In this lesson, you will determine the purpose and process of quality improvement in healthcare. You will explore the process used to improve healthcare and processes for staff. You will read examples of how it is used in the real world and determine its benefits. Specifically, this lesson will cover:
1. What Is Continuous Quality Improvement (CQI)?
Continuous quality improvement (CQI) is a process used by healthcare organizations to improve their systems, practices, and outcomes over time. The idea behind CQI is simple: No matter how well a healthcare system is performing, there is always room for improvement. It focuses on making small, gradual changes that lead to big improvements in patient care and the overall healthcare experience.
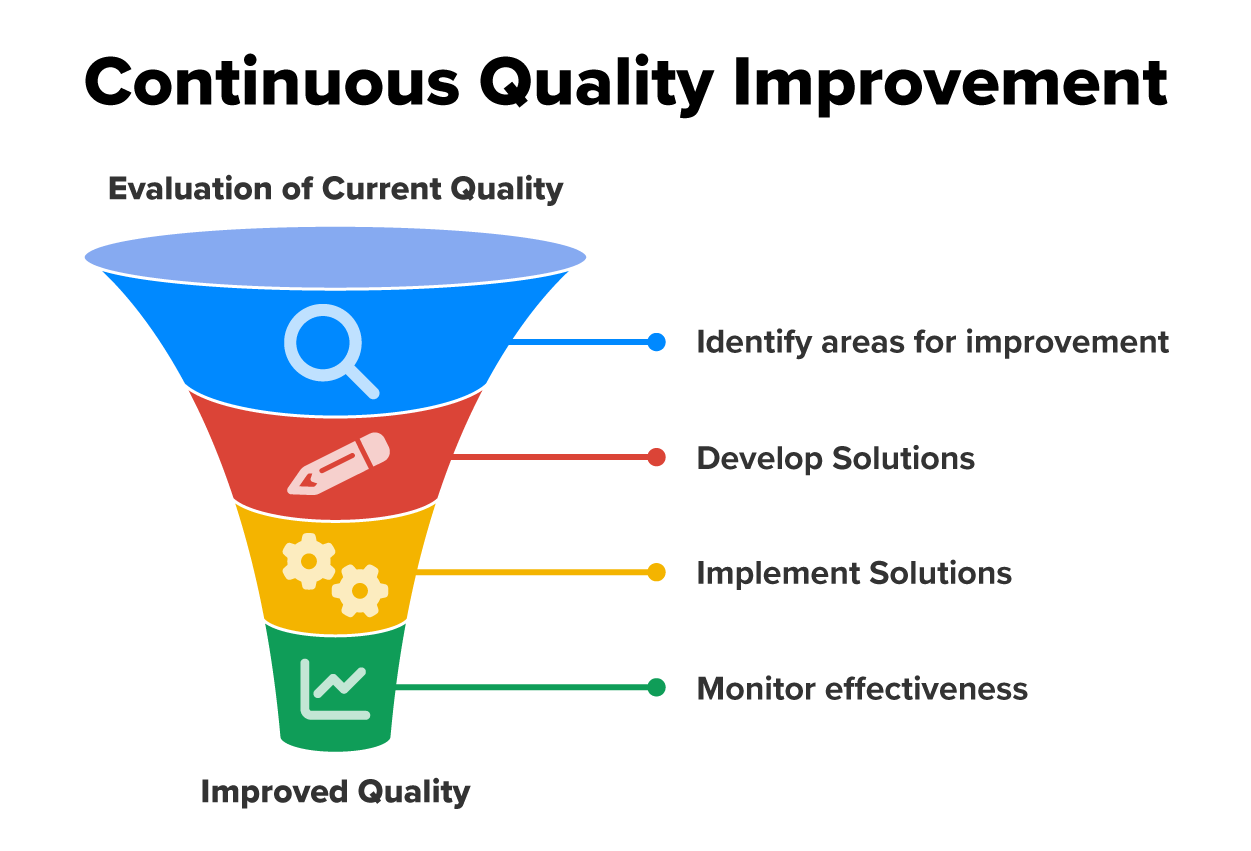
CQI is not a one-time fix. Instead, it’s an ongoing process where healthcare professionals continuously assess and evaluate their work, identify problems, and find solutions. Remember that the “C” stands for “continuous,” meaning that it is an ongoing process. The goal is not only to solve problems but to prevent them from happening in the future. It uses a cyclical process where areas for improvement are identified, then a team is used to identify solutions. Next, the solutions are implemented, and then, after some time, the team evaluates if the solutions were effective.
CQI is a data-driven decision-making process. It relies on data to identify areas for improvement rather than just relying on thoughts, assumptions, or opinions. This involves collecting and analyzing data on various aspects of healthcare services. Measuring the impact of any changes made also relies on collected data. CQI is also patient-focused. Since the primary goal of CQI is often to improve patient care, this means that putting the needs and preferences of patients at the center of all improvement efforts is crucial. The data needed to do this often comes from patient satisfaction surveys that tell us where there may be opportunities for improvement.
-
As a healthcare manager, you may be required to participate on a CQI team, or you may even be inclined to lead a CQI initiative in your department. By focusing on improving quality over time, healthcare organizations can make the system more efficient, cost-effective, and, most importantly, safer for patients.
-
- Continuous Quality Improvement (CQI)
- A process used by healthcare organizations to improve their systems, practices, and outcomes over time.
2. The Purpose of Continuous Quality Improvement in Healthcare
The purpose of CQI in healthcare is to ensure that patients receive high-quality care consistently, and to assist with improving processes within a healthcare organization. By focusing on quality improvement, healthcare providers can reduce errors, reduce inefficiencies, increase patient satisfaction, and improve the health outcomes of patients. In essence, CQI helps healthcare professionals deliver better care and services to those who need it most.
There are several key purposes of CQI in healthcare that you will explore next.
2a. Improving Patient Safety
One of the most important goals of CQI is to reduce the risk of medical errors. Medical errors, such as incorrect diagnoses, medication mistakes, or surgical errors, can have serious consequences for patients. By regularly assessing their practices and looking for ways to improve, healthcare organizations can minimize these errors and create a safer environment for patients.
2b. Enhancing Efficiency
Healthcare systems can sometimes be slow or inefficient, leading to delays in treatment or unnecessary procedures. CQI helps healthcare organizations identify inefficiencies in their processes and implement solutions to make them faster and more effective. For example, improving patient flow in hospitals can reduce waiting times, making it easier for patients to receive the care they need in a timely manner.
2c. Increasing Patient Satisfaction
Patient satisfaction is another important goal of CQI. When patients are satisfied with their care, they are more likely to follow treatment plans and return for follow-up care. By improving communication, addressing patient concerns, and providing personalized care, healthcare organizations can enhance patient satisfaction, leading to better overall outcomes.
2d. Cost-Effectiveness
CQI also helps healthcare organizations manage costs. By streamlining processes, reducing waste, and improving resource management, CQI can help healthcare facilities save money without compromising the quality of care. This is especially important in today’s healthcare environment, where budgets can be tight, and resources are limited.
2e. Promoting Teamwork and Collaboration
Continuous quality improvement encourages collaboration among healthcare professionals. Doctors, nurses, administrators, and other staff work together to identify problems, discuss solutions, and implement changes. This team-based approach leads to a more cooperative and supportive work environment, which benefits both staff and patients.
IN CONTEXT
There are many ways CQI can be applied in healthcare. Here are some examples of how it is used to improve patient care and outcomes:
Improving Hand Hygiene Practices
One common CQI initiative is improving hand hygiene among healthcare workers. Studies have shown that proper hand hygiene is one of the most effective ways to prevent the spread of infections in healthcare settings. If a hospital notices that hand hygiene compliance is low among staff, they might use CQI methods to improve the situation. They could implement a plan to remind staff to wash their hands before and after patient care, track compliance, and provide education on the importance of hand hygiene. Over time, as compliance improves, the hospital would evaluate the effectiveness of the changes and adjust them as necessary.
Reducing Hospital Readmissions
Another area where CQI is commonly used is in reducing hospital readmissions. When patients are discharged from the hospital, some may return for additional treatment or complications. This can be costly and lead to poor health outcomes. To address this, hospitals might use CQI to improve discharge planning, provide follow-up care, and ensure that patients understand how to manage their conditions after leaving the hospital. Through monitoring and analyzing patient outcomes, hospitals can identify strategies to reduce readmissions and improve patient care.
Improving Patient Flow in Emergency Rooms
As mentioned earlier, improving patient flow is another important CQI goal. Long waiting times in emergency rooms (ERs) are a common concern in healthcare systems around the world. Using CQI, an ER might implement a system to prioritize patients based on the severity of their condition, streamline the check-in process, and increase staff during busy times. By testing and refining these changes, the ER can reduce waiting times, improve patient satisfaction, and make the entire process more efficient.
-
- Hospital Readmission
- The process of a patient being admitted to the hospital again within a specified time period after being discharged, often due to complications or incomplete recovery from the initial illness or procedure.
3. The Process of Continuous Quality Improvement
The process of continuous quality improvement (CQI) in healthcare involves a systematic approach to improving the quality of services and outcomes through continuous assessment, planning, implementation, and evaluation. The goal is to make ongoing, incremental improvements that lead to better patient care, increased safety, higher satisfaction, and more efficient use of resources.
CQI is based on the principle that improvements are always possible, and it requires a commitment to regularly assess and refine processes.
-
Following is a step-by-step breakdown of how CQI works.
1. Identifying the Problem or Area for Improvement
The first step in the CQI process is to identify areas where improvement is needed. This can be done through:
- Data collection: Reviewing patient outcomes, safety reports, and performance metrics.
- Patient feedback: Gathering input from patients about their experiences and satisfaction with care.
- Staff feedback: Listening to the perspectives of healthcare providers and staff members who work directly with patients.
- Performance analysis: Examining any patterns or trends that suggest problems, such as high readmission rates, long wait times, or errors in medication administration.
For example, a hospital may notice that patients in the emergency department (ED) are waiting too long before being seen by a doctor. This could be an area identified for improvement.
2. Setting Goals and Defining Success
Once the area for improvement is identified, the next step is to set clear and measurable goals. These goals should be specific, achievable, and relevant to the problem at hand. In this example, the goal might be to reduce patient wait times in the ED by 20% within 6 months.
Defining success helps focus efforts on specific outcomes, such as improving patient flow, enhancing staff efficiency, or increasing patient satisfaction.
3. Planning Solutions and Interventions
After setting goals, the next step is to develop a plan to address the identified problem. This plan should outline specific interventions or strategies that will be implemented to improve the situation. These interventions might include:
- Process redesign: Changing the way work is organized, such as improving patient triage procedures or adding more staff during peak hours.
- Staff training: Educating healthcare workers on new protocols or best practices that could improve care delivery.
- Technology use: Implementing new technologies, like patient tracking systems or electronic health records, to streamline workflows.
For example, the hospital may decide to implement a new triage system where patients with the most urgent needs are seen first, or they might adjust staffing schedules to ensure more doctors and nurses are available during busy hours.
4. Implementing the Plan (Doing)
Once the plan is developed, the next step is to put it into action. This phase involves:
- Training staff: Ensuring that everyone involved understands the new procedures and their roles.
- Piloting interventions: In some cases, it may be helpful to test the changes on a small scale before rolling them out across the entire system.
- Collecting data: During the implementation phase, it’s important to track data to see how the changes are working. For example, the hospital may start tracking patient wait times immediately after the new triage process is implemented.
At this stage, healthcare professionals monitor the implementation closely to identify any challenges or unexpected issues.
5. Measuring and Evaluating Outcomes (Studying)
After the intervention is implemented, it’s time to measure and assess the outcomes. This phase involves:
- Collecting data: Gathering quantitative and qualitative data to see if the interventions are having the desired effect. For example, the hospital might compare the new patient wait times with baseline data to determine if the goal was met.
- Reviewing performance: Analyzing data and feedback to understand how well the intervention worked. If wait times decreased and patients reported higher satisfaction, the intervention would be considered successful.
- Identifying areas for improvement: Even if the intervention is successful, there may still be aspects that could be improved further. Continuous evaluation ensures that the process of improvement continues.
In the case of the hospital’s ED, they would look at how the new triage system impacted wait times and whether it led to better patient outcomes, such as fewer patients leaving without being seen.
6. Adjusting and Refining (Acting)
Based on the results of the evaluation, adjustments and refinements are made. This step ensures that improvements are sustained and that the process continues to evolve. The actions taken during this phase can include:
- Scaling up: If the changes were successful in a small test area, they can be expanded to the entire system or organization.
- Refining the plan: If the data shows areas for improvement, the plan can be adjusted to better meet the goal. For example, if wait times improved but not as much as expected, the hospital might tweak the triage system or add more staff.
- Standardizing successful practices: Once the desired outcomes are achieved, the improved processes can be standardized and implemented across the organization.
7. Sustaining Improvements and Repeating the Cycle
Continuous quality improvement is an ongoing process. Once improvements are made and successful changes are implemented, the organization continues to monitor performance to ensure the changes are sustained over time. The cycle is repeated periodically to drive further improvements.
For example, after reducing wait times in the ED, the hospital might begin looking at other areas of care, such as improving discharge processes or reducing medication errors. Each area of improvement follows the same cycle of planning, implementing, evaluating, and adjusting.
In this lesson, you determined the purpose and process of quality improvement in healthcare. What is continuous quality improvement (CQI)? CQI is a process used by healthcare organizations to improve their systems, practices, and outcomes over time. The purpose of continuous quality improvement in healthcare is to ensure that patients receive high-quality care consistently, and to assist with improving processes within a healthcare organization. These lead to benefits such as improving patient safety, enhancing efficiency, increasing patient satisfaction, cost-effectiveness, and promoting teamwork and collaboration. By focusing on quality improvement, healthcare providers can reduce errors, reduce inefficiencies, increase patient satisfaction, and improve the health outcomes of patients. The process of continuous quality improvement in healthcare involves a systematic, step-by-step approach to improving the quality of services and outcomes through continuous assessment, planning, implementation, and evaluation. The goal is to make ongoing, incremental improvements that lead to better patient care, increased safety, higher satisfaction, and more efficient use of resources.
