Table of Contents |
In this lesson, you will learn about varied procedures used to treat female reproductive system conditions.
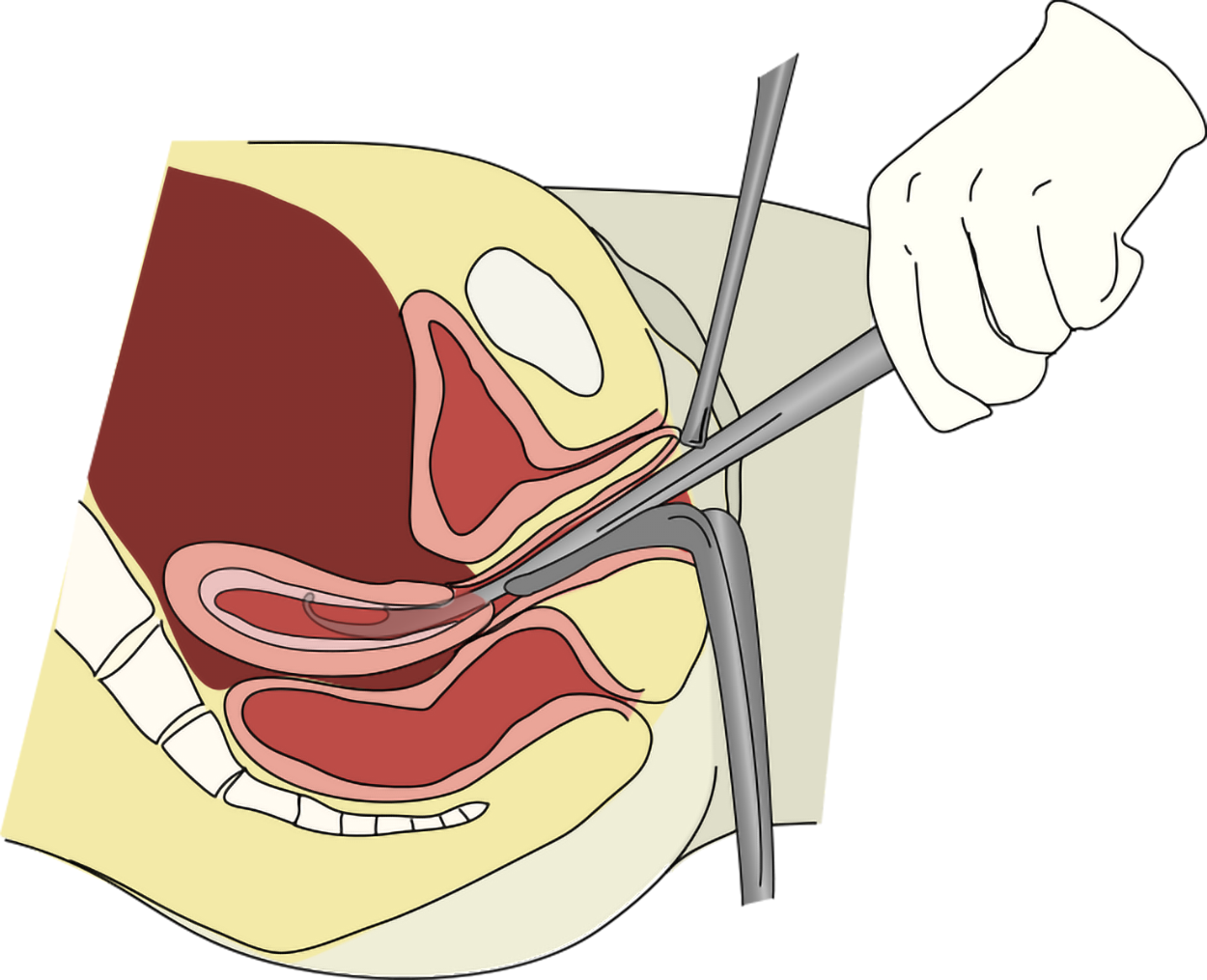
Dilation and curettage (D&C) is a procedure performed by a physician in which the opening of the cervix is stretched so that a surgical tool can be inserted into the uterus to scrape away the excess endometrial lining. The removed lining is then biopsied for abnormal tissue. A D&C can be performed to determine the cause of abnormal vaginal bleeding, as well as to treat it.
The figure below shows an illustration of a D&C.
A hysterectomy is a surgery used to treat a variety of disorders, such as dysfunctional uterine bleeding, fibroids, severe endometriosis, endometrial cancer, and ovarian cancer. There are several types of hysterectomies.
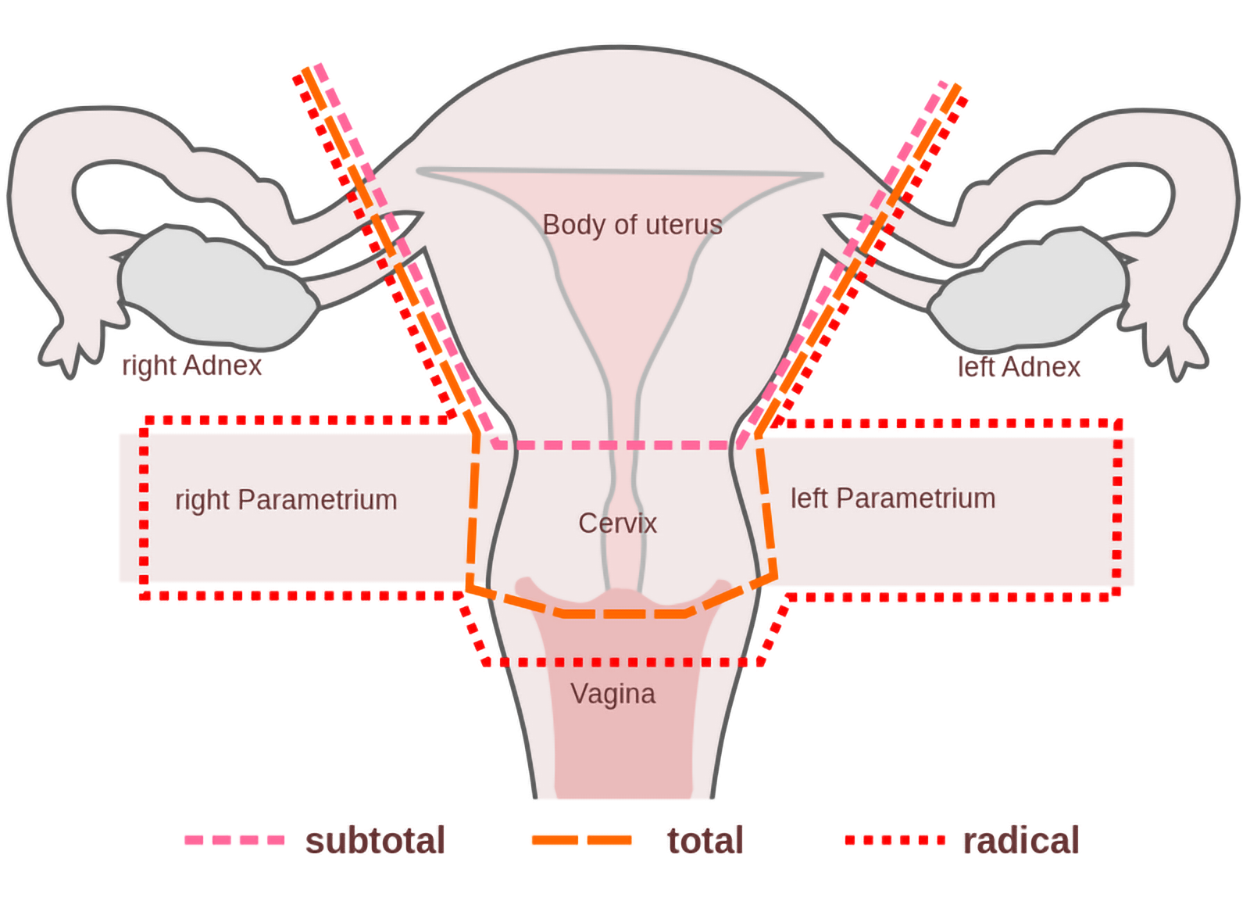
Total hysterectomy is surgery to remove the uterus, including the cervix. If the uterus and cervix are taken out through the vagina, the operation is called a vaginal hysterectomy. If the uterus and cervix are taken out through a large incision in the abdomen, the operation is called a total abdominal hysterectomy. If the uterus and cervix are taken out through a small incision in the abdomen using a laparoscope, the operation is called a total laparoscopic hysterectomy. A subtotal hysterectomy removes part of the uterus but leaves the cervix intact.
Radical hysterectomy is surgery to remove the uterus, cervix, and part of the vagina. The ovaries, uterine tubes (fallopian tubes), or nearby lymph nodes may also be removed during this procedure, referred to as a total hysterectomy/bilateral salpingectomy oophorectomy (TAH/BSO). An oophorectomy is the surgical removal of one or more ovaries. A bilateral oophorectomy is the removal of both ovaries. A salpingectomy is the removal of a uterine tube (fallopian tube). A salpingo-oophorectomy is the removal of one uterine tube (fallopian tube) and the associated ovary, or sometimes both uterine tubes and ovaries. Bilateral salpingo-oophorectomy means removal of both ovaries and uterine tubes (fallopian tubes).
The figure below shows how different types of hysterectomies compare.
A hysterosalpingogram is a common imaging procedure performed to assess for potential causes of infertility in women. During the procedure, radiopaque dye is injected into the uterus and fills the uterine cavity, continues into the uterine tubes (fallopian tubes), and eventually reaches the fimbriated ends next to the ovaries. Structures are visualized with an X-ray.
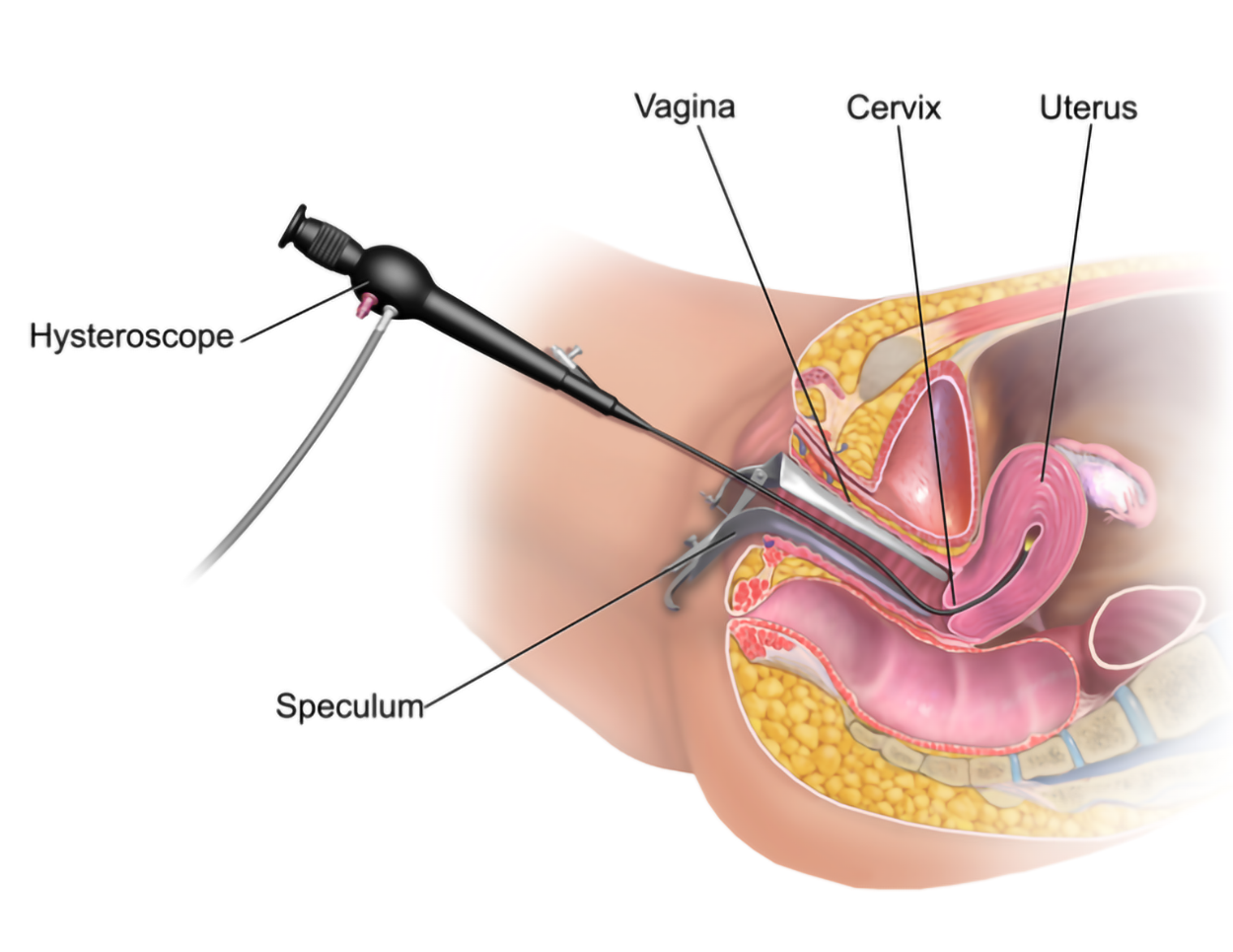
A hysteroscopy, shown in the illustration above, is a procedure to visually examine the uterus for abnormal areas. A hysteroscope is a thin, tube-like instrument with a light and a lens for viewing and is inserted through the vagina and cervix into the uterus. It may also have a tool to remove tissue samples, which are examined under a microscope for signs of cancer.
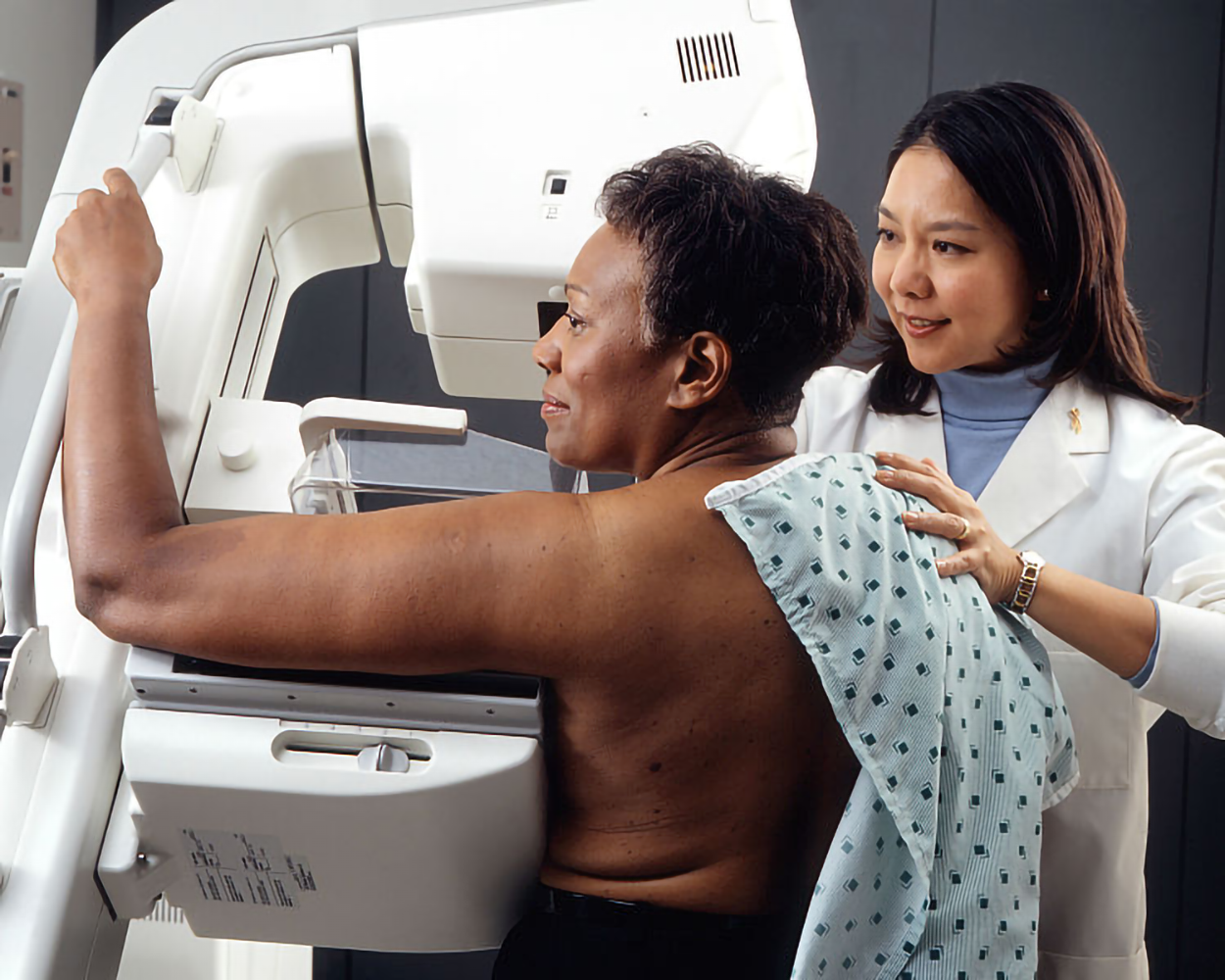
A mammogram, shown above, is a radiographic image of breast tissue to detect signs of breast cancer. At present, many mammograms are actually tomosynthesis, sometimes marketed as a 3D mammogram. Tomosynthesis differs from traditional mammograms in that more images are taken (as opposed to just two), and then these images are used to produce a 3D image for analysis (Hadjipanteli et al., 2018).
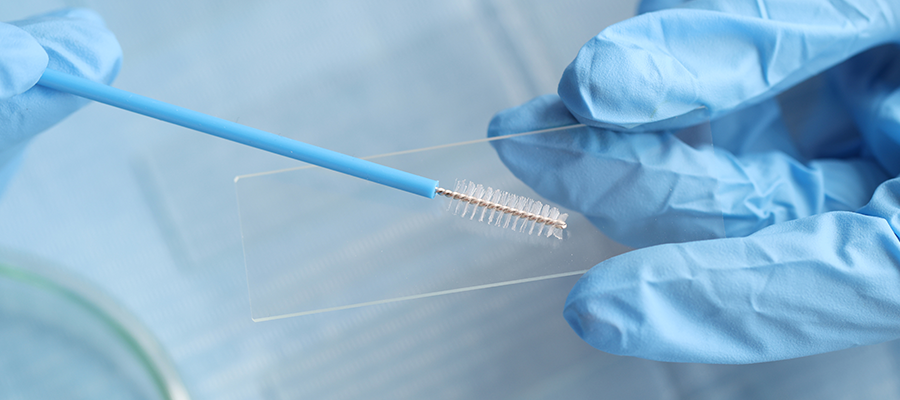
A Papanicolaou smear or Pap smear is a diagnostic test that screens for suspicious changes in cells of the cervix. During a Pap smear, a health care provider inserts a speculum into the vagina to allow visualization of the cervix. Cells are collected from the cervix using sterile swabs and/or cytobrushes and sent to a lab for analysis for abnormal cells or cancer.
The figure below shows a cytobrush used to collect cervical cell samples during a Pap smear.
A transvaginal ultrasound is a procedure used to examine the vagina, uterus, uterine tubes (fallopian tubes), and bladder. An ultrasound transducer (probe) is inserted into the vagina and used to bounce high-energy sound waves (ultrasound) off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram.
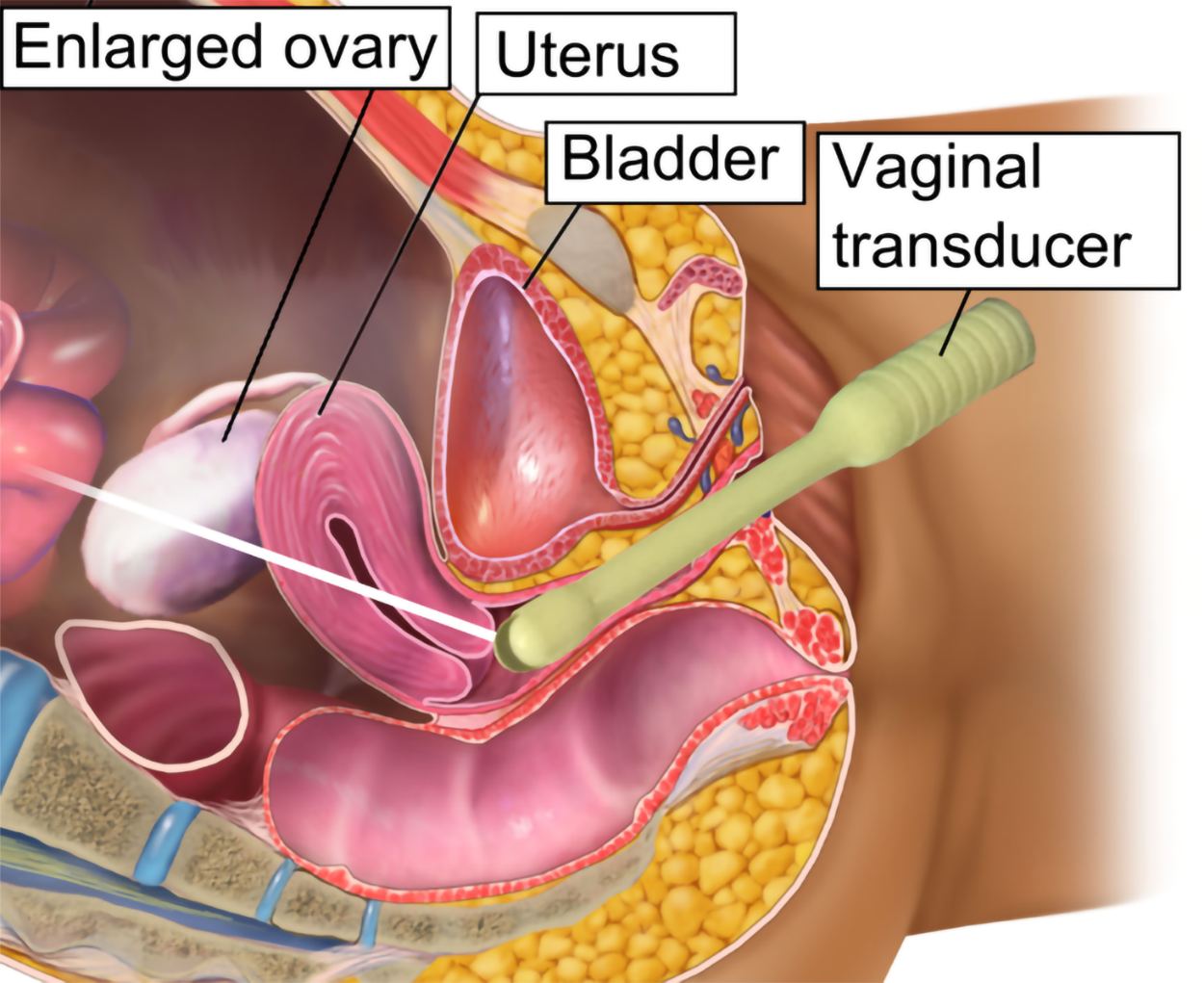
The figure above shows an illustration of the ultrasound transducer placement during a transvaginal ultrasound.
There are a variety of types of treatments that can be used to treat infertility, which is common and has many different causes. The cause of the infertility affects which treatments are appropriate. These can include medications that affect egg and sperm production, as well as natural family planning methods that involve tracking basal body temperature. Sometimes, efforts to improve health (such as improving nutrition and moderating excessive exercise) can help. Some surgeries can be available for both men and women (for example, if there is a blockage in a uterine tube or an ejaculatory duct in men). Uterine fibroids can also be removed using surgery (Cleveland Clinic, 2022a and Cleveland Clinic, 2023).
Assistive reproductive technologies (ART) are more involved approaches. In ART, a clinician intervenes in a way that manipulates the egg, sperm, or both. Examples of ART include intracytoplasmic sperm injection (ICSI), which involves injecting a sperm into an egg prior to returning up to three embryos produced this way into the uterus. Intrauterine insemination (IUI) involves helping sperm reach the egg by using a tube to insert sperm into the uterus (Cleveland Clinic, 2023a).
In vitro fertilization (IVF) is an assisted reproductive technology. There are many different indications for IVF.
EXAMPLE
A woman may produce normal eggs, but the eggs cannot reach the uterus because the uterine tubes are blocked or otherwise compromised. A man may have a low sperm count, low sperm motility, sperm with an unusually high percentage of morphological abnormalities, or sperm that are incapable of penetrating the zona pellucida of an egg. IVF can also be used for women who need medical treatment, such as cancer treatment, that may affect future fertility; a woman can have eggs stored for future use (men can also store sperm for fertility preservation; Cleveland Clinic, 2022b).There are five basic steps of IVF.
There are many challenging ethical issues related to assistive reproductive technologies, and many people have strong personal beliefs about them.
EXAMPLE
IVF may involve producing more embryos than are used in treatment, leading to difficult decisions about what to do with the embryos not used (Cleveland Clinic, 2022b). At the same time, people who pursue these approaches may have experienced considerable stress, disappointment, worry, and expense.The primary function of contraception is to prevent pregnancy. It is important to remember that contraception does not typically prevent the transmission of STIs, with the exception of condoms that are used properly. Contraception can involve the use of hormones, barrier methods that prevent sperm from reaching an egg, and behaviors such as tracking basal body temperature for natural family planning approaches.
Choosing a method of birth control requires carefully considering personal preferences and needs, as well as what is most likely to be effective. It is also important to consider whether protection from disease transmission is needed (Cleveland Clinic, 2022c).
Except for abstinence, all methods of birth control involve some risk of failure. For people who need to be especially careful (for example, if a medical condition means that pregnancy could be dangerous), using two methods is recommended (Cleveland Clinic, 2022c).
Hormonal birth control uses hormonal manipulation to reduce the possibility of pregnancy. A variety of types are available, including some that are for shorter-term use and others that are for longer-term use.
Birth control pills take advantage of the negative feedback system that regulates the ovarian and menstrual cycles to stop ovulation and prevent pregnancy. Typically, they work by providing a constant level of both estrogen and progesterone, which negatively feed back onto the hypothalamus and pituitary, thus preventing the release of FSH and LH. Without FSH, the follicles do not mature, and without the LH surge, ovulation does not occur. Although the estrogen in birth control pills does stimulate some thickening of the endometrial wall, it is reduced compared with a normal cycle and is less likely to support implantation.
Some birth control pills contain 21 active pills containing hormones, and 7 inactive pills (placebos). The decline in hormones during the week that the person takes the placebo pills triggers menses, although it is typically lighter than a normal menstrual flow because of the reduced endometrial thickening. Newer types of birth control pills have been developed that deliver low-dose estrogens and progesterone for the entire cycle (these are meant to be taken 365 days a year), and menses never occurs. While some people prefer to have the proof of a lack of pregnancy that a monthly period provides, menstruation every 28 days is not required for health reasons, and there are no reported adverse effects of not having a menstrual period in an otherwise healthy individual.
Because birth control pills function by providing constant estrogen and progesterone levels and disrupting negative feedback, skipping even just one or two pills at certain points of the cycle (or even being several hours late taking the pill) can lead to an increase in FSH and LH and result in ovulation. It is important, therefore, to follow the directions on the birth control pill package to successfully prevent pregnancy.
Birth control pills are very effective if used exactly as prescribed, but have to be taken daily, and some medications interfere with their effectiveness. Therefore, they can be convenient, but have a higher risk of failure than approaches that do not require daily action (Cleveland Clinic, 2023b).
Intrauterine devices (IUDs) can contain hormones, although one type contains copper. These T-shaped devices are inserted into the uterus and function for 3–10 years, depending on the type. They typically prevent thickening of the uterine lining, among other effects.
Barrier birth controls physically prevent fertilization from occurring. They include spermicides (chemicals that kill sperm) and a vaginal diaphragm that can be inserted into the vagina (used with either a special gel or a spermicide).
Condoms are of particular importance because they can prevent the transmission of sexually transmitted infections. A condom is a sheath that is worn on the penis during sexual intercourse to capture ejaculate, preventing sperm from reaching an egg.
Sterilization is a procedure that produces permanent protection against pregnancy. One method of sterilization is tubal ligation. Tubal ligation is a surgical procedure performed to prevent pregnancy and is also called female sterilization and commonly referred to as “getting your tubes tied.” “Tubal” refers to the uterine tubes (fallopian tubes), and “ligation” means to tie off. During this surgery, both uterine tubes (fallopian tubes) are blocked or cut to prevent fertilization of the egg by sperm. The procedure is usually performed in the hospital or in an outpatient surgical clinic. After the procedure, the woman still has a monthly menstrual cycle and menstrual flow.
Source: THIS TUTORIAL HAS BEEN ADAPTED FROM “OPEN RN | MEDICAL TERMINOLOGY – 2e” BY ERNSTMEYER & CHRISTMAN AT OPEN RESOURCES FOR NURSING (Open RN). ACCESS FOR FREE AT https://wtcs.pressbooks.pub/medterm/ LICENSING: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.
REFERENCES
Hadjipanteli, A., Kontos, M., & Constantinidou, A. (2019). The role of digital breast tomosynthesis in breast cancer screening: A manufacturer- and metrics-specific analysis. Cancer Management and Research, 11, 9277–9296. doi.org/10.2147/CMAR.S210979
Toxic Shock Syndrome. (2022, August 18). Cleveland Clinic. Toxic Shock Syndrome (TSS): Causes, Symptoms & Treatment
Pap Smear. (2024, August 19). Cleveland Clinic. Pap Smear: Test, Age, Duration, Results & Frequency
Ejaculatory Duct Obstruction. (2022a, April 10). Cleveland Clinic. Ejaculatory Duct Obstruction: Causes, Symptoms & Surgery
Infertility. (2023, April 19). Cleveland Clinic. Infertility: Types, Causes, Symptoms, Diagnosis & Treatment
Embryo Freezing. (2022b, February 17). Cleveland Clinic. Embryo Freezing (Cryopreservation): Purpose & Results
Birth Control. (2022c, August 18). Cleveland Clinic. Birth Control: Forms, Options, Risks & Effectiveness
Birth Control Pills. (2023b, July 5). Cleveland Clinic. Birth Control Pill: Types, Side Effects & Effectiveness