Table of Contents |
Blood transfusions in humans, in which blood is transferred from one person (a donor) to another (a recipient), were risky procedures until the discovery of the major human blood groups by Karl Landsteiner, an Austrian biologist and physician, in 1900. Until that point, physicians did not understand that death sometimes followed blood transfusions, when the type of donor blood infused into the patient was incompatible with the patient’s own blood. Blood groups are determined by the presence or absence of specific marker molecules (one type of cell surface marker) on the plasma membranes of erythrocytes. These markers are antigens, meaning that the immune system can recognize them and respond to them. With the discovery of erythrocyte antigens, it became possible for the first time to match patient-donor blood types and prevent transfusion reactions and deaths.
You already learned a little bit about antigens. Antigens are substances that may trigger a defensive response from leukocytes of the immune system if the body does not recognize the antigen as belonging to "self." Antigens are generally large proteins but may include other classes of organic molecules, including carbohydrates, lipids, and nucleic acids.
Following an infusion of incompatible blood, erythrocytes with foreign antigens appear in the bloodstream and trigger an immune response. Proteins called antibodies (immunoglobulins), which are produced by certain B lymphocytes called plasma cells, attach to the antigens on the plasma membranes of the infused erythrocytes and cause them to adhere to one another.
The ABO blood types are genetically determined for every individual based on the presence or absence of specific antigens called “A” or “B” on the individual’s red blood cells. These ABO antigens are glycoproteins.
When an individual has a particular antigen, their immune system is designed to recognize the antigen as self and will not attack it. Unfamiliar antigens are not self, and the immune system will typically recognize these antigens are foreign and stimulate an immune response.
EXAMPLE
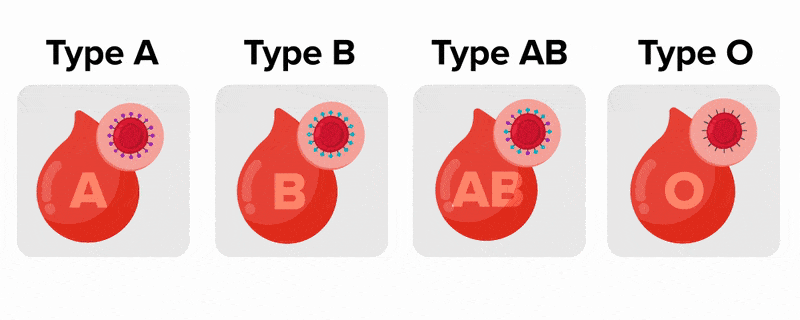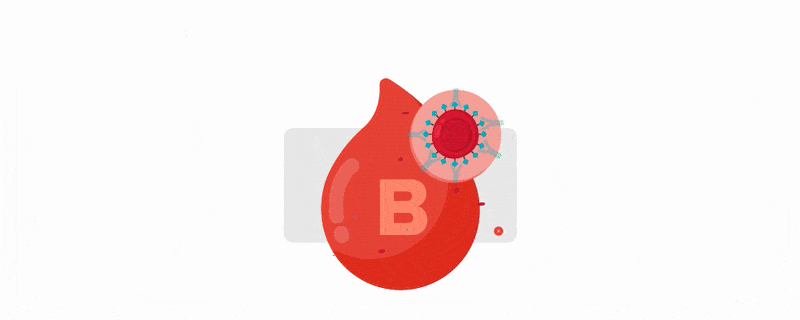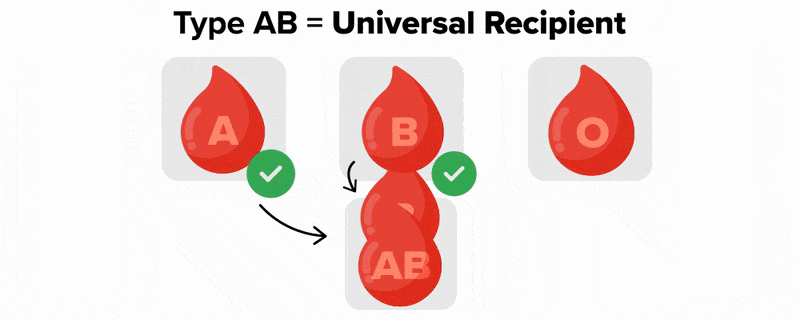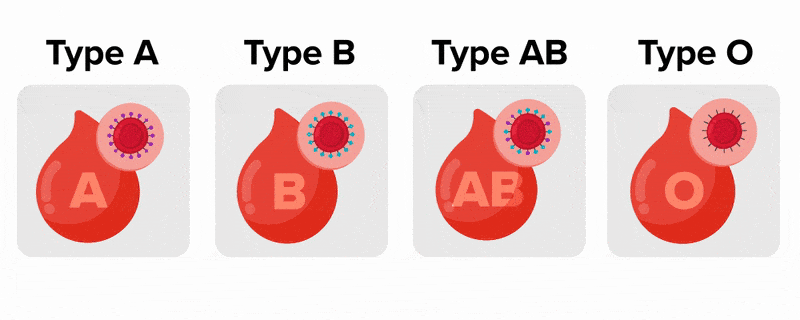
An individual with Type A blood has an A antigen on their RBC but has antibodies to the B antigen in their blood.People whose erythrocytes have A antigens on their erythrocyte membrane surfaces are designated blood type A, and those whose erythrocytes have B antigens are blood type B. People can also have both A and B antigens on their erythrocytes, in which case they are blood type AB. People with neither A nor B antigens are designated blood type O. ABO blood types are genetically determined.
Because of the way that the immune system recognizes and responds to unfamiliar antigens, receiving incompatible blood could lead to a life-threatening reaction. If an individual requires a blood transfusion, it is vital for the donated blood to be compatible with their blood type to avoid this type of reaction.
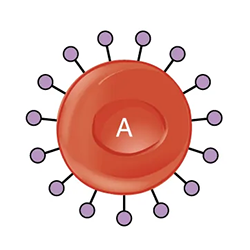
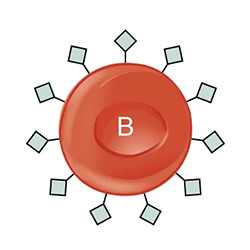
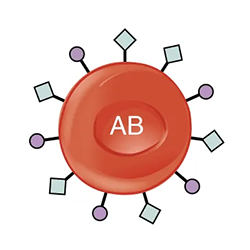
The table below shows the different blood types and associated antigens and antibodies, as well as their compatible blood types. This figure focuses only on ABO blood types; note that other factors must be considered in selecting blood for a transfusion. Note that type A blood has a specific antigen on the surface of the erythrocytes, while type B blood has a different antigen on the surface of its erythrocytes. Type AB blood has both of these antigens, type A and type B, while type O has neither of these antigens. In the plasma, type A blood has anti-B antibodies, type B blood has anti-A antibodies, type AB blood has neither type A nor type B antibodies, and type O blood has both type A and type B antibodies. This allows the body to recognize blood of a different type, leading to a reaction. If antibodies are present to an antigen on blood cells, a reaction occurs. Therefore, an individual with type A blood can only receive A or O blood; an individual with type B blood can only receive B or O blood; an individual with type AB blood is a universal recipient that can accept any of these blood types, and an individual with type O blood can only receive type O blood but is a universal donor.
| A | B | AB | O | |
|---|---|---|---|---|
| Red Blood Cell Type |
|
|
|

|
| Antibodies in Plasma |
 Anti-B |
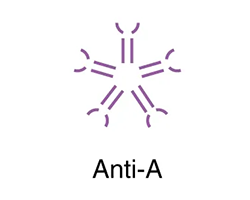 Anti-A |
None |
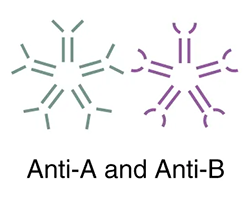 Anti-A and Anti-B |
| Antigens in Red Blood Cell |
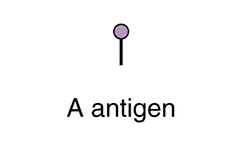
|
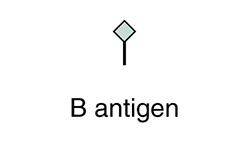
|
|
None |
| Blood Types Compatible in an Emergency | A, O | B, O |
A, B, AB, O (AB⁺ is the universal recipient) |
O (O is the universal donor) |
The animation below shows what happens when blood of the same or different types is combined. Note which combinations cause coagulation as antibodies bind to antigens on blood cells.
In addition to the A, B, AB, or O blood type, individuals may have another antigen on their red blood cells called Rh factor.
The Rh blood group is classified according to the presence or absence of this second erythrocyte antigen, identified as Rh. (It was first discovered in a type of primate known as a rhesus macaque, which is often used in research, because its blood is similar to that of humans.) Although dozens of Rh antigens have been identified, only one, designated D, is clinically important. Those who have the Rh D antigen present on their erythrocytes—about 85 percent of Americans—are described as Rh positive (Rh⁺), and those who lack it are Rh negative (Rh⁻).
Note that the Rh group is distinct from the ABO group, so any individual, no matter their ABO blood type, may have or lack this Rh antigen. When identifying a patient’s blood type, the Rh group is designated by adding the word positive or negative to the ABO type. Individuals who have the antigen on their RBCs are described as Rh positive (Rh⁺), and those who lack the antigen are described as Rh negative (Rh⁻).
When identifying a patient’s blood type, the Rh factor is designated by adding the word positive or negative to the ABO type.
EXAMPLE
A positive (A⁺) means A blood type with the Rh antigen present, and AB negative (AB⁻) means AB blood type without the Rh antigen.Individuals receiving blood transfusions must receive donated blood that matches their Rh type, or a serious, life-threatening reaction will occur.
During pregnancy, the fetus can be significantly affected if the mother has a different Rh factor. If an Rh⁻ mother conceives a Rh⁺ baby, her Rh antibodies can cross the placenta and destroy the fetal RBCs. This condition is known as hemolytic disease of the newborn and can be so severe that, without treatment, the fetus may die in the womb or shortly after birth. A medication known as RhoGAM can temporarily prevent the development of Rh antibodies in an Rh- mother, thereby averting this potentially serious disease for the fetus if it is Rh⁺. RhoGAM is administered to Rh- mothers during weeks 26−28 of pregnancy and within 72 hours following birth.
Note that you may sometimes see the term Rh D antigen. There are actually several types of Rh antigens, but Rh D is the one you will hear about regularly with respect to blood donation. The presence or absence of the Rh D antigen is what determines if your blood type is Rh positive or Rh negative, although other Rh antigens are also considered for compatibility as needed. The reason is that the Rh D antigen produces the strongest immune response (NHS, n.d.).
SOURCE: THIS TUTORIAL HAS BEEN ADAPTED FROM (1) “OPEN RN | MEDICAL TERMINOLOGY – 2E” BY ERNSTMEYER & CHRISTMAN AT OPEN RESOURCES FOR NURSING (OPEN RN). (2) "MEDICAL TERMINOLOGY" BY HOBBS & CASTEEL AT PHOENIX COLLEGE NURSING. ACCESS FOR FREE AT WTCS.PRESSBOOKS.PUB/MEDTERM/ AND OPEN.MARICOPA.EDU/MEDICALTERMINOLOGY/FRONT-MATTER/INTRODUCTION/. LICENSING: CREATIVE COMMONS ATTRIBUTION 4.0 INTERNATIONAL.
REFERENCES
The Rh System. (n.d.). NHS Blood and Transplant. The RH system - NHS Blood Donation