Table of Contents |
One helpful method for sorting out the sheer number of drugs on the market is by organizing them into different classifications. Most drugs are classified in two ways: therapeutic classification and pharmacologic classification.
EXAMPLE
The drug metoprolol has multiple classifications. Its therapeutic classification is antianginal because it relieves the chest discomfort associated with coronary artery disease. It also reduces blood pressure, so it has a second therapeutic classification and is also known as an antihypertensive.Medications are sometimes also classified based on their chemical structure.
EXAMPLE
Penicillin's (which are antibiotics) all have a similar structure.Once drugs are sorted into classifications, it is customary to utilize one drug within the class to compare to all the other drugs within that class. It becomes the “class representative,” known as the drug prototype. Using a drug prototype is helpful for an individual learning pharmacology because it makes learning much more manageable. It is also helpful in the clinical setting. Consider the situation of a healthcare provider who has administered the beta-adrenergic blocker metoprolol multiple times in the clinical setting and is quite familiar with its actions and side effects. When the health care provider orders the beta-adrenergic blocker (beta-blocker) atenolol, they know it will have a similar mechanism of action, side effects, and safety parameters as metoprolol. This is much easier for the student to learn than attempting to identify and learn every single drug made in the class.
Many different chemicals, substances, and drugs come under U.S. Drug Enforcement Administration (DEA) oversight (U.S. DEA, n.d.). In 1970, Congress passed the Controlled Substances Act, which led to the establishment of the DEA in 1973 and described the controls for manufacturing, distributing, and prescribing habit-forming drugs. This legislation not only categorized controlled substances based on their potential for abuse but also established drug schedules and provided drug treatment programs for those with addictions. All hospitals and pharmacies must keep records of drugs purchased and sold. Any health care provider with prescriptive authority must be registered with the DEA and given a unique DEA identifier that they must place on any controlled substance prescription.
Schedule I drugs have no medical use and a very high potential for abuse and physical/psychological dependency; therefore, most health care providers cannot issue prescriptions for those drugs, and pharmacies cannot fill those prescriptions. If research is being conducted with a Schedule I drug, applications and supporting documents have to be sent to the DEA for special permission. Schedule II, schedule III, and schedule IV drugs must have a medically sound reason for a prescription. Schedule V drugs are those with the lowest potential for misuse and dependency.
Cannabis has been classified as a Schedule I drug since the 1970 Controlled Substances Act. However, more than half of the states in the nation have decriminalized the substance, with some permitting medical usage and others both medical and recreational usage. As of May 2024, the Drug Enforcement Agency has recommended that cannabis be reclassified as a Schedule III drug, which would support wider medical usage and scientific research but not permit recreational usage on a national level. Formal reclassification will require additional steps.
The table below summarizes U.S. classifications.
| Drug Schedule | Example of Drugs in This Category | Therapeutic Use | Potential to Cause Physical or Psychological Dependency | Potential for Abuse |
|---|---|---|---|---|
| Schedule I | Heroin, lysergic acid diethylamide (LSD), peyote; see above regarding cannabis | No accepted medical use | High | The highest potential for abuse |
| Schedule II | Cocaine, methamphetamine, oxycodone, fentanyl, methadone, hydromorphone, mixed amphetamine salts, Adderall, Ritalin | Medical use | High | High |
| Schedule III | Acetaminophen with codeine, ketamine, anabolic steroids | Medical use | Moderate to low | Moderate to low |
| Schedule IV | Benzodiazepines such as alprazolam and diazepam; tramadol | Medical use; less abuse potential than Schedule III drugs and limited dependence liability | Low | Low |
| Schedule V | Atropine with diphenoxylate (Lomotil), pregabalin | General medical use | Low | Low |
Major classes of drugs include analgesics (pain relievers, antibiotics, other antimicrobials, cardiovascular drugs, endocrine and hormonal drugs, chemotherapy and cancer drugs, and nervous system drugs). In this section, you will learn more about each of these drug classes. Note that other categories can be included, and there is some overlap.
EXAMPLE
Non-steroidal anti-inflammatories (NSAIDs) are both pain relievers and anti-inflammatories.Analgesics are pain relievers. These are medications that relieve pain without causing a loss of consciousness.
A non-opioid analgesic refers to any pharmacologic agent that treats the symptoms of pain and does not involve activation of opioid receptors. These agents generally work by inhibiting cyclooxygenase (COX), a major pro-inflammatory enzyme that causes many signs and symptoms of inflammation, including redness, swelling, and sensitization of nociceptors (pain receptors), thereby increasing the transmission of painful signals to the brain. COX is also partly responsible for the pyrexia that occurs with infection, which is why many non-opioid analgesics that block the activity of COX also work as antipyretics to reduce fever. Non-opioid pain relievers include acetaminophen (also called paracetamol) and non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen.
Other non-opioid analgesics may serve as adjunctive agents for treating neuropathic sources of pain. These include antidepressant drugs (e.g., duloxetine, amitriptyline), antiseizure drugs (e.g., carbamazepine, pregabalin), and local anesthetics (e.g., lidocaine and bupivacaine). These are useful because they target the abnormal neuronal function that is the source of neuropathic pain.
Aspirin is a non-opioid analgesic that is also notable for its antiplatelet actions, so it can be used during myocardial infarctions to aid in maintaining coronary blood flow by inhibiting platelet aggregation.
Opioid agonists have been in use for thousands of years; these include opioid analgesics that involve the action of opioid receptors. Opioids originated from the opium poppy, Papaver somniferum, from which naturally occurring opioids such as heroin, codeine, and morphine are derived. Since the discovery of the potent analgesic effects of these medications, other opioids have been developed, including hydrocodone and oxycodone. The term opiate strictly refers to agents that come from the opium poppy (e.g., heroin, morphine), but is often used interchangeably with the term opioid. Opioid agonists are some of the most potent analgesics available and are used for the treatment of moderate to severe pain. However, opioids carry a risk for misuse and addiction that has led to one of the most notable public health crises to date, the opioid epidemic. Because of these risks, the DEA categorizes all opioids as controlled substances. Most opioids fall under the strict categorization of Schedule II (CII), meaning they have an acceptable medical use but are associated with a high risk for misuse and addiction.
Opioids produce many of their desired therapeutic effects and potentially life-threatening adverse effects via the opioid receptors, including the mu, delta, and kappa receptors. When activated, these receptors, located throughout the CNS, help modulate painful signals from peripheral tissues to alter pain perception and heighten the pain threshold. These same receptors are also known to cause many of the notable adverse effects of opioids, including the CNS and respiratory depression that can be seen in overdose. Opioid agonists also suppress the cough receptors in the brain and can be used as cough suppressants. However, due to the risk for misuse and addiction, opioid agonists are usually considered last-line treatments for cough.
Opioid analgesics, such as codeine, morphine, oxycodone, and fentanyl, are extremely effective when used to manage moderate to severe forms of pain but can cause potentially life-threatening CNS and respiratory depression when the recommended dosage is exceeded or when individuals use them along with other CNS depressants (e.g., alcohol). It is critical that agents are available to reverse the effects of opioids to avoid severe injury and potential death. Examples of these agents include naloxone hydrochloride and naltrexone hydrochloride.
Antibiotics are a group of drugs used specifically to treat infections caused by bacteria, either by directly killing the bacteria (bactericidal) or by suppressing their growth and multiplication (bacteriostatic). Antibiotics are some of the most commonly prescribed medications in the world; therefore, careful stewardship is necessary to avoid overuse, which can lead to antibiotic resistance.
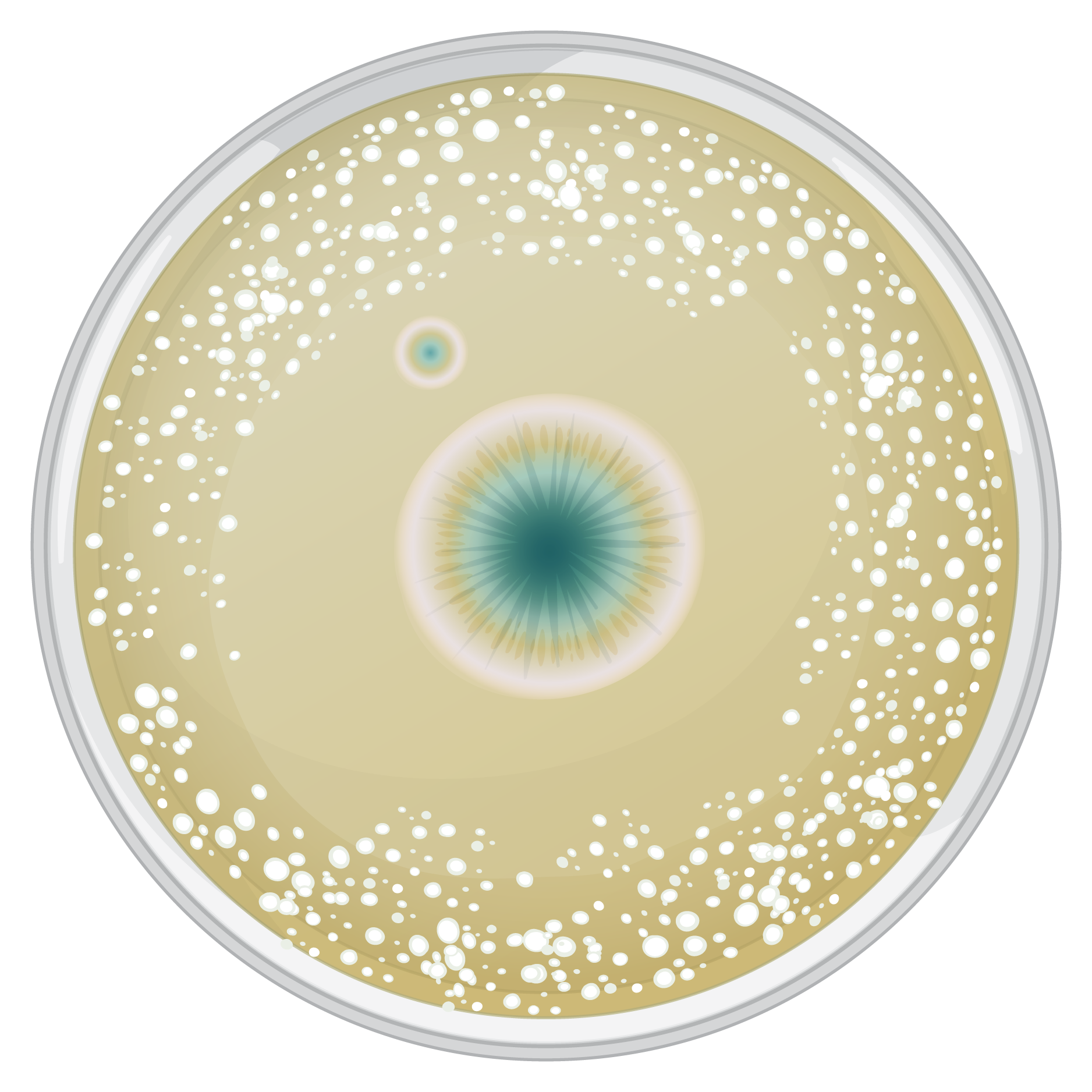
The figure above shows a petri dish of growth medium with bacterial colonies. In the middle, a fungus is growing. Note that there is a clear region around the fungus where it is inhibiting bacterial growth.
Antibiotic drug resistance (antibiotic resistance) is the process by which bacteria become less responsive to antibiotics over time. As bacteria are exposed to antibiotics, evolutionary changes occur, leading to the development of resistant strains that can withstand the antibiotic exposure and continue to thrive. These changes can include modification of antibiotic targets (e.g., bacterial DNA or proteins) so that the antibiotic can no longer affect them or the ability to remove a drug from the bacterial cell more effectively. Some bacteria are even able to share snippets of DNA that code for drug resistance with other bacteria.
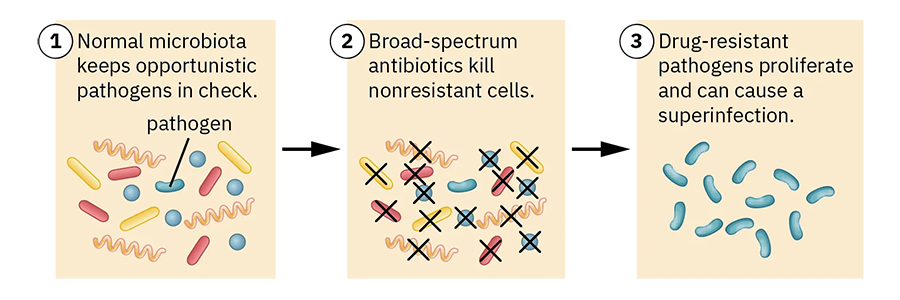
Antibiotic resistance is a major public health issue. Having fewer options to treat a client’s infection leads to worsened morbidity and mortality, higher health care costs, and the potential for bacteria to develop for which no effective treatment exists. Superinfections (a secondary infection on top of the first infection) can occur when the use of broad-spectrum antibiotics (effective against a wide range of microbes; Cambridge English Dictionary, n.d.) kills off normal nonpathogenic bacteria and leaves behind drug-resistant bacteria (which are antibiotic resistant), potentially producing a new infection that is more difficult to treat. Most antibiotic drug resistance occurs due to antibiotic overuse, both in humans and in agriculture. This is why health care providers should prescribe antibiotics only when there is a sufficient probability that the client has a bacterial infection.
The Step by Step and figure below summarize how superinfections occur.
Common antibiotic classes include:
- Penicillins – Amoxicillin, Penicillin G.
- Cephalosporins – Ceftriaxone, Cefuroxime.
- Macrolides – Erythromycin, Azithromycin.
- Tetracyclines – Doxycycline, Tetracycline.
- Fluoroquinolones – Ciprofloxacin, Levofloxacin.
This group includes antifungal medications, antiviral medications, and antiparasitic medications. Remember that bacterial cells are different from human cells; they are prokaryotic, whereas human cells are eukaryotic. The term parasite typically refers to eukaryotic pathogens (typically protists and parasitic worms), not bacteria. Because fungi and eukaryotic parasites are both eukaryotic, they have similarities to human cells. Viruses function by hijacking human cells. So developing treatments against viruses, fungi, and eukaryotic parasites has required different approaches to targeting bacteria.
EXAMPLE
Treatments for HIV target specific parts of the HIV life cycle (e.g., one type of HIV medication, integrase inhibitors, target an enzyme, integrase that inserts viral DNA into human DNA).For these reasons, medications to treat viral infections (antivirals), fungal infections (antifungals), and parasitic infections (antiparasitic medications) are varied.
EXAMPLE
Antifungal drugs may include fluconazole, clotrimazole, and amphotericin B.EXAMPLE
Antiviral drugs include acyclovir (herpes), oseltamivir (influenza), and remdesivir (COVID-19).EXAMPLE
Antiparasitic drugs include metronidazole (Giardia) and mebendazole (worm infections).
Cardiovascular drugs include medications that treat heart and blood vessel conditions. Common conditions include drugs to maintain a normal heart rhythm/correct dysrhythmias, antihypertensive drugs, antianginal drugs (to treat angina), heart failure drugs, lipid lowering drugs, drugs to reduce clotting, and drugs to use in cardiac emergencies.
Examples of some of these drugs include beta blockers (-olol), such as metoprolol and propranolol, which block receptors to slow; ACE inhibitors (-pril), such as lisinopril and enalapril; calcium channel blockers, such as amlodipine and nifedipine (which relax blood vessels; Mayo Clinic staff, 2025); diuretics (water pills) that increase urine output, such as furosemide and hydrochlorothiazide; anticoagulants that prevent clot formation, such as warfarin and heparin); and thrombolytics that dissolve blood clots, such as alteplase and streptokinase.

The figure above shows propranolol tablets. Note that the 10 mg and 20 mg pills are different colors. This helps to reduce the risk that someone will take the wrong dose without noticing (e.g., Stegemann, 2017). As you learn about different medications, you will see a variety of safety mechanisms like this. Remember that propranolol is a beta blocker, meaning that it blocks certain receptors; this has effects such as lowering heart rate and blood pressure (Cleveland Clinic, 2025a).
Many types of medications are used to treat endocrine conditions.
EXAMPLE
There are many types of diabetes medications, such as rapid-acting insulin (lispro) and long-acting insulin (glargine). Oral hypoglycemics include metformin, which is a first-line treatment for type 2 diabetes.Other endocrine conditions can be treated with pharmaceuticals.
EXAMPLE
Levothyroxine treats hypothyroidism and methimazole treats hyperthyroidism.Corticosteroids, such as prednisone and dexamethasone, are used for inflammation and autoimmune conditions, among other uses.

The figure above shows hydrocortisone cream, a steroid used to treat skin irritation (Cleveland Clinic, 2025b).
You have already learned about a variety of cancer drugs and treatments. Some common classes include alkylating agents (e.g., cyclophosphamide), antimetabolites such as methotrexate and 5-fluorouracil (5-FU); and monoclonal antibodies such as trastuzumab (used for breast cancer).
Alkylating agents kill cancer cells by cross-linking DNA, which prevents cell division in a manner that can lead to toxicity within the cell or unbalanced growth, both of which can cause cell death. They work most effectively on slower-growing tumors with a slowed mitotic rate.
Antimetabolite chemotherapies are a group of drugs that prevent cancer cell growth by imitating metabolites, which are substances necessary for tumor cell growth. Cancer cells use these substances, which, once inside the cell, prevent DNA replication. Without these substances, cells die.
Monoclonal antibodies are a type of biologic drug. They are engineered in the laboratory to target and bind to specific molecules or cells in the body. They are designed to mimic the immune system’s natural ability to recognize and attack foreign invaders, such as bacteria, viruses, and cancer cells. These antibodies can be used to block certain pathways involved in disease processes, modulate immune responses, or deliver drugs directly to specific cells or tissues.
Chemotherapy may be given for many different reasons. Often, it is given as a curative measure to eradicate all malignant cells. However, cure is not always realistic. When a cure is not attainable, chemotherapy can be used to decrease tumor size and prevent metastasis, and sometimes it may be used for palliation and symptom control. Differing regimens of chemotherapy are used for varying client needs.
The table below summarizes the types of chemotherapy.
| Type of Chemotherapy | Description |
|---|---|
| Adjuvant therapy | Given after initial treatment with surgery to destroy leftover cells |
| Neoadjuvant therapy | Initial treatment given to shrink the cancer before surgery |
| Salvage therapy | Second-line therapy given when first-line therapy is unsuccessful |
| Targeted therapy | Given to selectively kill cancer cells without harming normal cells |
| Biologic therapy | Used to enable the immune system to better kill cancer cells |
Nervous system drugs can include drugs to treat a wide variety of conditions, including psychiatric conditions. You learned about many of these in lessons on mental health. Nervous system drugs include medications to treat myasthenia gravis, Alzheimer’s disease, epilepsy, migraine, and intracranial emergencies.
There are multiple types of antidepressants. These include selective serotonin reuptake inhibitors (SSRIs), such as fluoxetine and sertraline, as well as tricyclic antidepressants (TCAs), such as amitriptyline.
There are also several types of antipsychotics. First-generation antipsychotics include haloperidol. Second-generation (atypical) antipsychotics include risperidone and olanzapine.
Anxiolytics include benzodiazepines, which have names ending in –pam or –lam. Examples include diazepam and lorazepam.
Finally, antiseizure drugs, which help to prevent seizures, include phenytoin, valproate, and levetiracetam (Cleveland Clinic, 2023).
Source: THIS TUTORIAL HAS BEEN ADAPTED FROM “Pharmacology for Nurses” BY Tina Barbour-Taylor, Leah Mueller (Sabato), Donna Paris, Dorie Weaver AT OpenStax. ACCESS FOR FREE AT https://openstax.org/books/pharmacology/pages/1-introduction. LICENSING: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.
REFERENCES
Calcium Channel Blockers. (2025, March 29). Mayo Clinic staff. Calcium channel blockers - Mayo Clinic
Stegemann, S., Riedl, R., & Sourij, H. (2017). Identification of different shapes, colors and sizes of standard oral dosage forms in diabetes type 2 patients-A pilot study. International Journal of Pharmaceutics, 517(1-2), 112–118. doi.org/10.1016/j.ijpharm.2016.11.066
Beta Blockers. (2025a, April 14). Cleveland Clinic. Beta-Blockers: Uses & Side Effects
American Chemical Society International Historic Chemical Landmarks. Discovery and Development of Penicillin. www.acs.org/content/acs/en/education/whatischemistry/landmarks/flemingpenicillin.html.
Broad-Spectrum Antibiotic. (n.d.). Cambridge English Dictionary. BROAD-SPECTRUM ANTIBIOTIC definition | Cambridge English Dictionary
Hydrocortisone Cream, Lotion, Ointment, or Solution. (2025b). Cleveland Clinic. Hydrocortisone Cream: Uses & Side Effects
Antiseizure Medications (Formerly Known as Anticonvulsants). (2023, February 3). Cleveland Clinic. Antiseizure Medication (Anticonvulsants): What It Is & Uses