Table of Contents |
The kidneys lie on either side of the spine in the retroperitoneal space between the parietal peritoneum and the posterior abdominal wall, well protected by muscle, fat, and ribs. They are roughly the size of your fist, and the male kidney is typically a bit larger than the female kidney. The kidneys are well vascularized, receiving about 25% of the cardiac output at rest.
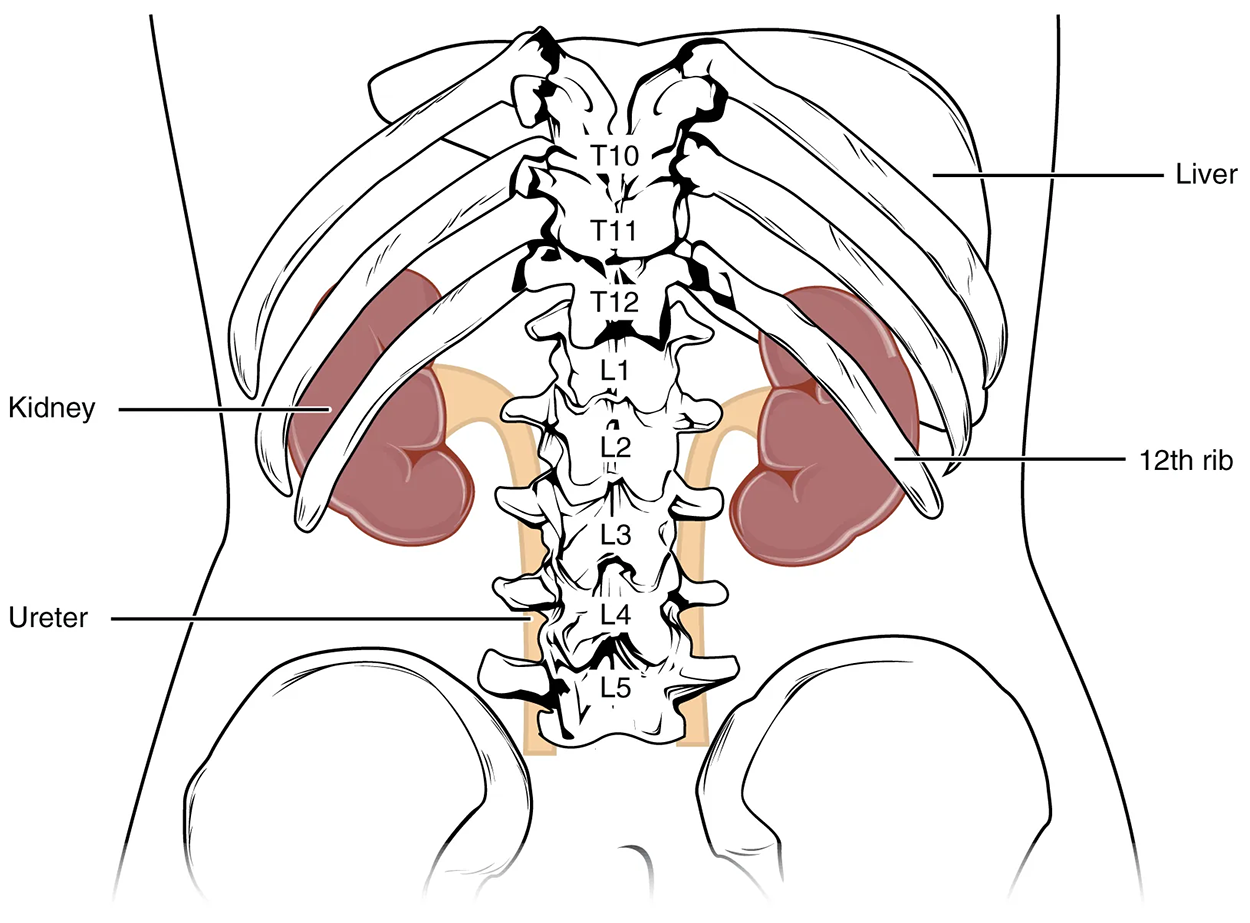
On the superior aspect of each kidney lies the adrenal gland. The adrenal cortex directly influences renal function through the production of the hormone aldosterone to stimulate sodium reabsorption.
A frontal section through the kidney reveals an outer region called the renal cortex, which contains most of the nephrons, and an inner region called the renal medulla. The renal columns are connective tissue extensions that radiate downward from the cortex through the medulla to separate the most characteristic features of the medulla: the renal pyramids and renal papillae. The papillae are bundles of collecting ducts that transport urine made by nephrons to the calyces of the kidney for excretion. The renal columns also divide the kidney into 6–8 lobes and provide a supportive framework for vessels that enter and exit the cortex. The pyramids and renal columns taken together constitute the kidney lobes.
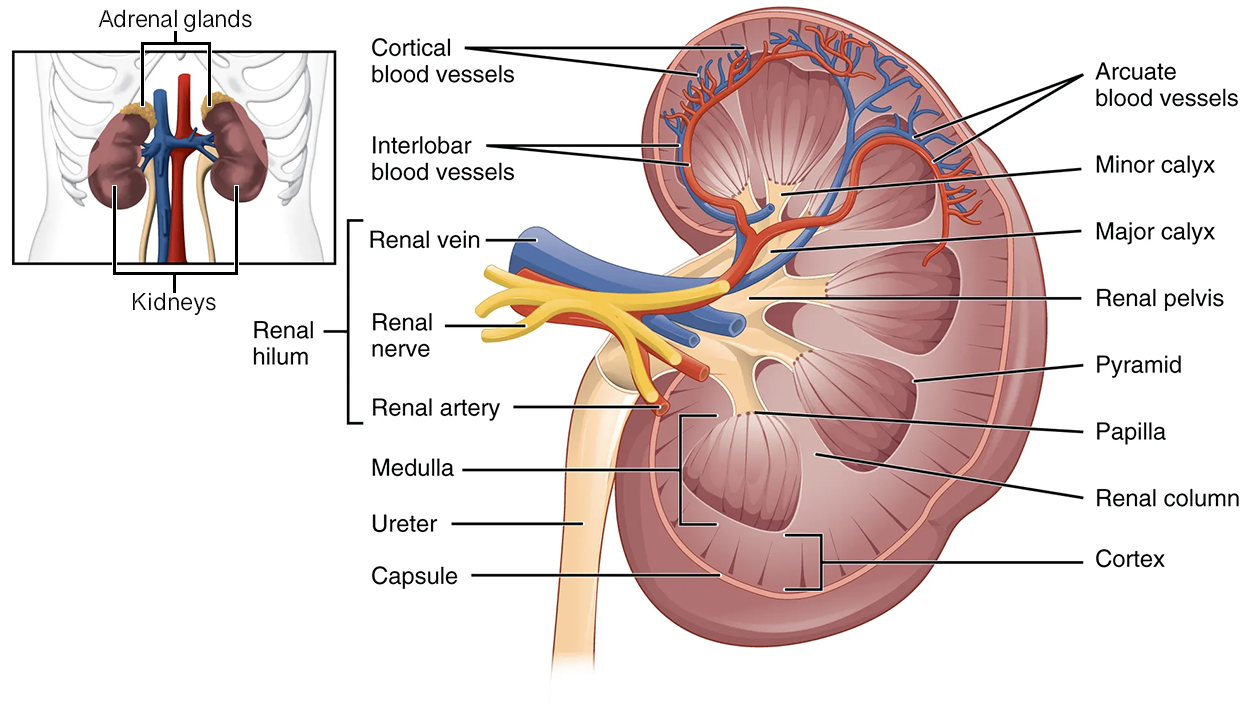
The renal hilum is the entry and exit site for structures servicing the kidneys: blood vessels, nerves, lymphatic vessels, and ureters. Emerging from the hilum is the renal pelvis, which is formed from the major and minor calyces in the kidney and is located in the renal sinus, which is a cavity that extends behind the renal hilum and includes the renal pelvis, blood vessels, nerves, and fat. The smooth muscle in the renal pelvis funnels urine via peristalsis (involuntary contractions similar to those that move food through the digestive tract) into the ureter. The renal arteries form directly from the descending aorta, whereas the renal veins return cleansed blood directly to the inferior vena cava.
The kidneys regulate the composition and volume of bodily fluids by filtering waste and excess water from the blood. This process starts when blood enters either kidney through the renal arteries (“renal” means having to do with the kidneys). It then passes through microscopic tubes called nephrons, which do the actual filtering. From there, the filtered blood leaves the kidney through the renal veins. The waste and excess water removed by the nephrons become urine, which flows through the renal pelvis out of the kidney and into the ureter.
Most nephrons are found in the renal cortex (the outer layer of the kidneys), but they also reach into the renal medulla (the inner layer of the kidneys).
The renal artery first divides into segmental arteries, followed by further branching to form interlobar arteries that pass through the renal columns to reach the cortex. The interlobar arteries, in turn, branch into arcuate arteries, cortical radiate arteries, and then into afferent arterioles, which supply blood to the nephrons. The afferent arterioles service approximately 1.3 million nephrons in each kidney.
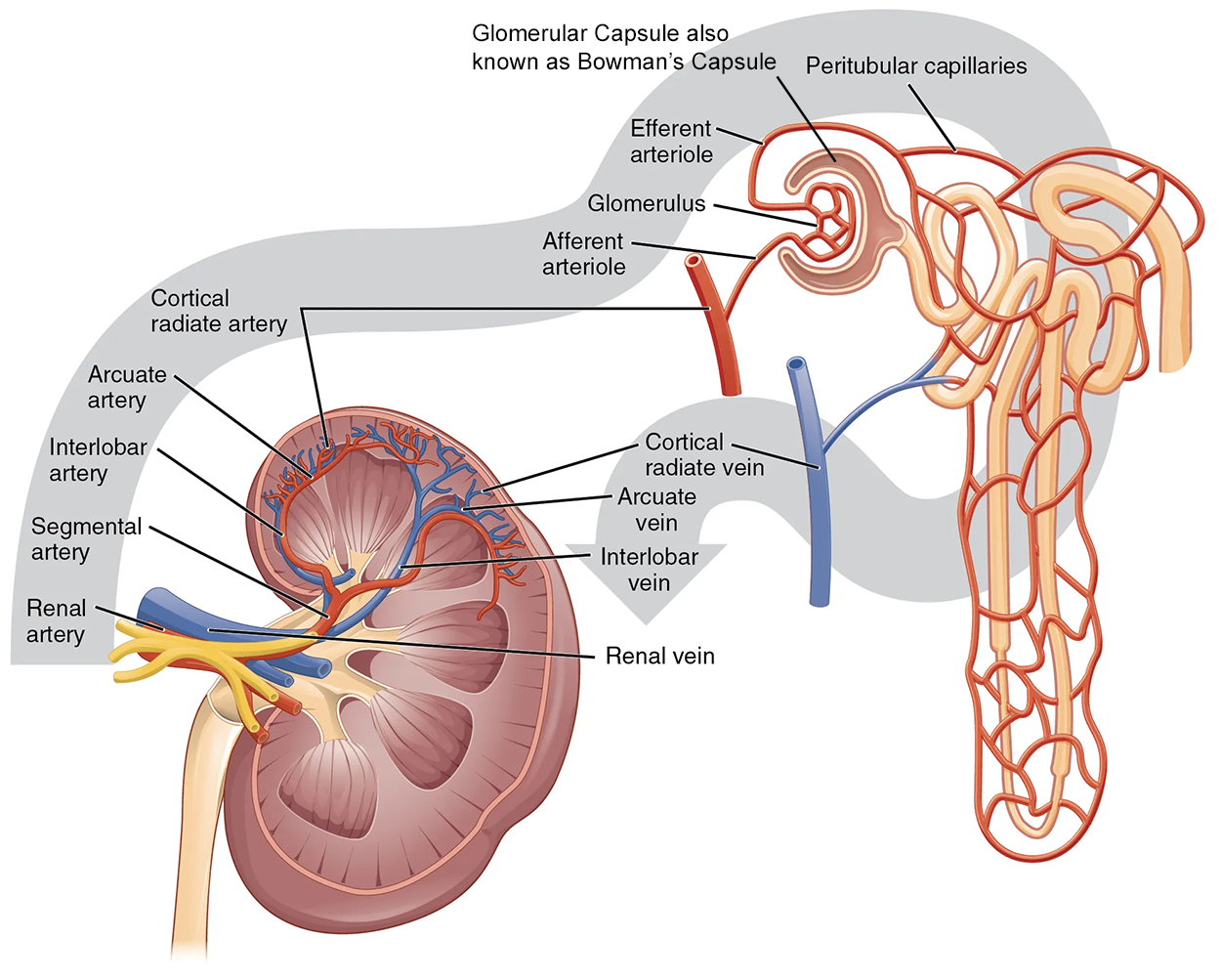
Nephrons are the “functional units” of the kidney; they cleanse the blood and balance the constituents of the circulation. The afferent arterioles form a tuft of high-pressure capillaries about 200 µm in diameter, the glomerulus. The rest of the nephron consists of a continuous sophisticated tubule whose proximal end surrounds the glomerulus in an intimate embrace—this is the Bowman’s capsule. The glomerulus and Bowman’s capsule together form the renal corpuscle.
These glomerular capillaries filter the blood based on particle size. After passing through the renal corpuscle, the capillaries form a second arteriole, the efferent arteriole. These will next form a capillary network around the more distal portions of the nephron tubule, the peritubular capillaries and vasa recta, before returning to the venous system.
As the glomerular filtrate progresses through the nephron, these capillary networks recover most of the solutes and water and return them to the circulation. Because a capillary bed (the glomerulus) drains into a vessel that in turn forms a second capillary bed, this is considered a portal system (a system where veins start and end in capillaries without going through the heart first).
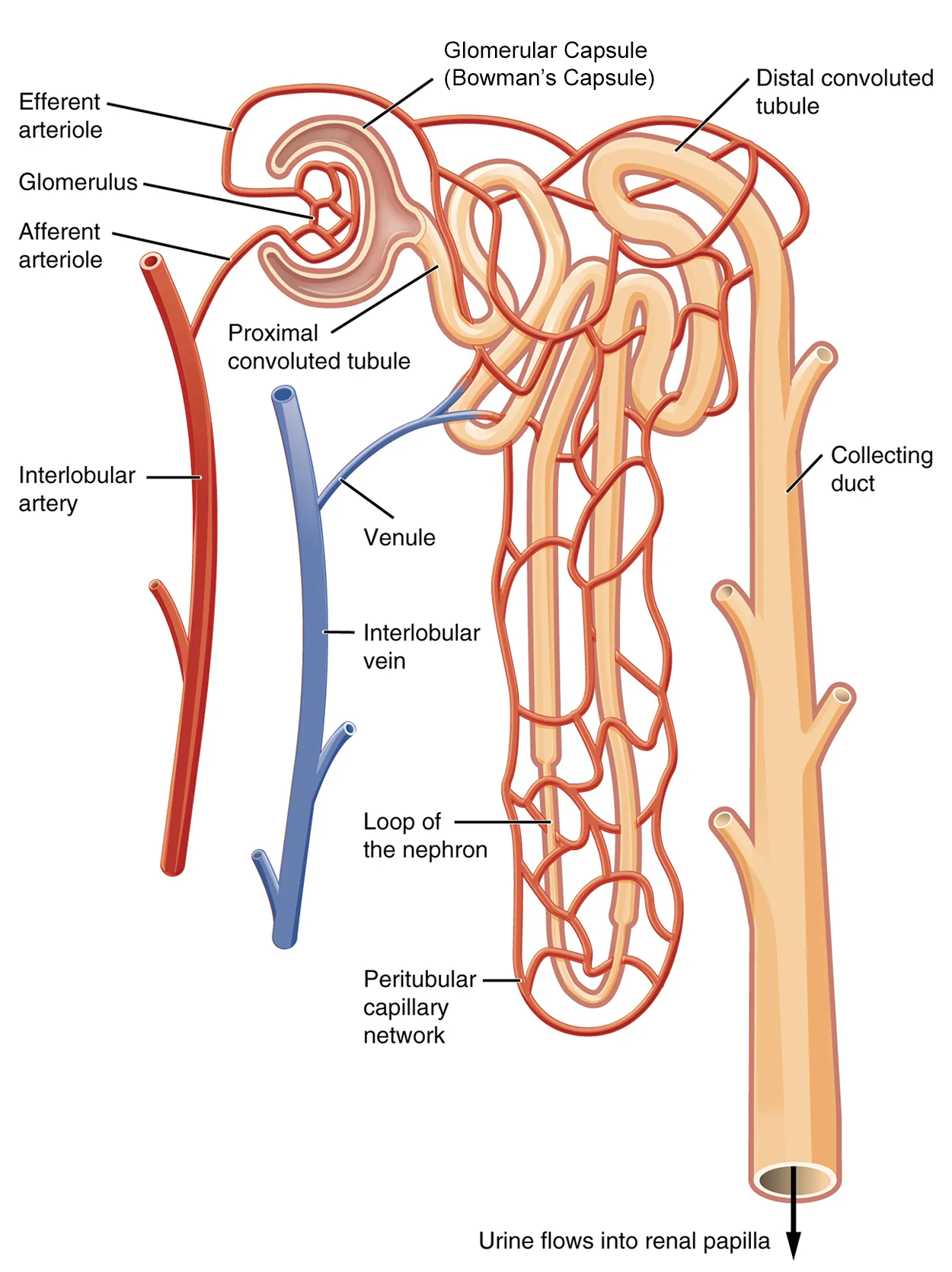
All of the renal corpuscles as well as both the proximal convoluted tubules (PCTs) and distal convoluted tubules (DCTs) are found in the cortex of the kidney. Some nephrons have a short loop of Henle that does not dip beyond the cortex. These nephrons are called cortical nephrons. About 15% of nephrons have long loops of Henle that extend deep into the medulla and are called juxtamedullary nephrons.
IN CONTEXT
Career Connection
Nephrologist
A nephrologist studies and deals with diseases of the kidneys—both those that cause kidney failure (such as diabetes) and the conditions that are produced by kidney disease (such as hypertension). Blood pressure, blood volume, and changes in electrolyte balance come under the purview of a nephrologist.
Nephrologists usually work with other physicians who refer patients to them or consult with them about specific diagnoses and treatment plans. Patients are usually referred to a nephrologist for symptoms such as blood or protein in the urine, very high blood pressure, kidney stones, or renal failure.
Nephrology is a subspecialty of internal medicine. To become a nephrologist, medical school is followed by additional training to become certified in internal medicine. An additional two or more years is spent specifically studying kidney disorders and their accompanying effects on the body.
SOURCE: THIS TUTORIAL HAS BEEN ADAPTED FROM OPENSTAX “ANATOMY AND PHYSIOLOGY 2E”. ACCESS FOR FREE AT OPENSTAX.ORG/BOOKS/ANATOMY-AND-PHYSIOLOGY-2E/PAGES/1-INTRODUCTION. LICENSE: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.