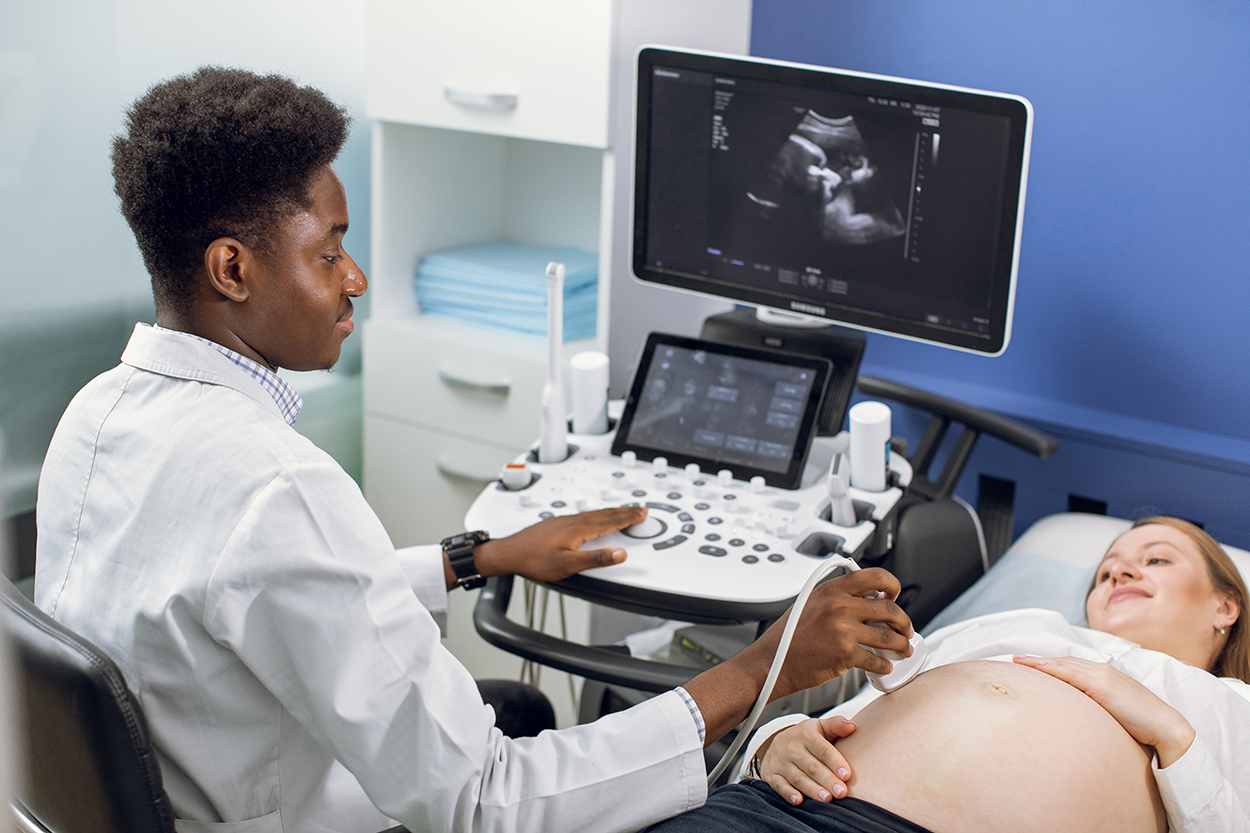
Modern times have sophisticated techniques for amputations, bone setting, and wound treatment. Now, there are modern diagnostic imaging tools like X-rays, computed tomography (CT) scans, magnetic resonance imaging (MRI), and ultrasounds, which allow for detailed imaging of organs and tissues. In premodern times, before the advances in technology led to the safer X-rays used today, early X-rays emitted dangerous levels of radiation and the images were blurry. Exposure to radiation in the early days would cause hair loss, skin burning, and blistering, and many people who volunteered to be exposed in the interest of advancing the use of X-rays died. Today, we are better equipped to limit exposure to radiation during an X-ray as modern detectors require significantly lower radiation doses than the antiquated systems (Sansare et al., 2011).
Pharmaceuticals have undergone significant advancements compared to premodern times. As mentioned earlier in this lesson, traditional medicine relied on folklore and ancient practices in premodern times. Patent medicines were commercial products sold in the 18th and 19th centuries in the United States. These over-the-counter medicines made bold claims about their curative properties. Although they were described as “patents,” they were rarely patented in the legal sense. These concoctions were marketed as “cure-alls” and relied on patient testimonials and aggressive advertising. In a time when medical practices were rudimentary, patent medicines offered an accessible alternative to costly doctor visits. However, many of these medicines contained harmful substances like mercury and opium, and their promises of effectiveness fell short (Oregon Health & Science University, 2023).

In modern times, pharmaceuticals are developed based on scientific research, clinical trials, and evidence-based medicine. They undergo rigorous testing for safety and efficacy or effectiveness. In premodern times, natural substances like herbs, minerals, and animal products were used. Formulations varied widely. In modern times, many pharmaceuticals are synthesized from chemical compounds, and their composition is standardized to ensure consistent quality and dosage. Other drugs are obtained from available natural resources such as plants and minerals (Gvalani, 2023).
Historically, drugs often came from nature, such as plant extracts or microorganisms. For instance, penicillin was discovered from the penicillin mold. It revolutionized medicine by fighting bacterial infections. Aspirin originated from willow bark and was modified to be less irritating to the stomach.
Scientists identify potential drug targets (proteins, enzymes, etc.) related to diseases. In labs, compounds are tested for safety and effectiveness (efficacy). Human trials, also known as clinical trials, involve three phases: Phase 1 is small-group testing for safety and dosage, Phase 2 is a larger group to assess effectiveness and side effects, and Phase 3 involves large-scale trials to confirm safety and efficacy.
If a drug is successful in these trials, it is submitted to regulatory agencies like the Food and Drug Administration (FDA) for approval. Pharmaceutical companies produce the drug on a large scale, and then they are distributed to hospitals, pharmacies, and patients. This process is complex and involves collaboration among scientists, doctors, and regulatory agencies (BBC Bitesize, n.d.).
As mentioned earlier, premodern times lacked evidence for practice. Their practices were shaped by tradition, anecdotes, available knowledge, and the cultural context. In modern times, however, scientific research and clinical trials produce evidence that the proposed methods are effective and safe for use.

Evidence-based public health and medicine refers to an approach that integrates the best available scientific evidence with clinical expertise and patient values. Evidence-based medicine (EBM) originated in the medical field and emphasizes using rigorous research evidence to inform clinical decisions. This involves systematic reviews that summarize existing research on specific topics; randomized controlled trials (RCTs), which compare treatments or interventions for effectiveness; and meta-analyses, which combine data from multiple studies to compare the effectiveness of treatments. EBM clinicians make informed choices about patient care based on the evidence from these various methods.
Evidence-based public health (EBPH) extends this approach to the practice of public and community health. This involves assessing evidence by evaluating the research on population health interventions and applying the evidence through implementing effective strategies based on the research findings. Monitoring and evaluation continuously assess the impact of interventions on populations. EBPH aims to improve community health by using evidence to guide policies, programs, and practices (Agency for Healthcare Research and Quality, n.d.). Evidence-based approaches enhance decision-making in both individual patient care and broader public health efforts.
Many of the developments in public health from premodern times to modern times were already discussed in this lesson. Medical technology, specialization in medicine, and the evolution of drugs from plants to laboratory science were highlighted. These achievements affected public health by generally improving health outcomes in individuals and in populations.
Some other developments from premodern times to modern times included vaccination efforts, safer workplaces, the control of infectious diseases, cleaner water, and improvements in sanitation to reduce diseases like typhoid and cholera. Adding fluoride to water reduced dental cavities. Also, during this time, medical knowledge promoted the prevention and treatment of chronic conditions like heart disease and diabetes, contributing to longer life expectancy.
Further, improved food safety practices and nutrition awareness positively impacted public health. Finally, awareness campaigns and policies highlighting the dangers of tobacco use significantly impacted public health. These achievements reflect the evolution of public health efforts over time, addressing diverse challenges from infectious diseases to lifestyle-related conditions (Centers for Disease Control and Prevention, 1999).
Source: THIS TUTORIAL WAS AUTHORED BY SOPHIA LEARNING. PLEASE SEE OUR TERMS OF USE.
Disclaimer: The use of any CDC and United States government materials, including any links to the materials on the CDC or government websites, does not imply endorsement by the CDC or the United States government of us, our company, product, facility, service, or enterprise.
REFERENCES
Agency for Healthcare Research and Quality. (n.d.). Topic: Evidence-based practice. www.ahrq.gov/topics/evidence-based-practice.html
BBC Bitesize. (n.d.). Making medicines - Edexcel. The discovery of new drugs. www.bbc.co.uk/bitesize/guides/zgh96yc/revision/1
Centers for Disease Control and Prevention. (1999, April 2). Morbidity and mortality weekly report. www.cdc.gov/mmwr/PDF/wk/mm4812.pdf
Gvalani, A. (2023, October 19). How are medicines made? ScienceABC.com. www.scienceabc.com/pure-sciences/how-are-medicines-made.html
Kong, X., Gao, P., Wang, J., Fang, Y., & Hwang, K. C. (2023). Advances of medical nanorobots for future cancer treatments. Journal of Hematology & Oncology, 16, Article 74. doi.org/10.1186/s13045-023-01463-z
Oregon Health & Science University. (2023, October). There’s a cure for that: Historic medicines and cure-alls in America. www.ohsu.edu/historical-collections-archives/theres-cure-historic-medicines-and-cure-alls-america
Penn Nursing. (n.d.). American nursing: An introduction to the past. www.nursing.upenn.edu/nhhc/american-nursing-an-introduction-to-the-past/
Sansare, K., Khanna, V., & Karjodkar, F. (2011). Early victims of X-rays: A tribute and current perception. Dentomaxillofacial Radiology, 40(2), 123–125. doi.org/10.1259%2Fdmfr%2F73488299